

How to Start a Healthcare Consulting Business
Below you will learn the key steps to starting a healthcare consulting business.
Download the Ultimate Consulting Business Plan Template
10 Steps to Starting a Healthcare Consulting Business
1. conduct market research to determine demand.
An important step to starting a healthcare consulting business is conducting market research. To begin, you must learn what services your clients want and how much they are willing to pay for them. There are two ways you can go about conducting this research:
- Survey your target market . This can be done through online surveys, focus groups, or interviews with potential clients.
- Perform a competitive analysis . This involves studying your competition and understanding the consulting services they offer, as well as what prices they charge.
Once you have analyzed the survey data, determine which types of businesses are likely to hire you and how much they are willing to pay. Use this information to set your consulting prices.
2. Name Your Healthcare Consulting Firm
Once you have analyzed your market and determined what services clients want, it’s time to name your business. While naming a business can be difficult, there are a few rules of thumb to keep in mind:
- Keep it Short : Your business name needs to be short enough for clients to remember and say.
- Keep it Relevant : Your business name should be relevant to the healthcare consulting services you offer and your ideal client’s needs.
- Keep it Memorable : Using clever ideas and words, help your audience connect with your business.
- Focus on Your Target Audience : Make sure that whoever sees or hears your company name understands who you are targeting as clients.
Read our article about choosing the right business name .
3. Choose Your Business Structure and Set-Up Your Company’s Legal Entity
As with any business, the type of legal entity you set up is critical. After all, you want your company to be treated as a separate entity, not just an extension of yourself. There are several types of structures in which you can start your healthcare consulting company. Three popular options are sole proprietorship, S-corporation and LLC (limited liability company).
- Sole Proprietorship : A sole proprietorship is one in which the business and the owner are considered to be one entity. Therefore, you are personally responsible for all debts and liabilities your healthcare consulting firm may incur. One benefit of this type of structure is that it’s easy to set up and there are no formal filings required.
- S-Corporation : An S corporation is a type of C Corporation that was designed by the IRS to help small corporations minimize their paperwork while still gaining many of the tax benefits of incorporating. It also offers protection for business owners in case of lawsuits and other liabilities.
- Limited Liability Company (LLC) : An LLC is a structure in which the company is considered a separate legal entity from its owners. This means that the company is responsible for its own debts and liabilities. This type of structure offers protection for business owners in case of lawsuits.
Read our article comparing the most common consulting business structures .
4. Write a Healthcare Consulting Business Plan
A business plan is a document that outlines your business goals, strategies, and how you plan to achieve them. For a healthcare consulting company, your business plan should include the following:
- Business Description : Describe what your company does, who your target market is, and how you will differentiate yourself from the competition.
- Industry & Market Analysis : Detail your research on the healthcare industry and what consulting services clients are most likely to want.
- Financial Plan : Outline your estimated income and expenses for the next three to five years.
Other sections of your plan will answer other key questions such as the following:
- What are your areas of expertise?
- What services can you offer your clients?
- Who is your target audience?
- How will you differentiate yourself from the competition?
Your business plan should also include several sections that detail your company’s history, current financial situation, and future goals. These sections will allow an investor to learn more about your company before they commit to investing in it.
Read our article about how to write a consulting business plan .
5. Apply for a Business License and Necessary Health Licenses
You must register your healthcare consulting company as a legal entity with the state in which you plan to do business.
To file your business with the state, obtain the necessary forms from the Secretary of State’s website or local County Clerk’s office. You will be required to pay a small fee for filing your business with the state.
Registering with the federal government may or may not be required. You can register your business on the federal level by obtaining an Employer Identification Number (EIN) from the IRS.
Read our article about obtaining the proper consulting business licenses .
6. Determine Your Budget & Apply for Funding as Needed
As with any business, you will need to use your own capital to finance the initial stages of your health consulting business. Your budget may also include several other costs including marketing expenses and the salary you wish to pay yourself.
After determining how much money you will invest in starting your business, review some options for financing your business. Here are several financing options that may be available to you:
- SBA Loans : The Small Business Administration (SBA) is a government agency that provides financial assistance to small businesses in the U.S.
- Bank Loans : Many small business owners are able to secure loans from their local banks. Often, you can borrow money for any purpose that relates to the growth of your company.
- Friends and Family : You can consider getting loans and/or equity investments from friends and family members..
- Angel investors : Angel investors may provide debt or equity funding to you.
Read our article about the costs associated with starting a consulting business to help you determine if funding is needed.
7. Get the Technology & Software Needed to Run Your Healthcare Consulting Company Efficiently
As a healthcare consulting firm, you will need different types of technology to complete projects and keep track of your company’s operations. To simplify the process of starting a consulting business, we’ve provided a list below detailing some items that you’ll need:
Computers : Even if most of your work is done remotely with clients on the other side of the country or world, you will need at least one computer that is dedicated to your healthcare consulting company.
Software : Software is an essential component of any consulting business. The right software can help you manage projects, track expenses, and communicate with clients more effectively.
Here are some popular software platforms that may be beneficial to your business:
- Microsoft Office : This software suite includes a variety of applications that can help you manage your company, including Word, Excel, and PowerPoint.
- QuickBooks : This software is designed for small businesses and can help you track income and expenses, create invoices, and manage payroll.
- Basecamp : This project management software can help you manage multiple projects simultaneously and keep track of deadlines and milestones.
- Gmail : Google’s email platform offers several features that can be helpful for consulting firms, including the ability to access the same email from multiple devices.
- CRM : Customer relationship management software can help you track customer communication, manage leads, and create reports that detail your sales activities.
Additional software specific to healthcare consulting may include:
- EHR software : This software is used by healthcare providers to manage patient data.
- HIPAA compliance software : This software helps organizations comply with the Health Insurance Portability and Accountability Act (HIPAA).
- EMR software : This software is used by healthcare providers to manage patient information and track medical appointments.
Read our article about the technology and software you need to run a consulting business .
8. Market Your Healthcare Consulting Firm to Potential Clients
Once you’ve established your healthcare consulting company, the next step is to market it to potential clients.
Here are some common marketing strategies used for healthcare consulting firms:
- Website : A website is an essential component of any marketing strategy. It provides potential clients with information about your company, including the consulting services you offer and the team of professionals who work for you.
- Online marketing : Marketing your business online, such as through a business website and pay-per-click and/or social media marketing, can help you reach a larger audience looking for your services.
- Direct Mail : Direct mail is a traditional marketing strategy that can be used to reach potential clients. You can send flyers, brochures, or letters to potential clients that provide information about your company and the services you offer.
- Trade Shows : Trade shows are a great way to connect with potential clients in person. You can exhibit at healthcare-focused trade shows or attend trade shows in other industries to reach potential clients who may need your services.
- Networking Events : Networking events are a great way to meet potential clients and connect with other professionals in your industry. Attending events such as Chamber of Commerce meetings or breakfast meetings can help you build relationships with potential clients.
You should also consider ways to incentivize potential clients to choose you over another healthcare consulting firm. Some incentives that work well include:
- Lower rates : Many healthcare consulting firms offer lower rates on their consulting services to attract new clients.
- Discounts on services : Offering discounts on certain projects may help you win bids against other healthcare consulting firms.
- Free consultation : Providing potential clients with a free consultation can help them determine if your company is the best one for their needs.
Learn more about how to market your consulting business .
9. Establish a Price Structure and Billing System
There are a few factors to consider when establishing your price structure:
- Hourly rates : Charging by the hour is a common way to price consulting services. This allows clients to budget for your services and gives you the flexibility to charge more for complex projects.
- Project rates : Charging a flat fee for a project can be beneficial for both the client and the consultant. It ensures that clients know what they are paying up front, and it allows healthcare consultants to charge more for more complex projects.
- Retainers : A retainer is a set amount of money that the client pays upfront for consulting services. This can be a good option for clients who need regular consulting services.
No matter which pricing structure you choose, be sure to clearly communicate it to your clients. Additionally, have a detailed invoice template that includes all the healthcare services you provided so the client knows exactly what they are paying for.
10. Manage Client Relationships and Deliver Projects
After finding new clients and marketing your healthcare consulting business, you should begin delivering the projects and getting paid. This means managing client relationships and making sure that clients are happy with your work. Some of the ways to manage relationships with your healthcare clients include:
- Regular communication : Make sure to stay in touch with your clients, even if there is not a lot of work to be done. By keeping in touch regularly, you can ensure that they know you are available and that they will be the first ones you contact when new projects arise.
- Project updates : Keep your clients updated on the progress of each project. This can be done in a variety of ways, such as through emails, reports, or presentations.
- Frequent contact : In some cases, it may be necessary to contact your clients more often than usual. If there are major changes to the project, for example, or if you need additional information from them.
Delivering projects on time and within budget is essential for a healthcare consulting business. It can be beneficial to create a project management plan that outlines how each project will be completed. This will help ensure that all deadlines are met and that the client is happy with the final product.
Learn more about how to effectively manage client relationships .
Starting a Healthcare Consulting Business FAQs
Why start a healthcare consulting business.
Healthcare consulting is a growing industry, and there are many reasons why starting a healthcare consulting business might be the right move for you. Some of the benefits of owning a healthcare consulting company include:
- You get to be your own boss
- The work is interesting and varied
- There is potential for high income
- You can help people
What is Needed to Start a Healthcare Consulting Business?
There are a few things you will need in order to start a healthcare consulting company. These include:
- A clear understanding of the healthcare industry
- Marketing materials
- An office space or home office
- Healthcare consulting software
What are Some Tips for Starting a Healthcare Consulting Company?
The following tips can help you to start a healthcare consulting company:
- Do your research : Before you launch your business, be sure to do your research and understand the industry inside and out. This will help you to develop a strong strategy and provide valuable services to your clients.
- Establish relationships with healthcare professionals : One of the best ways to grow your business is to establish relationships with healthcare professionals. Attend conferences, meet-ups, and other events where you can network with these individuals.
- Offer a range of services : In order to be successful, it is important to offer a variety of services to your clients. This will help you to meet the needs of a wider range of clients.
- Keep up with industry changes : The healthcare industry is constantly evolving, so it is important to keep up with the latest changes. This will help you to stay ahead of the competition and provide valuable services to your clients.
- Market your business : Marketing is key when it comes to a successful healthcare consulting company. Be sure to create a strong marketing strategy and use a variety of marketing channels to reach your target audience.
Limited time: Try B12 $1/mo for 3 months.
Build an AI website in 60 seconds
AI generates your personalized website instantly with built-in scheduling, payments, email marketing, and more.

How to start a health care consulting business

Are you interested in becoming a healthcare consultant? Do you want to start your own healthcare consulting business?
Healthcare consulting is a fast-growing industry that requires individuals with strong analytical and problem-solving skills, healthcare expertise, and business acumen. In the US, there are over 35,000 healthcare consultants. As a healthcare consultant, you'll work with healthcare providers, insurance companies, government agencies, and other stakeholders. You’ll help them improve their operations, reduce costs, and provide better healthcare to patients.
This blog post will guide you on how to start your own healthcare consulting business. We’ll provide you with the guidance and resources you need to succeed in healthcare consulting. Let’s get started!
Starting a healthcare consulting business: an overview
Starting a healthcare consulting business can be a fulfilling and exciting career. But it can also be challenging. The healthcare industry is constantly evolving. And there’s always a need for experienced consultants who can help navigate the changes and provide valuable insights.
Whether you are a recent graduate or an experienced healthcare professional looking for a new challenge, starting a healthcare consulting business is a viable option. With the high demand for healthcare consultants, the industry offers many opportunities for growth and career advancement.
Understanding healthcare consulting
Healthcare consulting is a rapidly growing industry that helps healthcare organizations solve complex problems and improve their overall performance.
What is healthcare consulting?
Healthcare consulting involves helping healthcare organizations improve their operations, financial performance, and patient care. Healthcare consultants work with hospitals, clinics, physician practices, insurance companies, and other healthcare organizations. They provide a wide range of services, including strategic planning, process improvement, revenue cycle management, and health information technology implementation.
Why healthcare consulting is a growing industry
Healthcare consulting is a growing industry due to the increasing complexity of the healthcare landscape. Healthcare organizations are facing unprecedented challenges, including rising costs, evolving regulations, and changing patient needs. Healthcare consultants help organizations navigate these challenges by providing expert advice and innovative solutions.
Benefits of being a healthcare consultant
There are many benefits to being a healthcare consultant. One of these is having a fulfilling career with opportunities for growth and advancement. Healthcare consultants can make a significant impact on the healthcare industry by helping organizations improve patient care and reduce costs. Additionally, healthcare consulting provides a rewarding work-life balance, with opportunities for remote work and flexible schedules. Finally, healthcare consulting offers competitive salaries and benefits packages, with opportunities for professional development and continuing education.
How to become a health care consultant
Becoming a healthcare consultant requires several qualifications, including education, experience, and essential skills. Below are the requirements and steps on how to become a healthcare consultant.
Education and certifications needed
One of the basic requirements for a healthcare consultant is a bachelor's degree in healthcare management or other related programs. A master’s degree in healthcare administration, health services administration, or business administration is preferred by many employers. However, a bachelor’s degree in a related field is also acceptable.
To advance your healthcare consultant career, certifications are important. Certifications like Certified Management Consultant (CMC) or Professional in Healthcare Risk Management (CPHRM) demonstrate your expertise and knowledge in the field.
Essential skills for healthcare consultants
Healthcare consulting requires several skills to be successful in the industry. Some essential skills you should develop include communication skills, analytical skills, and problem-solving skills. Strong interpersonal and management skills are also important in this profession. The ability to work with different teams and clients is also necessary.
How to get into healthcare consulting
Getting into healthcare consulting requires several steps. You can work in healthcare first, gain experience, and develop your skills. You can also do internships, attend networking events, and take part in relevant programs or workshops. For those who already have experience in healthcare but want to switch to consulting, it is beneficial to obtain relevant certifications and qualifications.
Finding healthcare consultant jobs
Job opportunities for healthcare consultants can be found in various settings. These include hospitals, clinics, consulting firms, and health insurance companies. Networking, building your professional profile, and attending career fairs can help you find job opportunities. Online job search engines and professional association websites like the National Society of Certified Healthcare Business Consultants (NSCHBC) can also help you find job opportunities.
Starting your healthcare consulting business
Starting a healthcare consulting business requires careful planning and preparation. Here are the key steps to get your healthcare consulting business off the ground.
Creating a business plan
A business plan outlines your business goals, target audience, marketing strategies, and financial projections. Your business plan should also include a detailed analysis of your competition. It should include a plan for how you will differentiate your business from theirs. Developing a comprehensive plan will help you stay focused as you start your business.
Legal considerations
Before starting your healthcare consulting business, consider its legal aspects. This includes registering your business, obtaining any necessary licenses and permits, and getting liability insurance. You will also need to decide on a legal structure for your business. For instance, you could opt for a sole proprietorship, partnership, or limited liability corporation (LLC). Seeking the advice of a lawyer or accountant can help you navigate these important legal considerations.
Marketing your services
Marketing your healthcare consulting services is crucial for attracting potential clients. Your marketing strategy should include creating a website, networking with other healthcare professionals, attending events and conferences, and utilizing social media platforms. You should also consider creating a referral program and asking satisfied clients for testimonials. By promoting your business effectively, you can establish your credibility and attract more clients.

Finding your niche
As a healthcare consultant, you can focus on a specific area of expertise. For instance, healthcare technology, hospital management, or public health. By specializing in a particular niche, you can differentiate yourself from other competitors and target specific clients. However, you must conduct market research. You must ensure there’s a demand for your services in your chosen niche. By identifying your niche, you can tailor your services. This way, you can meet your target audience’s specific needs and challenges.
Growing your healthcare consulting business
Imagine your healthcare consulting business continues to expand. In that case, you must have a plan in place for growth.
Expanding your services
One way to grow your healthcare consulting business is to expand your services. This can be done by offering new areas of expertise, or by branching out into new markets or geographies. Conduct market research to identify areas of potential growth, and invest in the necessary resources to develop new services.
Building your team
As your business grows, it may become necessary to build a team of consultants to handle increased demand. When hiring new talent, focus on finding individuals with the skills and experience needed to support your business goals. Develop a strong onboarding and training program. This is to ensure that new team members are fully integrated into the company culture.
Managing your finances
Have systems in place for tracking expenses, invoicing clients, and managing cash flow. Consider hiring a financial advisor or accountant. They’ll be able to help you manage your finances effectively.
Starting and growing a healthcare consulting business takes dedication, hard work, and a commitment to excellence. By understanding the industry, developing a unique niche, and focusing on delivering exceptional services, you can build a successful consulting practice. With the right strategies in place for growth and financial management, you can create a fulfilling career while helping others to improve their healthcare organizations.
Advancing your career in healthcare consulting
As a healthcare consultant, the career possibilities are endless. You can advance your career in several different directions. This all depends on your interests and expertise.
Public health consulting
Public health plays an essential role in ensuring the overall health of communities and populations. As a public health consultant, you will work with organizations and government agencies. You will help them identify health problems and implement solutions to improve the health of the public. This can include initiatives such as disease prevention, health promotion, and policy development.
Physician consulting
Physician consulting involves working with healthcare providers to improve patient care and outcomes. This can involve identifying inefficiencies in healthcare systems and streamlining processes. This can also be implementing new technologies to improve patient care and their healthcare facilities. Physician consulting can also involve working with healthcare organizations to develop new models of care that can improve patient outcomes.
Healthcare IT consulting
Healthcare organizations are becoming increasingly reliant on technology to improve patient outcomes and streamline workflows. Health IT consulting involves working with healthcare organizations to implement new technologies. For instance, electronic health records, telemedicine, and patient monitoring systems. As a health IT consultant, you will use your expertise to help healthcare organizations leverage technology to improve patient care and outcomes.
Top healthcare certifications to have
Obtaining healthcare certifications can help you stand out in a crowded job market and demonstrate your expertise in a particular area. Some of the top healthcare certifications to have include the Project Management Professional (PMP) certification and Certified Health Education Specialist (CHES) certification. You may also go for the Certified Professional in Healthcare Information and Management Systems (CPHIMS) certification.
Advancing your career in healthcare consulting requires dedication and expertise. It requires a willingness to adapt to changing healthcare trends. By considering these different paths, obtaining relevant certifications, and gaining specialized knowledge, you can grow your career and become a leader in the field.
Promote your healthcare consulting business with a solid website
Get your healthcare consulting business off the ground and make it more visible to potential clients with a solid online presence. Through a professional website, you can get your business in front of more customers, expanding your visibility and reach.
With B12, you can create, design, and launch a professional website in 30 days or less. Our AI website builder enables you to generate your site and crucial web pages complete with your branding. Choose from a vast library of templates, colors, fonts, and images specifically geared for the industry you’re in.
B12 is the all-in-one platform that helps professional service small businesses launch an online presence with tools like payments , scheduling, email marketing, and contracts. See your new site for free in 60 seconds to start winning, attracting, and serving clients in no time.
Attract, win, and serve more clients
Receive helpful resources directly to your inbox to help you succeed online.
Related posts

Spend less time on your website and more time growing your business
Let B12 set up your professional online presence with everything you need to attract, win, and serve clients.
How we help clients in your region
Middle east & africa.

McKinsey Health Institute

Center for US Healthcare Improvement

Business Building in Healthcare
Featured capabilities.

Healthcare Analytics

Actuarial Analytics

Nebula platform
Creating value beyond the hype.

Shubham Singhal
Senior partnerdetroit.

Drew Ungerman
Senior partnerdallas, featured insights.
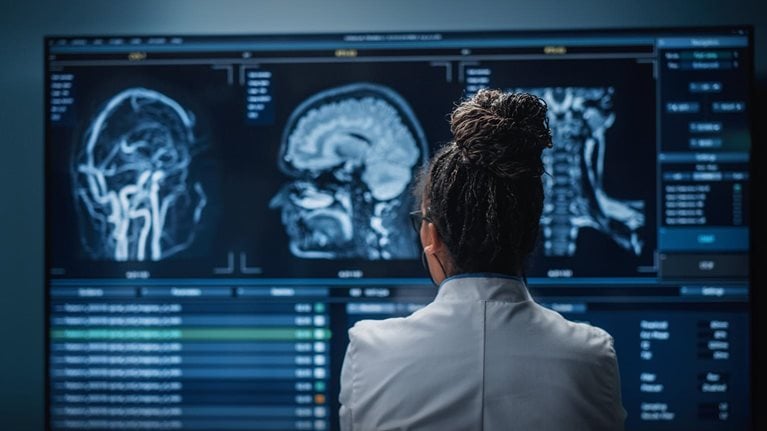
The Future of Healthcare

Tackling healthcare’s biggest burdens with generative AI

Reimagining the nursing workload: Finding time to close the workforce gap

The future of Medicare Advantage
New at mckinsey blog.

Responding to COVID-19: Adi Kumar
Related practices.

Public & Social Sector
Life Sciences

McKinsey Digital

Financial Services

McKinsey’s work for social sector, healthcare, and public entities
Connect with our healthcare practice.
Healthcare Consulting: What It Is & How to Succeed in It
Published: June 19, 2023
It’s surprising how the healthcare industry is complex and yet rewarding at the same time. Just one sector — for example, healthcare consulting — can unlock great opportunities. But what is healthcare consulting, and if it's so good of a career option, how can you become a healthcare consultant?

With constant developments in treatments, medication, and technology, healthcare organizations have much to keep track of — and doing so thoroughly and professionally is vital to their success and patients' health. But it isn’t as easy as it sounds. That’s where a healthcare consultant can take the responsibility to help these organizations balance patient care with patient experience.
This post will teach you why healthcare consulting is a job with a greater purpose, what options you have, and how to start working in the field.

Table of Contents
- What is healthcare consulting?
Types of Healthcare Consulting
Why healthcare consulting, how to get into healthcare consulting.
As the primary job of healthcare organizations is to cure their patients, they can fall behind in many areas when ignored. And since healthcare is a competitive industry, they can’t afford that.
Therefore, these organizations need healthcare consultants who can analyze the organization’s position, diagnose shortcomings, and create solutions to help overall growth.
.png)
8 Free Consulting Templates
Access 8 templates for consultants in The Complete Consultant's Success Kit.
- Management Consulting Plan Template
- Business Plan Template
- Sales Plan Template
Download Free
All fields are required.
You're all set!
Click this link to access this resource at any time.
A healthcare organization is a business with many minor sectors to look after; therefore, you can either choose to become a generalist to solve minor problems or specialize in one area to become a known expert and serve specific clients.
Here are the various types of healthcare consulting you can master to help organizations grow.

Strategy Consulting
For a healthcare organization to survive in a competitive market, it should stay at the top of its patients‘ (customers’) minds. As a strategy consultant, you’ll have diverse business knowledge and a deep understanding of your target audience’s pain points.
You’ll mainly conduct well-rounded assessments to find glitches in its business strategy and create solutions. Your job would be to ensure the healthcare organization grows its revenue and delivers excellent patient care.
Marketing Consulting
With the internet almost irreplaceable in customers’ lives, traditional marketing ways to attract customers no longer work. And as customers have many options, it’s far more important to appear as an expert and the only one who can diagnose their problem.
A marketing consultant will create smart digital marketing strategies to help healthcare organizations show up in front of the right target audience as the best option. You’ll be required to stay up-to-date with the latest marketing trends and develop creative campaigns to acquire new customers for these organizations.
Technology Consulting
Technology is ever-changing in the medical space. New equipment, improved medicine, and better treatment procedures are introduced every day.
For healthcare organizations to remain effective, they must leverage efficient technology paired with the right treatment and medication for their patients. The problem is they’re not very well-versed in testing, installing, and working with the latest technological equipment.
As a technology consultant, you’ll evaluate an organization’s technological needs and introduce and test new solutions. You’ll determine if a piece of new equipment is a good fit and will positively help the organization's growth.
HR and Operations Consulting
Like any business, healthcare organizations must ensure that each member adds value. But since they’re dealing with precious lives, they have to be extra careful. An HR and operations consultant will regularly analyze each staff member’s performance and guide them to help advance in their career.
Your duties will include:
- Creating job descriptions and responsibilities.
- Workplace standards.
- Hiring new staff.
- Promoting a healthy workplace culture.
- Ensuring staff members feel recognized when they deliver outstanding performance.
Legal and Regulatory Consulting
To run a healthcare organization legally, it’s required to abide by laws. But getting a license once isn’t enough because the laws and regulations constantly change. They also affect day-to-day operations, patient information management, treatment contracts, and more.
A legal and regulatory consultant is an expert who ensures that the organization abides by changing laws. Your job would include:
- Updating yourself with the recent legal modifications.
- Monitoring your organization’s condition regularly.
- Implementing the changes.
Working as a healthcare consultant is a highly regarded profession. Because you have a higher level of business expertise than an average employee, you’re a priceless resource to the organization.
In addition to developing creative solutions as a healthcare consultant, here are some benefits:
- As it’s a competitive industry with many players, your unique advice will help your client's healthcare organization stay on top.
- You’ll provide insights and expertise regarding company decisions directly impacting customers, patients, and other external stakeholders.
- You’ll get to work with various healthcare organizations and hospitals.
- You’ll maintain job security — as the industry constantly changes, healthcare organizations, pharmaceutical companies, government agencies, and hospitals will always need your expertise.
- You’ll earn an average salary ranging between $63K and $112K yearly.
- You’ll gain employment freedom — as you decide to work in full- or part-time positions or be self-employed.
Since consulting firms can employ hundreds of consultants, they can offer specialized support within various industry sectors. As a consultant at a firm within one of these specialties or sectors, you’ll develop greater expertise and put yourself in an even more desirable position to work with premium clients.
Here are some of the sectors that healthcare consulting firms specialize in:
- Healthcare systems and processes (strategy, technology, revenue, performance, finance, sustainability, etc.)
- Clinical operations
- Federal and state government agencies
- Hospitals, physicians, and physician groups
- Payer or insurance provider strategies
- Delivery systems
- Medical technology
Whether or not you think a firm is right for you, working in the healthcare consulting field requires the same background. Let’s review the typical steps for anyone looking to get into a healthcare consulting role next.
Your education is the most important part of your experience and background when trying to kickstart your career. You need a relevant bachelor’s degree to begin working as a healthcare consultant.

1. Earn a bachelor’s degree.
To ensure your bachelor’s degree is relevant to your desired position in healthcare consulting, choose a field of study related to the industry, such as public health, business, or even nursing. Since healthcare is a complex industry, a bachelor’s degree in a relevant subject will provide you with the necessary background you need to assist your clients and meet their needs effectively.
And speaking of this field's complexity, a master’s degree is something many of the top firms look for when hiring consultants.
2. Obtain a master’s degree (optional).
Having a master‘s degree isn’t necessarily essential to begin your career. A bachelor‘s degree alone qualifies you to get hired as a healthcare consultant. So, if you want to get experience quickly, you may just need a bachelor’s degree. You can always get a master‘s degree whenever you’re ready to upscale.
That being said, an advanced degree will make you more desirable among employers and clients and allow you to land positions with higher salaries and greater responsibilities. You might need a Master of Business Administration (MBA) or a Master of Public Health (MPH).
3. Determine which type of healthcare consultant you want to become.
Next, think about whether you want to be self-employed, work for a company as an internal consultant, or work for a consulting firm. There’s no right or wrong answer here. It’s all a matter of preference based on your goals, aspirations, and work style.
For example, if you thrive in a structured work environment alongside other employees, you might enjoy being at a major firm like McKinsey . But if you’d rather have complete flexibility to make your hours and choose your clients, working for yourself — or even a small firm — might be the way to go.
4. Develop the right skills.
You’ll need to develop various skills to become an effective healthcare consultant. Here are some of the technical and interpersonal skills that will help you do your job well:
- Communication skills. You’ll interact with many clients, coworkers, and patients throughout your career, so you should be a fluent and compelling speaker.
- Problem-solving. One of your most critical jobs would be identifying and solving problems in the healthcare organization. Therefore, you must be a keen observer to find problems and develop innovative solutions.
- Analytical skills. A part of your job will require you to analyze data to determine patterns or loopholes. You should be able to process a large amount of data or information.
- Financial knowledge. As an advisor, you must guide healthcare organizations to help them grow their revenue. You should quickly identify problems with their finances and suggest better solutions.
- Business expertise. If you decide to work as a strategic healthcare consultant, having business knowledge is the most required. Ideally, you should be able to figure out why the healthcare organization as a business isn’t growing.
- Medical expertise. As you’re working in the healthcare industry, it’s a no-brainer you should know about it. Teach yourself about healthcare laws, policies, legislation, practices, etc.
5. Gain experience in the field and grow your network.
After honing the right skills, it’s time to gain real work experience. In your beginning years, you should take as much work as possible as it will allow you to expand your knowledge and grow your professional network.
It’s also a good idea to build connections with other experts in the industry. So it’s easier for you to move up the ranking ladder (or gain more clients), expand your responsibilities, become well-known and highly regarded among clients, and achieve greater career aspirations.
6. Fine-tune your skills and stay up to speed with industry trends.
As both the healthcare industry and your clients are ever-changing, you, as a consultant, should consistently keep your industry knowledge updated and keep improving your skills.
For instance, you know that technology and laws are fast changing and that you’ll be left behind if you’re unaware of the recent changes. If you can't guide organizations to make adjustments based on these changes, you’d no longer be a valuable asset to the industry.
That’s why you should consistently update your knowledge to remain in demand.
Begin your healthcare consulting career.
Healthcare consulting is an impactful, well-regarded, and lucrative career path. You can educate various client types on improving operations, work within the boundaries of healthcare policies and laws, and streamline company processes and strategies. You’re bound to have an exciting and rewarding road ahead working as a healthcare consultant.

Don't forget to share this post!
Related articles.
![medical consulting business plan How to Write a Consulting Proposal [Templates & Examples]](https://knowledge.hubspot.com/hubfs/ft-consulting.webp)
How to Write a Consulting Proposal [Templates & Examples]

30 Consulting Buzzwords that Work (and Don't Work) in Conversation
![medical consulting business plan Start a Consulting Business in 6 Steps [+Ideas for Your Venture]](https://www.hubspot.com/hubfs/image1-Apr-06-2023-09-15-56-0028-PM.png)
Start a Consulting Business in 6 Steps [+Ideas for Your Venture]

What a Retainer-Based Approach Can Do for a Consulting Business

9 Essential Certificates for Consultants

Building a Career in Consulting — The Ultimate Guide

Innovation Consulting: Everything You Need to Know
![medical consulting business plan 15+ Interview Questions for Consultants [+ Sample Responses]](https://53.fs1.hubspotusercontent-na1.net/hubfs/53/Consultant%20Interview.png)
15+ Interview Questions for Consultants [+ Sample Responses]

Consultative Selling: 7 Ways to Win Deals With Consultative Sales

How to Network in Consulting (+6 Tips)
Powerful and easy-to-use sales software that drives productivity, enables customer connection, and supports growing sales orgs
How to Start an Online Healthcare Consultation Business?

Wondering why you might have to think about starting a healthcare consulting business ?
COVID-19 has taken a staggering toll affecting almost all industries, including healthcare. When we speak about healthcare, the industry is complex. Medical organizations have a lot to keep track of, consisting of hundreds of laws, regulations, a wide range of potential jobs, diagnoses, treatments, and medication. And all of these are absolutely critical to the success of the healthcare organization and the health of the patients. That is why medical consultants or healthcare consultants are valuable.
According to Brand essence market research, the healthcare industry is expected to exceed $20 billion by 2025 . And indeed, now is the right time to switch from conventional medical consultation to an online medical consultation business through a powerful conversational marketplace.
What does a medical consultation business do?
Before getting into how to start a healthcare consulting business , let’s understand more about the medical consultation business. Medical consulting is offering advice and guidance to medical institutions to make critical business decisions that influence their growth.
Medical consultants are experts in the healthcare industry- they have the right educational qualification and background on medical laws and policies to help healthcare organizations and hospitals run their businesses the most effectively. Medical consultants advise pharmaceutical businesses, biotech start-ups, health insurance companies, and governments on the most efficient and effective healthcare delivery methods.
Why Online healthcare consulting?
If you want to learn about how to start a healthcare consulting business , you must know more about healthcare consulting and why it is necessary. Creating a healthcare consulting business allows you to work closely with a wide range of medical institutions and organizations. Healthcare organizations, government agencies, hospitals, and pharmaceutical companies will always need industry expertise and advice. So you get to work with amazing clients from different industries. Every client has different needs, expectations, products, and services, so medical consultants can oversee projects of various types.
Working as an online medical consultant is a reputed career as it requires a certain level of academic qualification and expertise to be successful, which isn’t necessarily essential in other fields. You can offer insights and expertise regarding the business decisions of hospitals and medical institutions that directly impact patients, customers, and other stakeholders by launching an online consultation platform .
Here are some advantages of becoming an online health consultant :
Gain a competitive edge
As the healthcare industry is one of the sectors to go digital last, you will have an opportunity to gain a competitive advantage over your competitors. When other healthcare consulting businesses are working on transforming their business, you can emerge as a pioneer in your niche, which would provide a substantial competitive edge.
Flexibility in working hours
Becoming a medical consultant comes with the advantage of having the flexibility of creating your own schedule. With an online consulting website set up, consultant opportunities can be undertaken at your own pace. One of the main online consulting perks is creating a balance between your need between your consulting business and your personal life.
Reduced travel
As you can shift your medical consultation from offline to online, the travel requirements are eliminated, saving you more time and money. Through video conferencing tools, you can communicate and collaborate with medical professionals without having to travel to meet them.
Easy and quick communication
Considering the modern technology available today, customers expect incredible speed and quick response from healthcare consultants. With the fierce competition available in the industry, customers expect to receive value for the money they spent right away. With a healthcare consulting website for your consulting firm, you can quickly connect with customers.
New channel to find new customers
Shifting your medical consulting services online provides consulting firms with new ways to find customers. With an online consulting platform in place, geographical restrictions don’t even exist. Moreover, by launching a medical consulting business , you will have a new client who prefers getting their consulting services online. And with each year passing by, the number of clients preferring online services is increasing considerably.
Convenience and security
Work in either full-time or part-time positions for hospitals and medical organizations, or be self-employed. The traditional way of storing confidential information is not safe for both your clients and your consulting firm.
To offer a safe environment for your customers, your consulting business must have a secure place to keep all the sensitive information. Typically, it’s the database that is linked to your medical consulting website.
Building a successful online medical consultation business
With your expertise and experience in the field, you can start building a thriving online medical consultation business .
Now, let’s look into the steps to building a successful healthcare consulting business.
1. Crafting a Healthcare consulting business plan
Preparing a healthcare consulting business plan involves creating a document that defines your services and how you intend to run your business.
So here is a sample healthcare consulting business plan :
Executive summary : Give a clear description of your medical consulting business and a market analysis summary.
Company analysis : The company analysis section explains how your healthcare business would run, its current stage, legal structure, and related info.
Industry analysis : Conduct industry analysis and elaborate on current trends and market projections that directly affect your niche.
Customer analysis : In this section, understand who will your healthcare business service. Make sure you narrow down the demographics as well and find out the unique needs and how you can fulfill them.
Competitive analysis : When conducting a competitive analysis, include direct competitors whose businesses fulfill your needs and indirect competitors who target a different market.
Operations plan : The operation plans section elaborates on your methods of meeting the goals you have defined. Add both short-term goals and long-term goals, like expanding to a new market.
Management team : Define the team and backgrounds of key members of your team. Focus on your team’s ability to build and run a successful healthcare business.
Financial plan : The financial plan needs you to detail your individual revenue streams, cash flow statements, future income statements, balance sheets, etc.
2. Business models of online consulting business
The business model is an important aspect that plays a significant role in the success of any online consulting business. While medical consultants are usually hired for a one-time consultancy, medical consulting businesses can adopt several business models. You can build a consulting website which is basically a consulting platform that connects consultants with clients.
Here are some of the business models you can adopt:
- Live one-one consulting
One-one consulting is one of the common business models which allows clients to have one-one sessions with you. You can offer personal consulting sessions to professionals in the medical field where you work with them individually. One-one coaching allows your customers to get individual consultations, and the session is catered to offer personalized solutions to customer problems.
- Group Coaching
This is another popular business model where you deliver consultation sessions to a closed group that attends the sessions together. The medical consultants can offer support to several clients of the group at a time. As with any other type of consultation, it is carried out remotely through audio and video calls. By offering group classes, you can enhance productivity by spending your time with several customers at a single time.
- Subscription model
In a subscription business model, you allow your clients to access your consulting, along with the supporting materials and tools for a monthly or yearly subscription fee. You can create subscription packages on your online medical consultation platform and allow customers to book private or group consulting sessions as long as they subscribe to your plan.
3. Launch an online healthcare consultation website for your services
One of the significant benefits of running an online healthcare consultation business is that you can connect with your clients, virtually eliminating the need to meet them in person. This adds to the convenience, especially during the times of the COVID-19 pandemic, as social distancing has become a new norm.
Setting up a consultation site allows your clients to communicate with you through the platform to avail your services. While building a consultation site is mandatory, you don’t have to spend a fortune right away. You can quickly start using professional tutoring software to set up your online consulting site the most rapidly and affordably perfectly for a single and multi-tutor consulting business. You can connect with your clients through video conferencing, live one-one consultations, webinars, group classes, and videos.
4. Choose your preferred payment methods
If you ask about the main benefit of becoming a medical consultant and setting up your own consultation website, it is having complete control of your online consulting business. Having your own consultation platform offers you the flexibility to introduce the consultation fee according to your business requirements and goals. You can choose to charge upfront once the consultation is over or go for pre-billing consultations. However, you choose to charge your clients, integrate multiple payment gateways to offer the flexibility of selecting the preferred payment option for your clients.
5. Set your unique selling propositions and core values
Online healthcare consultation has a lot to do with your profound expertise, inspiring ideas, and value. Clients approach you for your valid expertise, expert suggestions and advice you can offer them. That is why it is critical to establish your unique selling propositions. Make sure your core values align with that of your potential services so that you can offer the best service to them.
6. Marketing strategies to adopt to promote your consulting business
Devising effective ways to promote your medical consultation business is as important as thinking about how to get into medical consulting . Leverage online marketing to find ideal customers and reach out to them with your online healthcare consulting services. The best market strategy you can follow to grow a client base is to build a powerful presence on social platforms like Twitter, Linked In, Facebook, Instagram, etc. Though a traditional form of marketing, email marketing is also very powerful. It can be easy to start with if you already have an email list of potential clients ready for you.
Online Medical consulting is an impactful and lucrative career choice. You can share your expertise and educate clients on improving their operations, work within the boundaries of healthcare laws and policies, and streamline company strategies. Moving your healthcare consultation business operations online and building your own healthcare consultation platform can facilitate smart and remote interaction.
If you want expert assistance in starting a healthcare consulting business , we are always at your service. Please get in touch with us right away!
Book a Free consultation Now!

Srivathsan GK
Free ebook- learn from udemy’s success story.
- Market & Sell
- Online Courses
- Product update
- Success Stories
- Uncategorized
You may also like

How to Create a Coaching Program? (Free Coaching Program Template)

Essential Checklist for Starting a Coaching Business

How to Become an Online Fitness Coach

How to Start a Healthcare Consulting Business
By: Author Tony Martins Ajaero
Home » Business ideas » Healthcare and Medical
Do you want to start a healthcare consulting firm? If YES, here is a complete guide to starting a healthcare consulting business with NO money and no experience .
It is no longer news that the healthcare sector sells like wild fire all over the world. This is one of the reasons why investors are willing to pump in a whole lot of money in order to be sure that they get good returns on their investments.
If you are a wishful entrepreneur with an experience in human resources and healthcare, one way you can launch your way into the business world is to start your own healthcare consulting firm.
You can be rest assured that your services would always be in demand not only by small healthcare organizations, but also big healthcare corporations and related businesses.
Healthcare consulting firms are organizations that specialize in providing business consulting services (healthcare administration or healthcare management) to the healthcare industry in areas such as finance, accounting, marketing, insurance, efficient operational process and other related areas.
Just like most businesses, the healthcare consulting services industry is open to as many people that are interested in the industry as long as they have what it takes to run a healthcare consulting services firm. Opening a healthcare consulting firm is not too expensive except for the money required to rent and furnish an office space.
Running this type of business requires that you should be trained as a consultant and it is indeed a very lucrative business in the United States, Canada, Australia and the United Kingdom because of the desire for continuous growth in the healthcare industry.
If you have decided to start a healthcare consulting services firm, then you must make sure that you carry out thorough feasibility studies and also market survey.
This will enable you properly locate the business in a community or city with the right demography; a location that can readily accept your services.
So, if you have done the required feasibility studies and market research, then you might want to venture into this business. If you have been pondering on starting your own healthcare consulting services firm but do not know how to go about it, then you should consider going through this article; it will sure give you the needed guide and direction.
18 Steps to Starting a Healthcare Consulting Business
1. understand the industry.
Players in the healthcare consulting services industry provide specialist advice to businesses involved in healthcare fields such as hospitals, physicians, pharmaceutical companies, healthcare related organizations, health management organizations and healthcare insurance providers et al.
These services include advice related to financial management, human resources, information technology and other operations.
More than ever before, the demand for healthcare consulting services has increased as a result of technological advances in the healthcare sector and of course the ever – changing regulatory environment in the united states.
Besides, the 2010 Patient Protection and Affordable Care Act expanded access to healthcare to millions of Americans, driving growth in the overall healthcare sector and stimulating demand for the services of healthcare consulting firms.
Nevertheless, budgets remained tight for many industry customers due to the lingering effects of the recession. Going forward, the revenue generated by the healthcare consulting services industry is projected to continue on its upward flight.
The Healthcare Consulting services Industry is indeed a large industry and pretty much active in countries such as United States of America, United Kingdom, France, Germany, Italy, Holland, Switzerland, Australia and Canada et al.
Statistics has it that in the United States of America alone, there are about 17,521 registered and licensed healthcare consulting firms scattered all across the United States responsible for employing about 26,479 and the industry rakes in a whooping sum of $6 billion annually.
The industry is projected to grow at a 7.1 percent annual growth within 2011 and 2016. It is important to state that Accenture, Advisory Board Company, Deloitte, Huron Consulting Group Inc. and PwC have the largest available market share in the industry.
A recent report shows that healthcare consultants have benefited from many factors over the five years to 2017. The report states that healthcare reforms in the United States has driven hospitals and other care providers to realign their operations to accommodate millions of previously uninsured Americans and comply with new regulatory requirements.
The report also noted that declining Medicare and Medicaid reimbursement rate and the rising cost of care have pushed healthcare providers to look for cost savings and engage industry consultants, thereby boosting industry revenue over the five years to 2017.
Coupled with the recovering economy and the passage and implementation of healthcare reforms, demand for healthcare consultants is expected to boom over the period, with total industry revenue forecast to grow an annualized 7.1 percent.
The fact that healthcare consulting firms can easily be found in cities in the United States of America, does not in any way make the industry to be over saturated. The fact that there are people and organizations out there who would always need professional healthcare consulting services from time to time to sort out business related issue et al makes the business evergreen.
Some of the factors that encourage entrepreneurs to start their own healthcare consulting business despite the fact that the business is risky is that the business is highly thriving and profitable and can be started in any part of the world.
Over and above, starting a healthcare consulting firm requires professionalism and a good grasp of the healthcare industry. Besides, you would need to get the required certifications and license and also meet the standard for such business before you can be allowed to start a healthcare consulting firm in the United States.
One good thing about the healthcare consulting industry is that there is a readily available market for their services because individuals and even organizations naturally would want to improve and effectively manage their business. So, if you are well positioned and you know how to deliver results as a healthcare consultant, you will always smile to the bank.
2. Conduct Market Research and Feasibility Studies
- Demographics and Psychographics
The demographic and psychographic arrangement of persons who need the services of healthcare consulting firms cut across businesses involved in healthcare fields such as hospitals, physicians, pharmaceutical companies, healthcare related organizations, health management organizations and healthcare insurance providers et al who need advice and guidance to sort out business related issues.
If you are defining the demographics for your healthcare consulting business, then you should make it all encompassing.
It should include businesses involved in healthcare fields such as hospitals, physicians, pharmaceutical companies, healthcare related organizations, health management organizations and healthcare insurance providers et al within and outside the city you are operating in who have the capacity to pay for your services.
3. Decide Which Niche to Concentrate On
Most healthcare consulting services firms tend to operate general services that involve every business activities that a standard healthcare consulting firm is expected to offer. That is why it seems like there are no niche areas in the industry.
But on the other hand, some healthcare consulting firms may decide to major in some key or niche area such as;
- Strategic management consulting
- Financial management consulting
- Information technology consulting
- Human resource consulting
- Process and logistics consulting services
- Marketing consulting services
The Level of Competition in the Industry
The competitions that exist in the healthcare consulting line of business goes beyond competitions amongst healthcare consulting firms in your location; you are expected to compete with other consulting firms that have the capacity to consult and proffer business solutions to healthcare organizations. Thus, it will be right to say the competition in the healthcare consulting line of business is tough.
The reality is that no matter the level of competition in an industry, if you have done your due diligence and you brand and promote your services or business properly, you will always make headway in the industry. Just ensure you can proffer business solutions to your clients, you can deliver excellent customer care services, get testimonials from your clients and you know how to attract and reach out to your target market.
Above and beyond, there are several healthcare consulting firms and general consulting firms that have the capacity to consult for healthcare organizations scattered all around the United States. So, if you choose to start your own healthcare consulting business in the United States, you will definitely meet stiffer competitions amongst healthcare consulting firms and general consulting firms that have the capacity to consult for healthcare organizations. Besides, there are larger healthcare consulting firms – brands that determine the trends in the industry and you should be ready to compete with them for customers.
4. Know Your Major Competitors in the Industry
In every industry, there are always brands that perform better or are better regarded by customers and the general public than others. Some of these brands are those that have been in the industry for a long time, while others are best known for how they conduct their businesses and the results they have achieved over the years.
These are some of the leading healthcare consulting services firms in the United States of America and also in the globe;
- Advisory Board Company
- Huron Consulting Group Inc.
- Bain & Company
- Deloitte Consulting
- The Chartis Group
- Simione Healthcare Consultants
- FTI Consulting
- Health Advances, LLC
- Pinnacle Healthcare Consulting
- Cynosure Health Solutions
- CTG Health Solutions
- Healthcare Strategy Group
- QHR (Quorum Health Resources)
- Alvarez & Marsal Healthcare Industry Group
- ECG Management Consultants
- Health Care Network Associates
- Healthcare Management & Consulting Services
- Healthplex Associates
Economic Analysis
When it comes to starting a business such as healthcare consulting services firm, you just have to get your feasibility studies and market research right before venturing into the business. It is good to mention that the healthcare consulting services business is not for rookies; it is for professionals who have gathered the required experience and expertise to proffer solutions to people and organizations.
Starting this kind of business definitely entails that you acquire the required degree and professional certifications and also build good working relationship with stakeholders in the healthcare industry. If you are already a major player in the healthcare consulting services industry before venturing out to start your own healthcare consulting services firm, this might not be an issue.
Depending on the scale at which you want to start from, you might require as much as multiple thousands of dollars to strike this off and at the same time you might need far less than that if you choose to start the business from your house, a virtual office or a shared office space.
You will be expected to hire the services of experts that will help you with a comprehensive economic and cost analysis of the business within the location that you intend launching it. If you get your economic and cost analysis right before launching the business, you may not have to stay the long before you breakeven.
5. Decide Whether to Buy a Franchise or Start from Scratch
When it comes to starting a business of this nature, it will pay you to buy the franchise of a successful healthcare consulting services firm as against starting from the scratch. Even though it is relatively expensive and difficult to buy the franchise of an established healthcare consulting services firm, but it will definitely pay you in the long run.
But if you truly want to build your own brand after you must have proved your worth in the financial services industry, then you might just want to start your own healthcare consulting services firm from the scratch. The truth is that it will pay you in the long run to start your healthcare consulting services firm from the scratch. Starting from the scratch will afford you the opportunity to conduct thorough market survey and feasibility studies before choosing a location to launch the business.
Please note that most of the big and successful healthcare consulting services firms round started from the scratch and they were able to build a solid business brand. It takes dedication, hard work and determination to achieve business success and of course you can build your own healthcare consulting services firm to become a successful brand with corporate and individual clients from all across the length and breadth of the United States of America and other countries of the world.
6. Know the Possible Threats and Challenges You Will Face
If you decide to start your own healthcare consulting services firm today, one of the major challenges you are likely going to face is the presence of well – established healthcare consulting services firms and also other related consulting firms and advisory businesses who are offering same services that you intend offering. The only way to avoid this challenge is to create your own market.
Some other threats that you are likely going to face as a healthcare consulting services firm operating in the United States are unfavorable government policies , the arrival of a competitor within your location of operation and global economic downturn which may affect businesses. There is hardly anything you can do as regards these threats other than to be optimistic that things will continue to work for your good.
7. Choose the Most Suitable Legal Entity (LLC, C Corp, S Corp)
Generally, you have the option of either choosing a general partnership, or limited liability Company which is commonly called an LLC for a healthcare consulting services firm. Ordinarily, general partnership should have been the ideal business structure for a small – scale healthcare consulting services firm especially if you are just starting out with a moderate start – up capital.
But people prefer limited liability Company for obvious reasons. If your intention is to grow the business and have clients both corporate and individual from all across the United States of America and other countries of the world, then choosing general partnership is not an option for you. Limited Liability Company , LLC will cut it for you.
Setting up an LLC protects you from personal liability. If anything goes wrong in the business, it is only the money that you invested into the limited liability company that will be at risk. It is not so for general partnerships. Limited liability companies are simpler and more flexible to operate and you don’t need a board of directors, shareholder’s meetings and other managerial formalities.
These are some of the factors you should consider before choosing a legal entity for your healthcare consulting services firm; limitation of personal liability, ease of transferability, admission of new owners, investors’ expectation and of course taxes.
If you take your time to critically study the various legal entity to use for your healthcare consulting services firm, you will agree that limited liability company; an LLC is most suitable. You can start this type of business as limited liability company (LLC) and in future convert it to a ‘C’ corporation or an ‘S’ corporation especially when you have the plans of going public.
8. Choose a Catchy Business Name
Generally, when it comes to choosing a name for a business, it is expected that you should be creative because whatever name you choose for your business will go a long way to create a perception of what the business represents. Usually it is the norm for people to follow the trend in the industry they intend operating from when naming their business.
If you are considering starting your own healthcare consulting services firm, here are some catchy names that you can choose from;
- McIntosh Jason & Co® Healthcare Consulting, LLC
- J K Randel® Healthcare Consulting Services, LLC
- Sage Group® Healthcare Advisors, LLP
- Clarkson McFarlane® Healthcare Consulting Services, LLP
- Innocent Thompson© Healthcare Consulting Services Company, Inc.
- Harrow Smiths & Associates® Healthcare Advisers, LLP
- Silver House® Healthcare Consulting Services Group
- East Coast® Healthcare Consulting Services, LLC
- Phil Nelson & Co Healthcare Advisors, LLP
- Flint Fingers® Healthcare Consulting Services, Inc.
- Shavonne Pearce Healthcare Consulting Services, Inc.
- Shannon & Shaun® Healthcare Consulting Services, LLP
9. Discuss with an Agent to Know the Best Insurance Policies for You
In the United States of America and in most countries of the world, you can’t operate a business without having some of the basic insurance policy covers that are required by the industry you want to operate from. So, it is imperative to create a budget for insurance policy covers and perhaps consult an insurance broker to guide you in choosing the best and most appropriate insurance policies for your healthcare consulting services firm.
Here are some of the basic insurance policy covers that you should consider purchasing if you want to start your own healthcare consulting services firm in the United States of America;
- General insurance
- Risk Insurance
- Financial reinsurance
- Health insurance
- Liability insurance
- Workers Compensation
- Overhead expense disability insurance
- Business owner’s policy group insurance
- Payment protection insurance
10. Protect your Intellectual Property With Trademark, Copyrights, Patents
If you are considering starting your own healthcare consulting services firm, usually you are required to file for intellectual property protection/trademark. This is so because the nature of the business makes it possible for you to challenge organizations and individuals in court for illegally making use of your company’s intellectual properties.
So also, if you want to protect your company’s logo and other documents or software that are unique to you or even jingles and media production concepts, then you can go ahead to file for intellectual property protection. If you want to register your trademark, you are expected to begin the process by filing an application with the USPTO. The final approval of your trademark is subjected to the review of attorneys as required by the USPTO.
11. Get the Necessary Professional Certification
Aside from the results you produce as it relates to timely and result oriented finance, accounting, marketing, insurance, and efficient operational process advice to your clients, professional certification is one of the main reasons why some healthcare consulting services firm stand out.
If you want to make an impact in the healthcare consulting services industry, you should work towards acquiring all the needed certifications in your area of specialization. Certification validates your competency and shows that you are highly skilled, committed to your career and up-to-date in this competitive market.
These are some of the certifications you can work towards achieving if you want to run your own healthcare consulting services firm;
- Certified Healthcare Business Consultant (CHBC)
- ACHC Certified Consultants
- Chartered Financial Analyst (CFA®)
- Chartered Financial Consultant (ChFC)
- Chartered Market Technician (CMT)
- Degree in Management and Healthcare Related Courses
Please note that you cannot successfully run a healthcare consulting services firm in the United States and in most countries of the world without necessarily acquiring professional certifications and business license even if you have adequate experience cum background in the healthcare consulting services industry.
12. Get the Necessary Legal Documents You Need to Operate
The essence of having the necessary documentation in place before launching a business in the United States of America cannot be overemphasized especially a business such as healthcare consulting services firm. It is a fact that you cannot successfully run any business in the United States without the proper documentations. If you do, it won’t be too long before the law catches up with you.
These are some of the basic legal documents that you are expected to have in place if you want to legally run your own healthcare consulting services firm in the United States of America;
- Certificate of Incorporation
- Federal Tax Payer’s ID
- State Permit
- Business License and Certification
- Business Plan
- Non – disclosure Agreement
- Employment Agreement (offer letters)
- Operating Agreement for LLCs
- Insurance Policy
- Consulting contract documents
- Online Terms of Use
- Online Privacy Policy Document
- Apostille (for those who intend operating beyond the United States of America)
- Company Bylaws
- Memorandum of Understanding (MoU)
13. Raise the Needed Startup Capital
Aside from the required certifications and hands-on experience, starting a healthcare consulting services firm can be cost effective. Securing a standard office in a good business district, equipping the office and paying your employees are part of what will consume a large chunk of your start – up capital.
When it comes to financing a business, one of the first things that you should consider is to write a good business plan . If you have a good and workable business plan document in place, you may not have to labor yourself before convincing your bank, investors and your friends to invest in your business or to partner with you.
Here are some of the options you can explore when sourcing for start – up capital for your healthcare consulting services firm;
- Raising money from personal savings and sale of personal stocks and properties
- Raising money from investors and business partners
- Sell of shares to interested investors
- Applying for loan from your bank/banks
- Pitching your business idea and applying for business grants and seed funding from donor organizations and angel investors
- Source for soft loans from your family members and your friends
14. Choose a Suitable Location for your Business
Healthcare consulting services firm and most consulting services based type of businesses require that you see physically with your clients hence it must be located in a good location; a location that is prone to both human and vehicular traffic and a location that is at the epicenter of a healthcare – related business district if indeed you want to attend to loads of clients and
- The demography of the location
- The demand for the services of healthcare consulting services in the location
- The purchasing power of businesses involved in healthcare fields such as hospitals, physicians, pharmaceutical companies, healthcare related organizations, health management organizations and healthcare insurance providers et al in the location
- Accessibility of the location
- The number of healthcare consulting services firms and related consulting services businesses that are in the location
- The local laws and regulations in the community/state
- Traffic, parking and security et al
15. Hire Employees for your Technical and Manpower Needs
On the average, there are no special technology or equipment needed to run this type of business except for customized healthcare consulting software and other related software apps and social media management software applications. So also, you will definitely need computers, internet facility, telephone, fax machine and office furniture (chairs, tables, and shelves).
When it comes to choosing between renting and leasing an office space, the size of the healthcare consulting services firm you want to build, and your entire budget for the business should influence your choice. If you have enough capital to run a standard healthcare consulting services firm then you should consider the option of leasing a facility for your office; when you lease, you will be able to work with long – term planning, structuring and expansion.
As regards the number of employees that you are expected to kick start the business with, you would need to consider your finance before making the decision. Averagely, you would need a Chief Executive Officer/Lead Healthcare Advisor, Healthcare Consultants, Risk Analyst, Legal Secretary, Admin and HR Manager, Business Developer, Accountant, Customer Service Executive/Front Desk Officer.
Over and above, you would need a minimum of 5 to 10 key staff to effectively run a medium scale but standard healthcare consulting services firm. Please note that there will be times when you are expected to go out of your way to hire experts to help you handle some high – profile clients especially from big corporations. If you are just starting out, you may not have the financial capacity or required business structure to retain all the professionals that are expected to work with you.
The Service Delivery Process of the Business
The way healthcare consulting services firms work vary from one agency to another, but ideally, a healthcare consulting services firm is expected to first and foremost build a robust company profile before sourcing for clients. Basically, when clients hire your services, they expect you to proffer solution to their pressing business-related challenges and concerns.
Depending on the agreement reached by both parties, you are expected to come up with measurable indices that will show that the professional advice you gave or products sold is indeed producing results. In some cases, the agreed consulting fee will be paid in part and in some cases, it will be paid in full and upfront.
It is important to state that a healthcare consulting services firm may decide to improvise or adopt any business process and structure that will guarantee them, good return on investment (ROI), efficiency and flexibility; the above stated healthcare consulting business cum services process is not cast on stone.
16. Write a Marketing Plan Packed with ideas & Strategies
As a healthcare consulting services firm, you would have to prove your worth over and over again before attracting corporate organizations and individuals to hire your services. So, if you have plans to start your own healthcare consulting services firm, it will pay you to build first build a successful career in the alternative healthcare services industry.
So, when you are drafting marketing plans and strategies for your healthcare consulting services firm, make sure that you create a compelling personal and company profile. Aside from your qualifications and experience, it is important to clearly state in practical terms what you have been able to achieve in time past as it relates to the healthcare consulting services industry and the organizations you have worked for. This will help boost your chances in the market place when sourcing for clients.
Here are some of the platforms you can utilize to market your healthcare consulting services firm;
- Introduce your business by sending introductory letters alongside your brochure to all the businesses involved in the healthcare field such as hospitals, physicians, pharmaceutical companies, healthcare related organizations, health management organizations and healthcare insurance providers et al within and outside the city you are operating in who have the capacity to pay for your services
- Advertise your business in relevant healthcare magazines, radio and TV stations (make yourself available for healthcare consulting services related talk shows and interactive sessions on TV and Radio)
- List your business on local directories / yellow pages
- Attend international healthcare expos, seminars, and business fairs
- Create different packages for different category of clients in order to consult for them
- Leverage on the internet to promote your business
- Join local chambers of commerce and industries around you with the main aim of networking and marketing your services; you are likely going to get referrals from such networks
- Engage the services of marketing executives and business developers to carry out direct marketing for you
17. Work Out a Reasonable Pricing for your Services & Products
One key factor that will help you offer your services at a price that is highly attractive is to ensure that you source your working capital from sources that won’t put pressure on you.
Another strategy that will help you offer your services at the right price is to ensure that you cut operational cost to the barest minimum, and channel your efforts towards marketing and promoting your brand name. Aside from the fact that this strategy will help you save cost, it will also help you get the right pricing for your products and services.
You can also try as much as possible to work with independent contractors and marketers; it will help you save cost for paying sales and marketing executives.
18. Develop Strategies to Boost Brand Awareness and Create a Corporate Identity
If you are in business and you are not deliberate about boosting you brand awareness and communicating your corporate identity, then you should be ready to take on whatever the society portray your business to be. One of the secrets of larger corporations is that they are willing to spend fortunes year in and year out to boost their brand awareness and to continue to communicate their corporate identity the way they want people to perceive them to be.
If your intention of starting a healthcare consulting services firm is to grow the business beyond the city where you are going to be operating from to become a national and international brand, then you must be ready to spend money on the promotion and advertisement of your brand.
In promoting your brand and corporate identity, you should leverage on both the print and electronic media and also social media (the internet). As a matter of fact, it is cost effective to use the internet and social media platforms to promote your brand, besides it is pretty much effective and wide reaching.
Another strategy is to sponsor relevant community based programs, TV and radio programs, advertise your business in relevant magazines and newspapers. Below are the platforms you can leverage on to boost your brand and to promote and advertise your healthcare consulting services firm;
- Place adverts on healthcare related magazines and newspapers, radio and TV stations
- Encourage the use of word of mouth publicity from your loyal customers
- Leverage on the internet and social media platforms like YouTube, Instagram, Facebook, Twitter, LinkedIn, Snapchat, Badoo, Google+ and other platforms to promote your business
- Ensure that you position your banners and billboards in strategic positions all around your city
- Distribute your fliers and handbills in target areas in and around your neighborhood
- Contact businesses involved in healthcare fields such as hospitals, physicians, pharmaceutical companies, healthcare related organizations, health management organizations and healthcare insurance providers et al within and outside the city you are operating in who have the capacity to pay for your services by calling them up and informing them of your organization and the services you offer
- Advertise your business in your official website and employ strategies that will help you pull traffic to the site
- Brand all your official cars and ensure that all your staff members wear your branded shirt or cap at regular intervals.
Related Posts:
- How Much Money Do Aromatherapists Make Yearly? [Profit Margin]
- How to Get DNV GL Advanced Certified Healthcare Operations Certification
- How to Start a Clinical Research Organization
- 50 Best Healthcare and Medical Business ideas
- How Much Does It Cost to Start a DME Company?
Healthcare Business Plan Template
Written by Dave Lavinsky
Healthcare Business Plan
You’ve come to the right place to create your Healthcare business plan.
We have helped over 10,000 entrepreneurs and business owners create business plans and many have used them to start or grow their Healthcare companies.
Below is a template to help you create each section of your Healthcare business plan.
Executive Summary
Business overview.
Riverside Medical is a family medical clinic located in San Francisco, California. Our goal is to provide easy access to quality healthcare, especially for members of the community who have low to moderate incomes. Our clinic provides a wide range of general and preventative healthcare services, including check-ups, minor surgeries, and gynecology. Anyone of any age or group is welcome to visit our clinic to get the healthcare that they need.
Our medical practitioners and supporting staff are well-trained and have a passion for helping improve the health and well-being of our clients. We serve our patients not just with our knowledge and skills but also with our hearts. Our clinic was founded by Samantha Parker, who has been a licensed doctor for nearly 20 years. Her experience and compassion will guide us throughout our mission.
Product Offering
Riverside Medical will provide extensive general care for all ages, creating a complete healthcare solution. Some of the services included in our care include the following:
- Primary care: annual checkups, preventative screenings, health counseling, diagnosis and treatment of common conditions
- Gynecology: PAP tests, annual well-woman exam, and family planning
- Pediatrics: infant care, annual physicals, and immunizations
- Minor procedures: stitches, casts/splints, skin biopsies, cyst removals, and growth lacerations
- Health and wellness: weight loss strategies, nutrition guidance, hormone balance, and preventive and routine services
The costs will depend upon the materials used, the physician’s time, and the amount designated for each procedure. Medical bills will be billed either directly to the patient or to their insurance provider.
Customer Focus
Riverside Medical will primarily serve the community living and working within the San Francisco bay area. The city is diverse and growing and includes people of all ages, ethnicities, and backgrounds. Everyone is welcome to visit our clinic to receive the health care they need.
Management Team
Riverside Medical’s most valuable asset is the expertise and experience of its founder, Samantha Parker. Samantha has been a licensed family doctor for 20 years now. She spent the most recent portion of her career on medical mission trips, where she learned that many people are not privileged to have access to quality medical services. Samantha will be responsible for ensuring the general health of her patients and creating a viable and profitable business medical practice.
Riverside Medical will also employ nurses, expert medical staff, and administrative assistants that also have a passion for healthcare.
Success Factors
Riverside Medical will be able to achieve success by offering the following competitive advantages:
- Location: Riverside Medical’s location is near the center of town. It’s visible from the street with many people walking to and from work on a daily basis, giving them a direct look at our clinic, most of which are part of our target market.
- Patient-oriented service: Riverside Medical will have a staff that prioritizes the needs of the patients and educates them on the proper way how to take care of themselves.
- Management: Samantha Parker has a genuine passion for helping the community, and because of her previous experience, she is fully equipped and overqualified to open this practice. Her unique qualifications will serve customers in a much more sophisticated manner than our competitors.
- Relationships: Having lived in the community for 25 years, Samantha Parker knows many of the local leaders, newspapers, and other influences. Furthermore, she will be able to draw from her ties to previous patients from her work at other clinics to establish a starting clientele.
Financial Highlights
Riverside Medical is seeking a total funding of $800,000 of debt capital to open its clinic. The capital will be used for funding capital expenditures and location build-out, acquiring basic medical supplies and equipment, hiring initial employees, marketing expenses, and working capital.
Specifically, these funds will be used as follows:
- Clinic design/build: $100,000
- Medical supplies and equipment: $150,000
- Six months of overhead expenses (rent, salaries, utilities): $450,000
- Marketing: $50,000
- Working capital: $50,000
The following graph below outlines the pro forma financial projections for Riverside Medical.
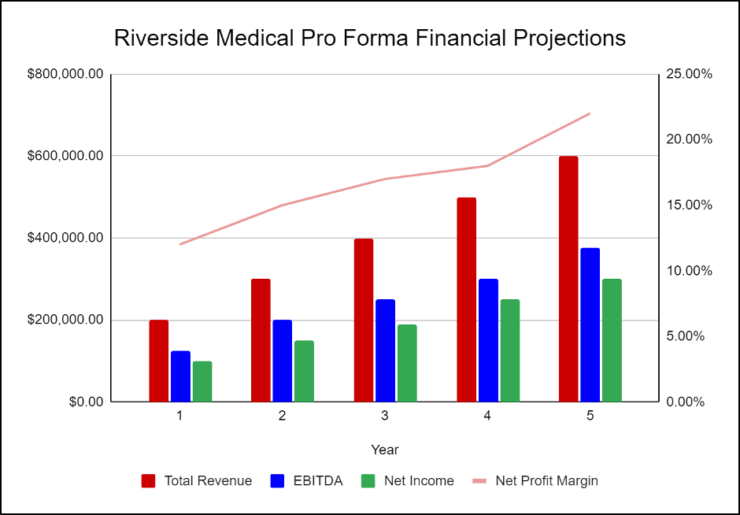
Company Overview
Who is riverside medical, riverside medical history.
Samantha Parker started the clinic with the goal of providing easy access to good quality health service, especially to those members of the community with low to moderate income. After years of planning, she finally started to build Riverside Medical in 2022. She gathered a group of professionals to fund the project and was able to incorporate and register Riverside Medical with their funding support.
Since its incorporation, Riverside Medical has achieved the following milestones:
- Found clinic space and signed Letter of Intent to lease it
- Developed the company’s name, logo, and website
- Hired a contractor for the office build-out
- Determined equipment and fixture requirements
- Began recruiting key employees with previous healthcare experience
- Drafted marketing campaigns to promote the clinic
Riverside Medical Services
Industry analysis.
The global healthcare market is one of the largest and highest-valued industries in the world. According to Global Newswire, the global healthcare services market is currently valued at $7548.52 billion and is expected to reach $10414.36 billion in 2026. This growth is expected to continue for the foreseeable future.
The biggest drivers of industry growth throughout the next decade will be a continual increase in illnesses and diseases as well as a quickly aging population. With more people aging and needing daily/frequent care, hospitals and medical clinics are bound to be in even more demand than they already are.
One obstacle for the industry is the rising cost of care. Though this results in greater profits, more and more Americans cannot afford basic medical care. Therefore, they are opting out of procedures they believe are unnecessary or unimportant.
Despite the challenges of the next decade, the industry is still expected to see substantial growth and expansion.
Customer Analysis
Demographic profile of target market.
Riverside Medical will serve the residents of the San Francisco bay area as well as those who work in the area.
The population of the area experiences a large income gap between the highest earners and the lowest earners. Therefore, it is hard for middle and lower-class families to find quality care that is affordable. As a result, they are in need of the services that we offer and are looking for accessible medical care.
The precise demographics of San Francisco are as follows:
Customer Segmentation
Our clinic is a general family practice and will treat patients of all ages, incomes, physical abilities, races, and ethnicities. As such, there is no need to create marketing materials targeted at only one or two of these groups, but we can appeal to all with a similar message.
Competitive Analysis
Direct and indirect competitors.
Riverside Medical will face competition from other companies with similar business profiles. A description of each competitor company is below.
City Medical
Founded in 2008, City Medical is a membership-based, primary-care practice in the heart of the city. City Medical offers a wide range of primary care services for patients who subscribe to the practice for an annual fee. Patients enjoy personalized care, including office visits, as well as the diagnosis and treatment of common health problems. The patient membership fee covers the services listed below, and most care is received in-office. However, some additional services, such as lab testing and vaccinations, are billed separately. Furthermore, though the annual fee is convenient for some, it is too high for many families, so many are priced out of care at this facility.
Bay Doctors
Bay Doctors is a primary care practice that provides highly personalized medical care in the office or patients’ homes. Bay Doctors includes a team of dedicated healthcare professionals with dual residency in Emergency Medicine and Internal Medicine. The practice offers same-day/next-day appointments, telemedicine, office visits, and home visits. Some of the medical care services they provide are primary care, urgent care, emergency care, gynecology, pediatrics, and minor procedures.
Community Care
Established in 1949, Community Care is a non-profit regional healthcare provider serving the city and surrounding suburbs. This facility offers a wide variety of medical services, including 24-hour emergency care, telemedicine, primary care, and more. In addition to their medical care, they have a wide variety of fundraising activities to raise money to operate the hospital and help families cover the costs of their care.
Competitive Advantage
Riverside Medical enjoys several advantages over its competitors. These advantages include:
Marketing Plan
Brand & value proposition.
The Riverside Medical brand will focus on the company’s unique value proposition:
- Client-focused healthcare services, where the company’s interests are aligned with the customer
- Service built on long-term relationships
- Big-hospital expertise in a small-clinic environment
Promotions Strategy
The promotions strategy for Riverside Medical is as follows:
Riverside Medical understands that the best promotion comes from satisfied customers. The company will encourage its patients to refer their friends and family by providing healthcare benefits for every new client produced. This strategy will increase in effectiveness after the business has already been established.
Direct Mail
The company will use a direct mail campaign to promote its brand and draw clients, as well. The campaign will blanket specific neighborhoods with simple, effective mail advertisements that highlight the credentials and credibility of Riverside Medical.
Website/SEO
Riverside Medical will invest heavily in developing a professional website that displays all of the clinic’s services and procedures. The website will also provide information about each doctor and medical staff member. The clinic will also invest heavily in SEO so the brand’s website will appear at the top of search engine results.
Social Media
Riverside Medical will invest heavily in a social media advertising campaign. The marketing manager will create the company’s social media accounts and invest in ads on all social media platforms. It will use targeted marketing to appeal to the target demographics.
Riverside Medical’s pricing will be lower than big hospitals. Over time, client testimonials will help to maintain our client base and attract new patients. Furthermore, we will be able to provide discounts and incentives for lower-income families by connecting with foundations and charities from people who are interested in helping.
Operations Plan
The following will be the operations plan for Riverside Medical.
Operation Functions:
- Samantha Parker is the founder of Riverside Medical and will operate as the sole doctor until she increases her patient list and hires more medical staff. As the clinic grows, she will operate as the CEO and take charge of all the operations and executive aspects of the business.
- Samantha is assisted by Elizabeth O’Reilly. Elizabeth has experience working as a receptionist at a fast-paced hospital and will act as the receptionist/administrative assistant for the clinic. She will be in charge of the administrative and marketing aspects of the business.
- Samantha is in the process of hiring doctors, nurses, and other medical staff to help with her growing patient list.
Milestones:
The following are a series of path steps that will lead to the vision of long-term success. Riverside Medical expects to achieve the following milestones in the following twelve months:
3/202X Finalize lease agreement
5/202X Design and build out Riverside Medical location
7/202X Hire and train initial staff
9/202X Kickoff of promotional campaign
11/202X Reach break-even
1/202X Reach 1000 patients
Financial Plan
Key revenue & costs.
Riverside Medical’s revenues will come primarily from medical services rendered. The clinic will either bill the patients directly or their insurance providers.
The major cost drivers for the clinic will include labor expenses, lease costs, equipment purchasing and upkeep, and ongoing marketing costs.
Funding Requirements and Use of Funds
Key assumptions.
Below are the key assumptions required to achieve the revenue and cost numbers in the financials and to pay off the startup business loan.
- Year 1: 120
- Year 2: 150
- Year 3: 200
- Year 4: 275
- Year 5: 400
- Annual lease: $50,000
Financial Projections
Income statement.
| FY 1 | FY 2 | FY 3 | FY 4 | FY 5 | ||
|---|---|---|---|---|---|---|
| Revenues | ||||||
| Total Revenues | $360,000 | $793,728 | $875,006 | $964,606 | $1,063,382 | |
| Expenses & Costs | ||||||
| Cost of goods sold | $64,800 | $142,871 | $157,501 | $173,629 | $191,409 | |
| Lease | $50,000 | $51,250 | $52,531 | $53,845 | $55,191 | |
| Marketing | $10,000 | $8,000 | $8,000 | $8,000 | $8,000 | |
| Salaries | $157,015 | $214,030 | $235,968 | $247,766 | $260,155 | |
| Initial expenditure | $10,000 | $0 | $0 | $0 | $0 | |
| Total Expenses & Costs | $291,815 | $416,151 | $454,000 | $483,240 | $514,754 | |
| EBITDA | $68,185 | $377,577 | $421,005 | $481,366 | $548,628 | |
| Depreciation | $27,160 | $27,160 | $27,160 | $27,160 | $27,160 | |
| EBIT | $41,025 | $350,417 | $393,845 | $454,206 | $521,468 | |
| Interest | $23,462 | $20,529 | $17,596 | $14,664 | $11,731 | |
| PRETAX INCOME | $17,563 | $329,888 | $376,249 | $439,543 | $509,737 | |
| Net Operating Loss | $0 | $0 | $0 | $0 | $0 | |
| Use of Net Operating Loss | $0 | $0 | $0 | $0 | $0 | |
| Taxable Income | $17,563 | $329,888 | $376,249 | $439,543 | $509,737 | |
| Income Tax Expense | $6,147 | $115,461 | $131,687 | $153,840 | $178,408 | |
| NET INCOME | $11,416 | $214,427 | $244,562 | $285,703 | $331,329 |
Balance Sheet
| FY 1 | FY 2 | FY 3 | FY 4 | FY 5 | ||
|---|---|---|---|---|---|---|
| ASSETS | ||||||
| Cash | $154,257 | $348,760 | $573,195 | $838,550 | $1,149,286 | |
| Accounts receivable | $0 | $0 | $0 | $0 | $0 | |
| Inventory | $30,000 | $33,072 | $36,459 | $40,192 | $44,308 | |
| Total Current Assets | $184,257 | $381,832 | $609,654 | $878,742 | $1,193,594 | |
| Fixed assets | $180,950 | $180,950 | $180,950 | $180,950 | $180,950 | |
| Depreciation | $27,160 | $54,320 | $81,480 | $108,640 | $135,800 | |
| Net fixed assets | $153,790 | $126,630 | $99,470 | $72,310 | $45,150 | |
| TOTAL ASSETS | $338,047 | $508,462 | $709,124 | $951,052 | $1,238,744 | |
| LIABILITIES & EQUITY | ||||||
| Debt | $315,831 | $270,713 | $225,594 | $180,475 | $135,356 | |
| Accounts payable | $10,800 | $11,906 | $13,125 | $14,469 | $15,951 | |
| Total Liability | $326,631 | $282,618 | $238,719 | $194,944 | $151,307 | |
| Share Capital | $0 | $0 | $0 | $0 | $0 | |
| Retained earnings | $11,416 | $225,843 | $470,405 | $756,108 | $1,087,437 | |
| Total Equity | $11,416 | $225,843 | $470,405 | $756,108 | $1,087,437 | |
| TOTAL LIABILITIES & EQUITY | $338,047 | $508,462 | $709,124 | $951,052 | $1,238,744 |
Cash Flow Statement
| FY 1 | FY 2 | FY 3 | FY 4 | FY 5 | ||
|---|---|---|---|---|---|---|
| CASH FLOW FROM OPERATIONS | ||||||
| Net Income (Loss) | $11,416 | $214,427 | $244,562 | $285,703 | $331,329 | |
| Change in working capital | ($19,200) | ($1,966) | ($2,167) | ($2,389) | ($2,634) | |
| Depreciation | $27,160 | $27,160 | $27,160 | $27,160 | $27,160 | |
| Net Cash Flow from Operations | $19,376 | $239,621 | $269,554 | $310,473 | $355,855 | |
| CASH FLOW FROM INVESTMENTS | ||||||
| Investment | ($180,950) | $0 | $0 | $0 | $0 | |
| Net Cash Flow from Investments | ($180,950) | $0 | $0 | $0 | $0 | |
| CASH FLOW FROM FINANCING | ||||||
| Cash from equity | $0 | $0 | $0 | $0 | $0 | |
| Cash from debt | $315,831 | ($45,119) | ($45,119) | ($45,119) | ($45,119) | |
| Net Cash Flow from Financing | $315,831 | ($45,119) | ($45,119) | ($45,119) | ($45,119) | |
| Net Cash Flow | $154,257 | $194,502 | $224,436 | $265,355 | $310,736 | |
| Cash at Beginning of Period | $0 | $154,257 | $348,760 | $573,195 | $838,550 | |
| Cash at End of Period | $154,257 | $348,760 | $573,195 | $838,550 | $1,149,286 |
Healthcare Business Plan FAQs
What is a healthcare business plan.
A healthcare business plan is a plan to start and/or grow your healthcare business. Among other things, it outlines your business concept, identifies your target customers, presents your marketing plan and details your financial projections.
You can easily complete your Healthcare business plan using our Healthcare Business Plan Template here .
What are the Main Types of Healthcare Businesses?
There are a number of different kinds of healthcare businesses , some examples include: Nursing care, Physical home health care, or Home health care aides:
How Do You Get Funding for Your Healthcare Business Plan?
Healthcare businesses are often funded through small business loans. Personal savings, credit card financing and angel investors are also popular forms of funding.
What are the Steps To Start a Healthcare Business?
Starting a healthcare business can be an exciting endeavor. Having a clear roadmap of the steps to start a business will help you stay focused on your goals and get started faster.
1. Develop A Healthcare Business Plan - The first step in starting a business is to create a detailed healthcare business plan that outlines all aspects of the venture. This should include potential market size and target customers, the services or products you will offer, pricing strategies and a detailed financial forecast.
2. Choose Your Legal Structure - It's important to select an appropriate legal entity for your healthcare business. This could be a limited liability company (LLC), corporation, partnership, or sole proprietorship. Each type has its own benefits and drawbacks so it’s important to do research and choose wisely so that your healthcare business is in compliance with local laws.
3. Register Your Healthcare Business - Once you have chosen a legal structure, the next step is to register your healthcare business with the government or state where you’re operating from. This includes obtaining licenses and permits as required by federal, state, and local laws.
4. Identify Financing Options - It’s likely that you’ll need some capital to start your healthcare business, so take some time to identify what financing options are available such as bank loans, investor funding, grants, or crowdfunding platforms.
5. Choose a Location - Whether you plan on operating out of a physical location or not, you should always have an idea of where you’ll be based should it become necessary in the future as well as what kind of space would be suitable for your operations.
6. Hire Employees - There are several ways to find qualified employees including job boards like LinkedIn or Indeed as well as hiring agencies if needed – depending on what type of employees you need it might also be more effective to reach out directly through networking events.
7. Acquire Necessary Healthcare Equipment & Supplies - In order to start your healthcare business, you'll need to purchase all of the necessary equipment and supplies to run a successful operation.
8. Market & Promote Your Business - Once you have all the necessary pieces in place, it’s time to start promoting and marketing your healthcare business. This includes creating a website, utilizing social media platforms like Facebook or Twitter, and having an effective Search Engine Optimization (SEO) strategy. You should also consider traditional marketing techniques such as radio or print advertising.
Other Helpful Business Plan Templates
Nonprofit Business Plan Template Non-Emergency Medical Transportation Business Plan Template Medical Practice Business Plan Template Home Health Care Business Plan Template

Humanizing healthcare
People expect intuitive access to their healthcare and personalized experiences. Leaders that reinvent to create easy access and engaging experiences will stay resilient while delivering better outcomes.
Healthcare now
of CEOs and 79% of health system leaders see substantial or transformative change ahead
increase in home and virtual care expected by health executives over the next decade
the projected shortage of nurses by 2030 according to the International Council of Nurses
of healthcare workers’ tasks in the US could be redesigned by technology augmentation or automation
How to reinvent health
Use technology to humanize healthcare for people and the organization, get new value from your emr cloud, reinvent care to grow the capacity of your clinicians so they can help more patients..

All for one and one for all
Improve the health experiences that improve health outcomes and achieve loyalty over leaving., optimize health facility operations, combat rising costs and complexity, and build organizational resilience, improve patient care by strengthening your digital core.
Want to expand access to healthcare, bolster its security and improve patient care? Technology can help get you there: continuous innovation, data insight and a strong digital core.
Customize service
Personalize patient engagement using advanced digital capabilities — like cloud, data and AI.
Maximize care with Gen-AI
Augment scarce clinical resources through the combined power of technology and human ingenuity.
Secure health for all
Integrate your incident response and risk resilience to build patient confidence and trust — and drive growth.
The cloud enables a more secure, dynamic and efficient EMR system. It not only minimizes your risk and disruption, it increases the insights and value you get from it.
Cost reduction
You can reduce costs by improving your technology infrastructure, consumption-based fees and managed services.
Strengthen your security’s ability to mitigate cybersecurity attacks and minimize downtime impact.
Reliability
Improve the stability and availability of your EMR technology by integrating your data with the cloud.
The workforce deficit requires a fundamental reassessment of work. Technology can improve access, experience and outcomes for all—but it cannot solve the issues without human ingenuity.
$4.6 billion
Enable the workforce.
Use analytics to identify ways to improve care processes and capacity — and ease clinical burdens.
Revamp for better care
Redesign care delivery models so you can offer your patients care anywhere and behavioral health integration.
Improve patient journeys
Transform rote patient journeys into customized intelligent journeys to improve patient experiences and results.
Data-driven, AI-powered tools are already helping healthcare professionals consider their patients’ cultures and backgrounds in their delivery of equitable patient outcomes.
Create sustainable change
Sustainable change is structural change we can guide you through during the care continuum: reinventing care delivery, scaling social investments, integrating clinical research and more.
Mitigate bias in data
Don’t let your data perpetuate healthcare inequity. Use data-driven, AI-powered tools that enable culture-centered, unbiased decisions.
Inclusive design
Health equity must be considered from the start of product and service design. Engage community-based organizations and leaders early and throughout. Produce culture-specific materials and communications.
Stop trading off experience vs. access vs. outcomes. With a reinvention mindset, you can enable a new frontier of possibilities and provide each patient with relevant experiences crafted to their needs.
Human-centric care
Intelligent technology can help you meet people where they are — and free up clinician time to focus on people’s high-touch needs.
Connected patient journey
Build loyalty and trust by offering an omnichannel experience that seamlessly powers the whole patient journey.
Prepare your organization for today’s disruptions — and tomorrow’s
Transform your operations to help your organization respond to every disruption — from advanced technologies to rising customer expectations.
Intelligent health facilities
Optimize health facility operations patient experience with smart technologies. It will create a more sustainable business and environment for staff, patients and broader community.
Efficient corporate functions
Combat healthcare’s complexity and cost pressures by introducing shared services, centralized functions, standardized processes and strategic sourcing.
Segments we support
Stabilize the workforce to deliver better experiences and outcomes by bringing together technology and humans to rethink care delivery.
Mega mergers, digital disruption, new competitors...it’s all disrupting payers. Use advanced technologies to speed change, retain and attract talent, redefine work and innovate.
Use data-driven insights to deliver outcomes for national, state and local communities affordably, efficiently and with equity.
What’s trending in health

Five imperatives the C-suite must address to reinvent in the age of generative AI.

We outline factors to help healthcare providers and payers deliver the digital health experiences that people expect to promote patient loyalty.

Through growth and talent strategies, Accenture helped PruittHealth navigate the pandemic’s challenges, enhancing senior care access and improving its financial outcomes.

Addressing the clinician shortage for the long term requires continuous, dynamic reinvention to reimagine work and the workforce. Four imperatives that health leaders need to prioritize.

The nursing shortage is a global health emergency. By reinventing care delivery using nurse talent and technology, we can solve this critical challenge.
With innovations like ChatGPT dominating headlines, the world is waking up to the transformative potential of generative AI. Find out how AI working side-by-side with people will impact science, business and society itself.

Cyber transformers are excelling at both business resilience and business outcomes—with high-performing cybersecurity propelling their digital transformations forward.

The four trends in the Accenture Digital Health Technology Vision show how technology innovations are shaping healthcare experiences of the future.
Partners in change

Unlock end-to-end value through insights and accelerated digital transformation with Oracle cloud and enterprise solutions.

The largest global Microsoft practice. Eighteen-time Microsoft Global Alliance SI Partner of the Year. Powered by Avanade. Runs on Microsoft.

Reimagining human experiences that reignite growth and accelerate the path to value.
Awards and recognition
Overall leader in everest group healthcare data & analytics.
Accenture recognized for strategic acquisitions, and focus on analytics, cloud and AI technologies to drive digital transformation for Payer organizations.
Top leader Healthcare Provider digital services Everest
Accenture scored higher than all competitors in both Market Impact and Vision & Capability for its ability to drive digital transformation across the healthcare provider value chain, including patient engagement, care management, financials and network management.
Leader in Healthcare Payer digital services Everest
Our leaders.

Rich Birhanzel
Senior Managing Director – Global Health Lead

Steve Savas
Managing Director – Strategy & Consulting, Health Lead, North America

Kaveh Safavi, MD, JD
Senior Managing Director – Consulting Global Health

Michael Zettel
Senior Managing Director - EMEA Health Industry Lead

Kristin Ficery
Senior Managing Director – Global Health Strategy Lead
Grow your careers at the heart of change

Medical Device Business Plan Template
Written by Dave Lavinsky

Medical Device Business Plan
Over the past 20+ years, we have helped over 500 entrepreneurs and business owners create business plans to start and grow their medical device companies.
If you’re unfamiliar with creating a medical device business plan, you may think creating one will be a time-consuming and frustrating process. For most entrepreneurs it is, but for you, it won’t be since we’re here to help. We have the experience, resources, and knowledge to help you create a great business plan.
In this article, you will learn some background information on why business planning is important. Then, you will learn how to write a medical device business plan step-by-step so you can create your plan today.
Download our Ultimate Business Plan Template here >
What is a Medical Device Business Plan?
A business plan provides a snapshot of your medical device business as it stands today, and lays out your growth plan for the next five years. It explains your business goals and your strategies for reaching them. It also includes market research to support your plans.
Why You Need a Business Plan for a Medical Device Business
If you’re looking to start a medical device business or grow your existing medical device company, you need a business plan. A business plan will help you raise funding, if needed, and plan out the growth of your medical device business to improve your chances of success. Your medical device business plan is a living document that should be updated annually as your company grows and changes.
Sources of Funding for Medical Device Businesses
With regards to funding, the main sources of funding for a medical device business are personal savings, credit cards, bank loans, and angel investors. When it comes to bank loans, banks will want to review your business plan and gain confidence that you will be able to repay your loan and interest. To acquire this confidence, the loan officer will not only want to ensure that your financials are reasonable, but they will also want to see a professional plan. Such a plan will give them the confidence that you can successfully and professionally operate a business. Personal savings and bank loans are the most common funding paths for medical device companies.
Finish Your Business Plan Today!
How to write a business plan for a medical device business.
If you want to start a medical device business or expand your current one, you need a business plan. The guide below details the necessary information for how to write each essential component of your medical device business plan.
Executive Summary
Your executive summary provides an introduction to your business plan, but it is normally the last section you write because it provides a summary of each key section of your plan.
The goal of your executive summary is to quickly engage the reader. Explain to them the kind of medical device business you are running and the status. For example, are you a startup, do you have a medical device business that you would like to grow, or are you operating an established medical device business that you would like to sell?
Next, provide an overview of each of the subsequent sections of your plan.
- Give a brief overview of the medical device industry.
- Discuss the type of medical device business you are operating.
- Detail your direct competitors. Give an overview of your target customers.
- Provide a snapshot of your marketing strategy. Identify the key members of your team.
- Offer an overview of your financial plan.
Company Overview
In your company overview, you will detail the type of medical device business you are operating.
For example, you might specialize in one of the following types of medical device businesses:
- Class 1 medical device: This type of medical device is one that poses low risk to end-users and does not have too many regulatory controls. Stethoscopes and tongue depressors are some examples of Class 1 medical devices.
- Class 2 medical device: This type of medical device could pose higher risk to end-users than Class 1, thus requiring the company to submit a Premarket Notification 510(k) form to the FDA before the product can be sold. Examples of Class 2 medical devices include catheters and surgical tools.
- Class 3 medical device: This type of medical device poses more of a risk to the end-user than Class 1 or Class 2 devices. For this reason, companies selling Class 3 devices must go through a more stringent FDA approval before the product can be sold. Examples of Class 3 devices include cochlear implants and pacemakers.
In addition to explaining the type of medical device business you will operate, the company overview needs to provide background on the business.
Include answers to questions such as:
- When and why did you start the business?
- What milestones have you achieved to date? Milestones could include the number of customers served, the number of products sold, or reaching $X amount in revenue, etc.
- Your legal business Are you incorporated as an S-Corp? An LLC? A sole proprietorship? Explain your legal structure here.
Industry Analysis
In your industry or market analysis, you need to provide an overview of the medical device industry.
While this may seem unnecessary, it serves multiple purposes.
First, researching the medical device industry educates you. It helps you understand the market in which you are operating.
Secondly, market research can improve your marketing strategy, particularly if your analysis identifies market trends.
The third reason is to prove to readers that you are an expert in your industry. By conducting the research and presenting it in your plan, you achieve just that.
The following questions should be answered in the industry analysis section of your medical device business plan:
- How big is the medical device industry (in dollars)?
- Is the market declining or increasing?
- Who are the key competitors in the market?
- Who are the key suppliers in the market?
- What trends are affecting the industry?
- What is the industry’s growth forecast over the next 5 – 10 years?
- What is the relevant market size? That is, how big is the potential target market for your medical device business? You can extrapolate such a figure by assessing the size of the market in the entire country and then applying that figure to your local population.
Customer Analysis
The customer analysis section of your medical device business plan must detail the customers you serve and/or expect to serve.
The following are examples of customer segments: individuals, schools, families, and corporations.
As you can imagine, the customer segment(s) you choose will have a great impact on the type of medical device business you operate. Clearly, individuals would respond to different marketing promotions than corporations, for example.
Try to break out your target customers in terms of their demographic and psychographic profiles. With regards to demographics, including a discussion of the ages, genders, locations, and income levels of the potential customers you seek to serve.
Psychographic profiles explain the wants and needs of your target customers. The more you can recognize and define these needs, the better you will do in attracting and retaining your customers.
Finish Your Medical Device Business Plan in 1 Day!
Don’t you wish there was a faster, easier way to finish your business plan?
With Growthink’s Ultimate Business Plan Template you can finish your plan in just 8 hours or less!
Competitive Analysis
Your competitive analysis should identify the indirect and direct competitors your business faces and then focus on the latter.
Direct competitors are other medical device businesses.
Indirect competitors are other options that customers have to purchase from that aren’t directly competing with your product or service. This includes alternative medical devices and other types of medical device retailers. You need to mention such competition as well.
For each such competitor, provide an overview of their business and document their strengths and weaknesses. Unless you once worked at your competitors’ businesses, it will be impossible to know everything about them. But you should be able to find out key things about them such as
- What types of customers do they serve?
- What type of medical device business are they?
- What is their pricing (premium, low, etc.)?
- What are they good at?
- What are their weaknesses?
With regards to the last two questions, think about your answers from the customers’ perspective. And don’t be afraid to ask your competitors’ customers what they like most and least about them.
The final part of your competitive analysis section is to document your areas of competitive advantage. For example:
- Will you make it easier for customers to acquire your product?
- Will you offer products or services that your competition doesn’t?
- Will you provide better customer service?
- Will you offer better pricing?
Think about ways you will outperform your competition and document them in this section of your plan.
Marketing Plan
Traditionally, a marketing plan includes the four P’s: Product, Price, Place, and Promotion. For a medical device business plan, your marketing strategy should include the following:
Product : In the product section, you should reiterate the type of medical device company that you documented in your company overview. Then, detail the specific products or services you will be offering. For example, will you provide surgical instruments, implants, or test kits?
Price : Document the prices you will offer and how they compare to your competitors. Essentially in the product and price sub-sections of your plan, you are presenting the products you offer and their prices.
Place : Place refers to the site of your medical device company. Document where your company is situated and mention how the site will impact your success. For example, is your medical device business located in a busy retail district, a business district, a standalone building, or purely online? Discuss how your site might be the ideal location for your customers.
Promotions : The final part of your medical device marketing plan is where you will document how you will drive potential customers to your location(s). The following are some promotional methods you might consider:
- Advertise in local papers, radio stations and/or magazines
- Reach out to websites
- Distribute flyers
- Engage in email marketing
- Advertise on social media platforms
- Improve the SEO (search engine optimization) on your website for targeted keywords
Operations Plan
While the earlier sections of your business plan explained your goals, your operations plan describes how you will meet them. Your operations plan should have two distinct sections as follows.
Everyday short-term processes include all of the tasks involved in running your medical device business, including answering calls, meeting with potential customers, scheduling shipments, billing customers and collecting payments, etc.
Long-term goals are the milestones you hope to achieve. These could include the dates when you expect to acquire your Xth customer, or when you hope to reach $X in revenue. It could also be when you expect to expand your medical device business to a new city.
Management Team
To demonstrate your medical device business’ potential to succeed, a strong management team is essential. Highlight your key players’ backgrounds, emphasizing those skills and experiences that prove their ability to grow a company.
Ideally, you and/or your team members have direct experience in managing medical device businesses. If so, highlight this experience and expertise. But also highlight any experience that you think will help your business succeed.
If your team is lacking, consider assembling an advisory board. An advisory board would include 2 to 8 individuals who would act as mentors to your business. They would help answer questions and provide strategic guidance. If needed, look for advisory board members with experience in managing a medical device business.
Financial Plan
Your financial plan should include your 5-year financial statement broken out both monthly or quarterly for the first year and then annually. Your financial statements include your income statement, balance sheet, and cash flow statements.
Income Statement
An income statement is more commonly called a Profit and Loss statement or P&L. It shows your revenue and then subtracts your costs to show whether you turned a profit or not.
In developing your income statement, you need to devise assumptions. For example, will you keep 300 devices on-hand and will sell and restock your inventory every 3 months? And will sales grow by 2% or 10% per year? As you can imagine, your choice of assumptions will greatly impact the financial forecasts for your business. As much as possible, conduct research to try to root your assumptions in reality.
Balance Sheets
Balance sheets show your assets and liabilities. While balance sheets can include much information, try to simplify them to the key items you need to know about. For instance, if you spend $50,000 on building out your medical device business, this will not give you immediate profits. Rather it is an asset that will hopefully help you generate profits for years to come. Likewise, if a lender writes you a check for $50,000, you don’t need to pay it back immediately. Rather, that is a liability you will pay back over time.
Cash Flow Statement
Your cash flow statement will help determine how much money you need to start or grow your business, and ensure you never run out of money. What most entrepreneurs and business owners don’t realize is that you can turn a profit but run out of money and go bankrupt.
When creating your Income Statement and Balance Sheets be sure to include several of the key costs needed in starting or growing a medical device business:
- Cost of equipment and office supplies
- Payroll or salaries paid to staff
- Business insurance
- Other start-up expenses (if you’re a new business) like legal expenses, permits, computer software, and equipment
Attach your full financial projections in the appendix of your plan along with any supporting documents that make your plan more compelling. For example, you might include your business location lease or a list of medical devices in your inventory.
Writing a business plan for your medical device business is a worthwhile endeavor. If you follow the template above, by the time you are done, you will truly be an expert. You will understand the medical device industry, your competition, and your customers. You will develop a marketing strategy and will understand what it takes to launch and grow a successful medical device business.
Medical Device Business Plan FAQs
What is the easiest way to complete my medical device business plan.
Growthink's Ultimate Business Plan Template allows you to quickly and easily write your medical device business plan.
Where Can I Download a Medical Device Business Plan PDF?
You can download our medical device business plan PDF here. This is a business plan template you can use in PDF format.
How Do You Start a Medical Device Business?
Starting a medical device business is easy with these 14 steps:
- Choose the Name for Your Medical Device Business
- Create Your Medical Device Business Plan
- Choose the Legal Structure for Your Medical Device Business
- Secure Startup Funding for Medical Device Business (If Needed)
- Secure a Location for Your Business
- Register Your Medical Device Business with the IRS
- Open a Business Bank Account
- Get a Business Credit Card
- Get the Required Business Licenses and Permits
- Get Business Insurance for Your Medical Device Business
- Buy or Lease the Right Medical Device Business Equipment
- Develop Your Medical Device Business Marketing Materials
- Purchase and Setup the Software Needed to Run Your Medical Device Business
- Open for Business
Don’t you wish there was a faster, easier way to finish your Medical Device business plan?
OR, Let Us Develop Your Plan For You
Since 1999, Growthink has developed business plans for thousands of companies who have gone on to achieve tremendous success. Click here to see how a Growthink business planning consultant can create your business plan for you.
Other Helpful Business Plan Articles & Templates

AI ASSISTANTS
Upmetrics AI Your go-to AI-powered business assistant
AI Writing Assist Write, translate, and refine your text with AI
AI Financial Assist Automated forecasts and AI recommendations
TOP FEATURES
AI Business Plan Generator Create business plans faster with AI
Financial Forecasting Make accurate financial forecasts faster
INTEGRATIONS
QuickBooks (Coming soon...) Sync and compare with your QuickBooks data
Strategic Planning Develop actionable strategic plans on-the-go
AI Pitch Deck Generator Use AI to generate your investor deck
Xero Sync and compare with your Xero data
See how easy it is to plan your business with Upmetrics: Take a Tour →
AI-powered business planning software
Very useful business plan software connected to AI. Saved a lot of time, money and energy. Their team is highly skilled and always here to help.
- Julien López
BY USE CASE
Secure Funding, Loans, Grants Create plans that get you funded
Starting & Launching a Business Plan your business for launch and success
Validate Your Business Idea Discover the potential of your business idea
E2 Visa Business Plan Create a business plan to support your E2 - Visa
Business Consultant & Advisors Plan with your team members and clients
Incubators & Accelerators Empowering startups for growth
Business Schools & Educators Simplify business plan education for students
Students & Learners Your e-tutor for business planning
- Sample Plans
WHY UPMETRICS?
Reviews See why customers love Upmetrics
Customer Success Stories Read our customer success stories
Blogs Latest business planning tips and strategies
Strategic Planning Templates Ready-to-use strategic plan templates
Business Plan Course A step-by-step business planning course
Help Center Help & guides to plan your business
Ebooks & Guides A free resource hub on business planning
Business Tools Free business tools to help you grow
Tips for Choosing the Right Business Plan Consultant

Free Business Plan Template
- June 24, 2024

Find yourself staring at the blank screen while writing your business plan? Well, every entrepreneur feels that once in their business journey. This is where a business plan consultant comes into the picture.
Think of a business plan consultant as your strategic partner who helps you craft the plan and create strategies that help you with funding.
But the tricky part is: How do you choose the right business plan consultant? Because there are a lot of options that will confuse you.
Worry not, here are the tips for choosing the right business plan consultant through which you can examine and select the right one for your business.
But before that let us understand why it’s important to hire a consultant.
Why do I need a business plan consultant?
A business plan consultant works closely with you and understands your business thoroughly. They help you achieve your goals like expanded market share, cost reduction, enhanced customer experience, and more.
Consultants have experience in various industries and expertise in fields like marketing, strategic planning, and more. So, having a consultant by your side will lead you to a successful business.
So, as we know why we need a business plan consultant, let’s move ahead to the tips.
8 Tips for choosing the right business plan consultant
Are you too facing the issues in choosing the right business plan consultant ? Well, there are many options online and offline for a consultant, so let’s see how to choose “the one” for your business:
1. Experience and expertise
First, look into which industries the business plan consultant has experience in. Also, consider their expertise, and see if it is relevant for your business.
Go for industry-specific experience, as this ensures familiarity with the unique problems and opportunities related to the industry.
Also, see if they have any successful track record in similar projects in the same industry. Lastly, review their portfolio for detailed strategic plans customized for a business like yours.
2. Check qualifications
Before finalizing the business plan consultant, ensure they have the qualifications that you’re looking for. Go for a solid educational background, such as degrees in business, finance, or related fields, which is necessary for your industry.
Also, check if the consultants have any additional training and memberships in any professional organizations.
3. Review ratings and feedback
Explore recommendations and reviews of the consultant, before you finalize them. If you have word-of-mouth referrals from other businesses then it is a plus, as they come authentically.
Also, scan online reviews and get to know about the consultant’s methodology. All of these combined act as evidence of the consultant’s past work, process, and credibility.
4. Consider compatibility
Look for a consultant who not only has the necessary skills and expertise but communicates effectively. A compatible consultant will be able to offer personalized advice that resonates with your vision, ultimately leading to a more successful output.
5. Verify their process
Understanding the approach of the consultant is essential to ensure a successful outcome. It’s important to verify that their process includes comprehensive research, data analysis, and a clear strategic plan.
Requesting a detailed outline of the process along with the expected timeline can help you understand their method and set clear expectations.
6. Discuss fees and contracts
Discussing fees and contracts before hiring a consultant maintains transparency. You need to clearly understand their fee structure and what it covers.
Apart from that, make sure the contract clearly states what you’ll get, when you’ll get the plan, and how much you’ll have. This clarity helps prevent misunderstandings and potential disputes later on.
7. Review sample plans
Request sample business plans from the consultant to evaluate their work. This will help you know their writing style, attention to detail, and overall professionalism.
By going through their past work, you can consider whether their process syncs with your expectations and requirements.
8. Know their knowledge
Here you should get to know about the consultant’s knowledge by asking certain specific questions from the industry like:
- How do you update yourself with all the industry changes and trends?
- Can you please explain a complex concept of the business and how you plan to apply the same in my business?
- What metrics or KPIs are the most important for you and which you will use for my business?
Also, look into if they can provide you with in-depth replies to your questions.
That’s it guys! I hope following the above tips will help you choose the right business plan consultant for your business.
But, if you don’t want to go to and for for your business plan, you can write it on your own with the help of a business planning software like Upmetrics .
This tool helps you with business planning, creating financial forecasts, strategic planning, and a lot more.
So, why not write your business plan on your own? Start planning today.

Sample Business Plan Library
Explore over 400 real-world business plan examples from a wide variety of industries.

One Page Business Plan Template
Use this simple one-page business plan template to immediately get started on your plan.

Free Startup Business Plan Template
Use this simple startup business plan template to immediately get started on your plan.
Frequently Asked Questions
Can a business plan consultant help with funding.
Yes, a business plan consultant helps you with writing engaging business plans which ultimately supports you in attracting investors and banks for funds.
How long does it take to complete a business plan?
It might take around weeks, months, or even more for a business plan consultant or a writer to create a business plan for your business. However, with the AI-powered business planning tool like Upmetrics, you can write your plan in days.
Should I pay someone to write my business plan?
Paying someone or not depends on your budget and requirements. But you can write your business plan professionally for just as low as $7 with Upmetrics.
What kind of information do I need to provide to the consultant?
You need to provide the history of your business, product or services, target market, competitors, marketing strategies, financial projections, operational details, legal requirements, and more—for them to understand your business.
About the Author
Upmetrics Team
Upmetrics is the #1 business planning software that helps entrepreneurs and business owners create investment-ready business plans using AI. We regularly share business planning insights on our blog. Check out the Upmetrics blog for such interesting reads. Read more
Reach Your Goals with Accurate Planning
- Marketplace
- Business Consulting Firms
Top California Business Consulting Firms
Best california business consulting company rankings.

TruAdvantage

Kanda Software

Naked Development

Tusk Creative Studios

Crystal Pyramid Productions
Need help selecting the right agency for your project.

Sigma Software

Startup House

Healthcare Success

Brenton Way

Premier BPO

Ludwig Marketing & Sales

Use All Five

PRA Public Relations

Disruptive Advertising

Dynamic Wave Consulting

SEO Seagull

Designotion.com

Eide Bailly

Search Traffic Success

Challenge.IS - Marketing Agency, Web Design and SEO Company

ProMailing Solutions

The Hoyt Organization

Zenith Strategic Global Partners

MAKO Design + Invent

CodeStringers

Red Slice, LLC

Kingsmen Digital Ventures

Grant Thornton

Insurance Support World

Polaris Marketing & Consulting

TMS Business Solutions

CIENCE Technologies

Janet Guerriero Marketing Solutions
-logo-listing.jpg)
ChrisRubinCreativ (CRC)
Top Business Consulting Firms in California:
- Los Angeles
- San Francisco
- Orange County
Related Service Providers in California:
- Accounting Firms in California
- Advertising Agencies in California
- Big Data Companies in California
- BPO Companies in California
- Branding Agencies in California
- Cloud Consulting Companies in California
- Conversion Rate Optimization Agencies in California
- CRM Consultants in California
- Custom Software Development Companies in California
- Customer Service Outsourcing Companies in California
- Design Agencies in California
- Digital Marketing Agencies in California
- ECM Consultants in California
- ERP Consultants in California
- IT Services Companies in California
- Managed IT Service Providers in California
- Market Research Companies in California
- Media Buying Agencies in California
- Video Production Companies in California
- Web Design Companies in California
Nearby Locations:
- Business Consulting Firms in Arizona
Latest Trends Related to Business Consulting

Don't bother with copy and paste.
Get this complete sample business plan as a free text document.
Medical Billing Business Plan
Start your own medical billing business plan
Physicians 1st Billing and Claims
Executive summary executive summary is a brief introduction to your business plan. it describes your business, the problem that it solves, your target market, and financial highlights.">.
Billing services currently exist to manage medical practices. These services relieve medical professionals of tedious detail work, but rarely do they offer a means to substantially maximize the practice’s bottom line. Physicians 1st Billing and Claims will not only free office staff for more crucial tasks, but will also maximize return from insurance carriers.
National statistics show only about 70 percent of insurance claims, initially submitted on paper, are ever paid by insurance carriers. With electronic submission Physicians 1st Billing and Claims can increase the percentage of claims paid to around 98 percent.
Additional statistics indicate that it currently costs a medical practice between $8.00-$10.00 per claim to process insurance for their patients. Physicians 1st Billing and Claims can reduce these costs by 50 percent or more.
Statistics show turnaround on paper insurance claims to be 30, 60, even 90 days or longer, creating serious outstanding receivables for the practice. By submitting claims electronically, Physicians 1st Billing and Claims can generally have money in the physician’s hand within 14-18 days. Of course, this reduces outstanding receivables proportionately and tremendously improves cash flow.
Statistics also show a 30 percent suspension/rejection rate for paper insurance claims. This doesn’t mean that the claims are never paid. What it does mean is medical staff must hassle with insurance carriers over payment. With the extensive editing performed on electronic claims prior to their transmission to carriers, this percentage is reduced to 2-3 percent. Claims are submitted with a 98 percent accuracy rate.
For many years physicians graduated from medical school under the premise that they were going to run a “practice.” “Businesses” were for other professionals. Many simple administrative procedures were neglected, such as:
- Keeping current with insurance specifications and regulations, so that claims were paid on a timely basis,
- Concentrating on collecting receivables and co-payments,
- Ensuring that fees were kept at the maximum allowable insurance carriers were paying, or
- Procedure codes were current so that claims weren’t suspended or rejected.
For many offices, outstanding receivables grew tremendously and annual bad-debt write-offs became routine. But adequate profit margins allowed medical practices to ignore sound business procedures. Medical practice complacency toward industry change is in the past. Physicians’ heads raised and they began taking note of public opinions toward health care reform issues four years ago. With the onslaught of managed care organizations into the industry, physicians are finding profit margins shrinking. They are now alert to the fact that in order to remain in business into the 21st century, they will have to adopt more efficient business practices. Physicians 1st Billing and Claims is prepared to assist local health care providers move through the last of the 20th century and into the 21st century with sound practices that will guarantee business success and, in turn, guarantee quality health care for our families and our country.
Physicians 1st Billing and Claims is contributing over $9,000 to this business. We are requesting to borrow another $5,000. Please give this detailed business plan your attention. The use of these funds is explained in the Start up Summary section.
1.1 Objectives
- To acquire one account by the end of month two.
- To process 1,500 claims a month by month 15.
- To become recognized as a local industry expert in the field of medical reimbursement.
- Code optimization.
- Managed care contract analysis.
- Full practice management.
- Customized reporting.
- Medical transcription.
- Fee analysis.
- Medicare financial impact analysis.
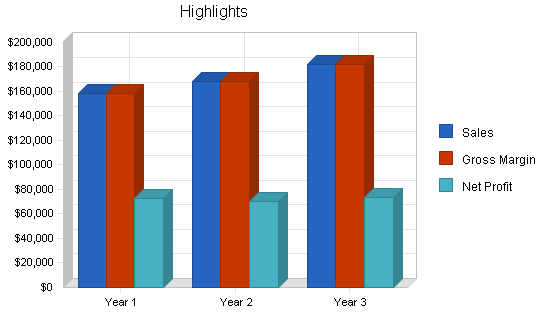
1.2 Mission
Physicians 1st Billing and Claims is a medical reimbursement consulting firm dedicated to helping medical practices become more efficient and save money by allowing them to out-source their insurance processing and medical billing to an expert reimbursement service. We intend to have complete one-stop-shopping for all medical practice administrative functions by the end of 1998. We intend to make enough profit to repay our business-start-up loan and finance continued growth and development with our quality service.
1.3 Keys to Success
Since 1985, the Federal Government has been urging the health care industry to submit insurance claims electronically. Statistics prove that electronic submission can save millions of dollars annually for the industry. Presently, 95 percent of all pharmaceutical claims and 70 percent of hospital claims are submitted electronically. Physicians and dentists trail far behind, with only 25-30 percent.
The Federal Government is not happy with this situation so in 1990, Congress mandated that physicians are required to file claims on behalf of all their Medicare patients. Many doctors were not prepared for this deluge of paperwork. Eight years later doctors are still climbing out from under the paperwork. In 1996 the motions calling for electronic submission of all Medicare claims were being echoed throughout the halls of congress. No mandate was passed but the paperwork continues to mount up and as baby boomers near retirement age the paper problem will only get worse and those echoes will turn into screams. This year in the U.S. over 1 trillion dollars worth of medical charges will be issued. This amounts to 9 billion medical claims. Medical practices will be forced to meet the mandates, and growing mountains of paper and most are not currently equipped to handle the transition. The sensible solution is to out-source the process to experts that are prepared to save the practices money, produce a much faster return from insurance carriers, and handle the claims with a high degree of accuracy. There aren’t many businesses that can say the Federal Government is behind them all the way.
A second key to our success will be flexibility. Physicians 1st Billing and Claims understands that each medical practice is unique. Even practices of the same specialty will have different staff and offer different services. Physicians 1st Billing and Claims will evaluate the needs of each practice and offer solutions to help the practice become more efficient. Some may want all the services we offer and some may select only a few. Our billing will be customized to each office’s needs.
A third key is our diversified services. Physicians 1st Billing and Claims offers a one-stop-shopping experience for medical administrative services.
Company Summary company overview ) is an overview of the most important points about your company—your history, management team, location, mission statement and legal structure.">
We are currently organized as a partnership, being formed in October, 1998.
Physicians 1st Billing and Claims and the logo shown on the cover of this plan are trade marked through the U.S. Department of Commerce Patent and Trade Mark Office. The trademark covers Medical Practice Management and Reimbursement Consulting.
2.1 Company Ownership
The two individuals forming this partnership are John and Mary Biller, a husband and wife team.
John’s experience consists of three years of teaching experience, 13 years managerial experience in the Building Materials industry, and 12 years as a father. As a manager, John gained experience in marketing, back-office operations, sales, and managing people. John will use this experience in managing the Marketing and Sales departments.

2.2 Start-up Summary
Physicians 1st Billing and Claims start up will focus on John and Mary working full-time in the business.
John’s main duties will center on marketing/sales, purchasing, and data entry. Mary’s main duties will center on data entry, clerical administration, and training. John and Mary will jointly assume the accounting responsibilities. The children, Erika and Matthew, will work when needed in data entry and housekeeping. The entire Biller family is dedicated to ensuring the success of Physicians 1st Billing and Claims.
John and Mary have decided to purchase a business opportunity package offered by Claim Systems Inc. The price of this package includes: state of the art medical billing and accounting software, unlimited training for the first six months, two years of 24-hour technical support, emergency support service, and a full-featured marketing package. The price of the package is $5,000.00 plus $45.00 for shipping and handling. Optional dental billing software can be purchased for $900.00 plus shipping. This software will be added at a later date. An additional deposit of $400.00 will be included at time of purchase of the package to secure the rights to become a franchise once Claim Systems receives licensing from the State of Indiana. At such time as Claim Systems receives this approval, Physicians 1st Billing and Claims will pay an additional $1,595.00 for ownership of franchise rights from Claim Systems. The benefits of this will allow us to advertise nationally and establish name recognition.
John owns a Pentium II Gateway computer with ink-jet printer and a scanner that will be utilized for the business. The following additional office equipment will be purchased: a Pentium computer, an ink-jet printer, a fax machine, assorted phone and communications equipment, a chair, a copy machine, accounting software and misc. office supplies.
John and Mary are investing $9,640 of their own capital in the business, and are looking for a four-year loan for an additional $16,000 which they feel will be necessary to successfully start Physicians 1st Billing and Claims.
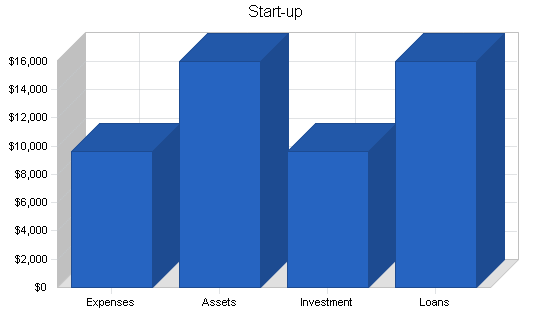
| Start-up | |
| Requirements | |
| Start-up Expenses | |
| Legal | $200 |
| Office Supplies Stationery | $200 |
| Furniture | $500 |
| Business Opportunity | $6,040 |
| Insurance | $200 |
| Rent | $50 |
| Software | $69 |
| Expensed Equipment | $345 |
| Other | $2,000 |
| Total Start-up Expenses | $9,604 |
| Start-up Assets | |
| Cash Required | $16,000 |
| Other Current Assets | $0 |
| Long-term Assets | $0 |
| Total Assets | $16,000 |
| Total Requirements | $25,604 |
| Start-up Funding | |
| Start-up Expenses to Fund | $9,604 |
| Start-up Assets to Fund | $16,000 |
| Total Funding Required | $25,604 |
| Assets | |
| Non-cash Assets from Start-up | $0 |
| Cash Requirements from Start-up | $16,000 |
| Additional Cash Raised | $0 |
| Cash Balance on Starting Date | $16,000 |
| Total Assets | $16,000 |
| Liabilities and Capital | |
| Liabilities | |
| Current Borrowing | $16,000 |
| Long-term Liabilities | $0 |
| Accounts Payable (Outstanding Bills) | $0 |
| Other Current Liabilities (interest-free) | $0 |
| Total Liabilities | $16,000 |
| Capital | |
| Planned Investment | |
| Owners | $9,604 |
| Investor | $0 |
| Additional Investment Requirement | $0 |
| Total Planned Investment | $9,604 |
| Loss at Start-up (Start-up Expenses) | ($9,604) |
| Total Capital | $0 |
| Total Capital and Liabilities | $16,000 |
| Total Funding | $25,604 |
2.3 Company Locations and Facilities
John and Mary will be utilizing 518 sq. ft. (an extra large bedroom in the upstairs) of their home. John’s office area will be utilized for marketing and accounting operations. Mary’s office area will be utilized for data entry and clerical operations, etc.
Our position in the market will be a full-service medical reimbursement business with individual pricing. As stated previously, our goal is one-stop shopping for medical practices when it comes to administrative functions. Physicians 1st Billing and Claims Electronic Claims Service’s policy is to customize our charges based on the work we do, and the needs of each office. We find that each practice is unique and, therefore, we do not quote a “standard charge” for services.
Initially, Physicians 1st Billing and Claims will offer electronic billing of medical insurance claims. This is a badly needed service for most medical practices, and is even more critical since the Federal Government will mandate electronic submission of Medicare claims in the near future.
A detailed description of the electronic submission process follows. The data necessary to submit claims will be downloaded from the medical office and input into specialized computer software. The software performs certain generic edits on the data and stores the information. When a batch of claims is complete for an office, it is time to transmit to the national clearinghouse. The data travels via modems and telephone lines to the clearinghouse where the data is edited a second time. This second series of edits incorporates “insurance company specific edits.” Cooperating insurance carriers notify the clearinghouse of certain edits they feel are necessary to allow payment of their claims. These edits are performed on each claim before they are transmitted on to the carrier, thus guaranteeing accuracy and payment in most cases. Upon receiving the insurance claim from the clearinghouse, the carriers process the claim and send payment directly to the medical practice. With electronic transmission to the clearinghouse and on to the carrier, computerized data verification, and elimination of most of the human element, the process of claims payment is greatly simplified and accelerated. Physicians will no longer wait 30, 60 or 90 days for payment, but will have money in their hands usually within 14-18 days.
As practices begin experiencing the benefits of electronic submission, many will see the advantage of out-sourcing other administrative functions. Physicians 1st Billing and Claims’ full-featured practice management software will allow us to meet those needs. Patients can be billed for co-payments or amounts which their insurance company did not cover. Secondary and supplementary insurance can be tracked and payments and balances applied accurately. The software utilizes state-of-the-art, open-item accounting, where most other systems use balance-forward systems. Outstanding receivables can be tracked with insurance aging reports, in several different sequences for ease of use. A complete practice analysis will increase office efficiency by showing where money is coming from. For each procedure, the charges and percentage of total charges they represent are calculated and printed for immediate reference. Transaction Journals and Detail Ledgers provide an accurate overall picture of the practice.
With managed care sweeping the country, it is imperative for medical practices to evaluate the benefits they receive from affiliation with different organizations. Our managed care contract service tracks payments and analyzes the information to produce customized reports showing profitability, or lack of profitability, with each managed care facility. These reports are critical when decisions need to be made on renewing and negotiating contracts.
Claim Systems’ state-of-the-art software will allow the physician to do complete dictation transcription. This allows the physician to meet the needs of the new strict HCFA mandate on clarity of all Medicare claims.
3.1 Service Description
Physicians 1st Billing and Claims’ number one goal is to provide outstanding service.
We show our dedication to service by providing the physician one-stop shopping for all his or her billing and claims needs. The services we provide are as follows:
- Complete patient record setup.
- Electronic and manual medical claims filing.
- Patient billing.
- Claims posting and patient record updating.
- Collection services.
- Complete practice analysis.
- Assistance in negotiating health care contracts.
- Automated transcription service.
- Volume discounting.
Initially we will focus on just claims filing. In the near future we will diligently pursue our goal of providing one-stop shopping for physicians’ medical office management.
3.2 Competitive Comparison
An evaluation is performed on each medical practice during the marketing phase. This will allow us to determine the needs of the practice and how to charge for services rendered.
During the evaluation certain facts are gathered, such as:
- The time it will take to key patient and claims information into the software.
- The approximate number of claims a practice will submit monthly.
- The approximate “total dollars” a practice submits monthly to insurance carriers.
- How accurate is the information obtained from the office (is it complete and easy to enter or does it require extensive editing and follow-up?).
- How often will the information need to be gathered (based on claims volume).
- What method is best to collect the information (personally, mail, FAX, Federal Express, downloading via modems).
- What other services may interest the practice.
3.3 Sales Literature
Included in the appendix to this plan are copies of Physicians 1st Billing and Claims’ sales brochure and tips brochure. These brochures were developed with the expertise of a national marketing company specializing in medical reimbursement issues. The sales brochure will be used in conjunction with sales calls. Physicians 1st Billing and Claims’ Tips brochure will be utilized as a direct mail piece. Also included are copies of business cards and stationery.
3.4 Technology
The computer software that is the crux of Physicians 1st Billing and Claims’ medical reimbursement business is state of the art. Physicians 1st Billing and Claims is running in Windows 95. The software was specifically developed as a tool for medical reimbursement consultants. This is important because some software being sold is written to manage a doctor’s office and does not necessarily incorporate all functions that are needed for consultants. The software also includes the latest features needed for managed care organization management, including tables for the numerous fee schedules which may be required, and customized reports to evaluate contacts.
The ET&T clearinghouse, which verifies the claims data, is highly respected in the industry. They are members of and have been certified by AFECHT, a national policing organization. They utilize the American National Standards formats recognized by Medicare and most commercial insurance carriers. They guarantee claims are 98 percent accurate before being sent on to carriers.
3.5 Future Services
As stated earlier in 3.1, Mary and John plan to initially process claims manually and electronically. As they gain experience, they will offer full medical office consulting services as follows:
Market Analysis Summary how to do a market analysis for your business plan.">
Physicians 1st Billing and Claims’ target market consists of any medical practice or health care delivery unit that utilizes the HCFA-1500 format (a national standard utilized by Medicare) for submission of claims. This includes family practice, internal medicine, surgeons, psychologists, chiropractors, physical therapists, podiatrists, specialists, ambulance services, medical laboratories, etc. Physicians 1st Billing and Claims can also process claims for dentists with the use of special ADA software.
New practices are particularly appealing as Physicians 1st Billing and Claims can assist the new physician and his or her staff in billing and claims training. By equipping the physicians with a a well trained staff in claims handling and putting an efficient billing program into place, Physicians 1st Billing and Claims can reduce the stress of start up and ensure greater likelihood of a practice’s success due in part to increased cash flow.
4.1 Market Segmentation
The following is a chart showing the number of physicians in (omitted) for each speciality mentioned.
Number and Specialty
5 Allergy-Immunology 47 Anesthesiologist 3 Cardiovascular 12 Cardiovascular Surgery 84 Chiropractors 1 Clinical Genetics 2 Child Psychiatry 1 Clinical Immunology 5 Colon Rectal Surgery 10 Critical Care Medicine 179 Dental 11 Dermatology 1 Diabetes 35 Diagnostic Radiology 1 Education 21 Emergency Medicine 16 Ear, Nose and Throat 114 Family Practice 30 Family Practice Residents 1 Family Practice Sports Med. 12 Gastroenterology 10 Geriatrics 22 General Surgery 1 General Surgery Burns 7 Gynecology 7 Hematology 4 Infectious Diseases 40 Internal Medicine 10 Neurology 12 Nephrology 4 Neonatal-Prenatal Medicine 3 Nuclear Radiology 9 Neurological Surgery 26 Obstetrics 1 Obstetrics & Gynecology Resident 1 Occupational Medicine 3 Oncology 22 Ophthalmology 35 Orthopedic Surgery 7 Orthopedic Surgery Resident 14 Optometry 24 Pediatrics 14 Psychiatry 49 Psychologists 1 Pediatrics Pulmonary 6 Physical Med. & Rehab. 15 Physical therapy 1 Pediatric Nephrology 9 Plastic Surgery 21 Pathology 11 Pulmonary 3 Rheumatology 6 Therapeutic Radiology 13 Thoracic Surgery 14 Urology 12 Vascular Surgery
Physicians 1st Billing and Claims’ initial plan is to sign a single doctor practice. An ideal target would be a family practice physician.

| Market Analysis | |||||||
| Year 1 | Year 2 | Year 3 | Year 4 | Year 5 | |||
| Potential Customers | Growth | CAGR | |||||
| Physicians | 2% | 867 | 884 | 902 | 920 | 938 | 1.99% |
| Dentists | 2% | 179 | 183 | 187 | 191 | 195 | 2.16% |
| Other | 2% | 18 | 18 | 18 | 18 | 18 | 0.00% |
| Total | 1.98% | 1,064 | 1,085 | 1,107 | 1,129 | 1,151 | 1.98% |
4.2 Service Business Analysis
The Federal Government’s influence is quite positive. In May, 1992, the Health Care Financing Administration, the governing body for Medicare, established what they call “payment floors” for Medicare claims. Carriers contracted to pay Medicare claims were told to hold paper claims’ payments until “at least the 27th day after receipt.” Electronic claims were to be held until the 14th day, but had to be paid by the 19th day. If “clean claims” (claims that are error free) were not paid by the 19th day after receipt, the Federal Government would have to pay interest on the claim amount. No payment penalties were placed on paper claims. Program Memorandum AB-92-5 described above, was beneficial for the electronic medical claims industry.
Several states have passed mandates of their own since 1992, but until now there has been no real action by the Federal Government on this issue. As stated earlier, it is expected that Congress will mandate electronic submission of Medicare claims in the near future and the cut-off date for paper claims will follow soon after. After the cut-off date, paper Medicare claims will not be accepted.
If history is any indication and current trends continue, commercial insurance carriers will follow suit within a short period of time. It is in their best interest as well. Statistics show that it currently costs a commercial carrier between $2.60 to $20.00 to process a claim. The same claim can be processed electronically for approximately $1.10. The conversion costs of moving from paper to electronic processing can be extensive, but in the long run these savings will be substantial.
4.2.1 Main Competitors
Our main competition is Bi-State Medical Consulting. They provide full service medical claims management.
Their strengths are:
- Experience.
- Large client base.
Their weaknesses are:
- One-way claims communication and software.
- Limited advertising ability.
The strengths and weaknesses, however, seem of little consequence as the local market by all accounts is untouched, and no other company in this area can offer the software features or the dedicated service that Physicians 1st Billing and Claims is able to offer.
The bottom line of our ability to compete lies in our ability to provide any and every physician with free practice management software, two-way computer communications which allow for next day patient records updating, and substantially improved cash flow for the physician.
4.2.2 Business Participants
If Congress does mandate electronic submission of insurance claims during 1998, 600 physicians will be scrambling to meet the mandates. Since October, 1990, physicians treating Medicare and Medicaid patients have been required by law to file the necessary claims for these individuals. If practices are unable to meet the mandates, they will lose a good portion of their patient base.
During the past few years, medical practice’s interest in Total Quality Control (TQC) has intensified. Part of this is attributed to the Federal Government and the American public’s interest in health care reform. Physicians fear that if they do not voluntarily comply, more Federal regulations will be imposed.
The managed care movement across America is also influencing medical practices. In the past, doctors personally decided what they would charge for services rendered. For many physicians this fee-for-service payment method is a thing of the past. With managed care, physicians sign contracts and affiliate with different health maintenance organizations (HMOs) or preferred provider organizations (PPOs). Most decide to affiliate for one of two reasons:
- Their peers are doing it and they do not want to be left out, or
- They feel it will increase their patient base.
Strategy and Implementation Summary
Studies show that the No. 1 issue with consumers today is “personal service.” They are tired of robotic salespeople, hollow sales promises, and mediocre support from unresponsive technical staff. They want to know that someone really cares about their concerns and wants to resolve their problems. They want thoroughly thought out solutions that reap benefits. And they want it when they want it. Physicians 1st Billing and Claims understands this because we have been in their position.
Physicians 1st Billing and Claims also understands that they want a reasonable price for services. That is why Physicians 1st Billing and Claims takes the time to evaluate the needs of each medical office and then we customize our service and our charges, based on needs. We need to make sure we are not overcharging or undercharging. If we’re overcharging, then the client will not be happy. If we’re undercharging, then we won’t be happy and we probably won’t do a good job. What we’re looking for is win-win, long-term relationships with our clients. Zig Ziglar, noted sales trainer, asks the question, “Would you buy from you? Are you the type of business that you would like to do business with?” Physicians 1st Billing and Claims feels we are the type of company that anyone would be happy to do business with.
5.1 Competitive Edge
Physicians 1st Billing and Claims can provide the following benefits:
- Free State-Of-The-Art Practice Software.
- Two-way Computer Communications.
- Next Day Patient Record Updating.
- Complete Practice Analysis.
- Full Service Medical Claims Management.
- Superior Service.
No one else in the local market can offer this service package.
5.2 Marketing Strategy
There is a marked increase in results when multiple items are used in concert to attain your goal, a contract for services between you and a health care practice.
The basic plan is divided into five segments:
- Contacting the medical practice for the first time.
- Identifying the gatekeeper and making contact with them.
- Mailing or dropping off information
- Three-panel brochure.
- Self mailer.
- Promotional letter.
- Scheduling an appointment for a presentation.
- The presentation.
Contacts to implement this marketing strategy will be from a prior developed database of physicians who currently do not file medical claims electronically. This information is obtained from public records.
5.2.1 Promotion Strategy
We believe it is much smarter for a medical practice to out-source the detail work of insurance processing to an expert medical reimbursement service instead of trying to make the transition to in-house processing themselves. For years medical practices have been relying on the expert advice of accounting services for tax issues and financial planning. These areas have become very complicated and expertise is needed to ensure judicious decisions. Insurance processing has become very complicated as well, and physicians need to begin relying on expert services to maximize their reimbursement from insurance carriers.
Most medical offices are computerized to the degree that they own a computer and software with capabilities to set appointments, bill patients, and print paper insurance claims. Most do not have capabilities to transmit claims electronically or scientifically evaluate managed care contracts, and the transition is expensive.
Their current software and system have been very stable, and for years may not have even required a software update. Electronic claims submission is a very volatile and different industry requiring frequent software modifications to stay abreast of industry changes. Expertise and time is required over and above what the normal medical office can afford.
For most offices the transition would begin with buying new hardware (or updating the old), claims software, modems, communications software, etc. Very likely the current medical staff will not have the expertise to handle upgrades, install programs, test modems, understand baud rates, conduct initial testing, and other essential skills. This means the office has to hire someone with these skills or retain an expensive support service. With the high turnover of personnel that most medical offices currently experience, retaining another type of employee adds a completely new dimension.
The logical solution to meeting Federal mandates and to process all claims electronically, is to contract with an expert electronic medical billing and reimbursement service. This allows current office staff to resume the tasks they were trained to do, such as assist patients and doctors.
5.2.2 Marketing Programs
With a service-oriented business such as this, clients must be brought on one at a time. The full practice analysis will be conducted with each need being identified. Charges will be negotiated based on these needs. When we have successfully met the needs of each practice, the practice will be more inclined to promote our business to other medical practices that would benefit from our service. Studies have shown that the most common way to expand a medical reimbursement business is through referrals from current clients.
In addition to the on-going program discussed above, Physicians 1st Billing and Claims will incorporate numerous other strategies simultaneously.
In general they are:
- A listing in the local Yellow Pages. We realize the importance of stability and professionalism; anyone who has been in business any length of time can be located in the Yellow Pages. We will only be utilizing a one-line listing for we feel this will not be the main source of clients contacting us, but will provide the professional appearance we need.
- Networking as members of the Chamber of Commerce, local civic organizations, county medical associations.
- Attending and volunteering services for medical fundraisers and health fairs, maintaining an information booth at local medical trade shows.
- Attending Medicare, Medicaid, Blue Shield and Worker’s Compensation activities.
- Networking with other professionals, such as medical and professional consultants, attorneys, and accountants whose clientele is predominately medical, pharmaceutical representatives, and medical equipment salespeople.
- Affiliation with local and national peer organizations, including those available on the Internet.
- Advertising in local/hospital newsletters.
- Membership in the Better Business Bureau.
- Accepting an invitation to appear on a local radio talk show.
- Submitting several press releases annually to local newspapers.
- Writing articles for several health publications in the area.
5.2.3 Pricing Strategy
Physicians 1st Billing and Claims’s pricing strategy is a two part program:
Part 1: The first question that must be asked in the negotiation process is, “Does this practice want complete claims management?” If the answer is yes, Physicians 1st Billing and Claims will negotiate services based on a percentage. Usually the percentage will be from 6 to 10 percent based on the size of the practice.
Part 2: If the practice simply wants claims filing, the pay-for-services rendered will be based on a sliding scale with ranges between $3.50 and $5.00. This scale is divided as follows:
| 1-99 | $5.00 |
| 100-199 | $4.50 |
| 200-299 | $4.25 |
| 300-399 | $4.00 |
| 400+ | $3.50 |
A one time setup charge between $150.00 and $500.00 based on patient load will be assessed and will be due at contract signing.
5.3 Sales Strategy
The following graph and chart reflect the realistic goals we have set.

| Sales Forecast | |||
| Year 1 | Year 2 | Year 3 | |
| Unit Sales | |||
| Service 1 | 33,000 | 48,000 | 52,000 |
| Service 2 | 28,800 | 0 | 0 |
| Total Unit Sales | 61,800 | 48,000 | 52,000 |
| Unit Prices | Year 1 | Year 2 | Year 3 |
| Service 1 | $3.50 | $3.50 | $3.50 |
| Service 2 | $1.50 | $1.50 | $3.50 |
| Sales | |||
| Service 1 | $115,500 | $168,000 | $182,000 |
| Service 2 | $43,200 | $0 | $0 |
| Total Sales | $158,700 | $168,000 | $182,000 |
| Direct Unit Costs | Year 1 | Year 2 | Year 3 |
| Service 1 | $0.00 | $0.00 | $0.00 |
| Service 2 | $0.00 | $0.00 | $0.00 |
| Direct Cost of Sales | |||
| Service 1 | $0 | $0 | $0 |
| Service 2 | $0 | $0 | $0 |
| Subtotal Direct Cost of Sales | $0 | $0 | $0 |
5.4 Strategic Alliances
Physicians 1st Billing and Claims is a franchise affiliated with the nationally known Medical billing franchise. This affiliation allows us to take advantage of the prestige and experience associated with the national company. Included with affiliation is:
- Full-accounting, state-of-the-art medical billing software (Windows based) that includes patient billing, specialized reports, superbill generation, electronic claims, open-item accounting, patient recall, mailing labels, patient scheduling, and graphics capabilities.
- One year, toll-free telephone support for software, claims processing and marketing strategies.
- One year software updates, rewrites, and new manuals.
- A library of current medical insurance carriers.
- A library of current CPT (procedure) codes.
- A library of current ICD-9-CM (diagnosis) codes.
- Flash Code for Windows (software that handles extensive validity checking on procedure and diagnosis codes).
- Clearinghouse registration for claims processing centers and first medical practices.
- Dental electronic claims software.
- Marketing manuals, audio tapes, and supplemental marketing materials.
- Computer software to help in designing innovative marketing brochures.
- Personalized help in designing marketing materials.
- Updates to keep us informed concerning changes in the health care industry.
- Computer software to calculate what it currently costs a medical practice to provide insurance processing for patients and to help calculate customized charges for medical practices.
- Invoicing software.
- Contact management software.
5.5 Milestones
See Milestone table.
| Milestones | |||||
| Milestone | Start Date | End Date | Budget | Manager | Department |
| First Client | 10/1/1998 | 10/30/1998 | $1,200 | John & Mary Biller | S&M |
| Second Client | 10/30/1998 | 11/30/1998 | $1,200 | John & Mary Biller | S&M |
| Third Client | 11/30/1998 | 12/30/1998 | $1,200 | John & Mary Biller | S&M |
| Fourth Client | 12/30/1998 | 1/30/1998 | $1,200 | John & Mary Biller | S&M |
| Fifth Client | 1/1/1999 | 2/1/1999 | $1,200 | John & Mary Biller | S&M |
| Totals | $6,000 | ||||
Management Summary management summary will include information about who's on your team and why they're the right people for the job, as well as your future hiring plans.">
As stated earlier in the section on Company Ownership, the primary management of the company will be handled by John Biller. As President of Physicians 1st Billing and Claims, John brings 16 years of management experience to his position. John holds a Bachelor of Science degree from Ball State University in Education. John’s education and experience in the medical field come from his extensive training in Physiology and Anatomy as a major part of a Health Science degree. John managed Big Timber Building Materials from 1982 to 1995. Having been responsible for sales in excess of $12 million, John is more than capable of leading Physicians 1st Billing and Claims to the Number 1 billing and claims processing firm in the local area. John will handle all marketing and sales functions. John will oversee the data processing, training, accounting, and computer departments.
Mary will serve as the Chief Operating Officer of administration and clerical. Mary brings 18 years of valuable experience to her administrative post. Mary holds a Bachelor of Science degree from Ball State University in Education. Mary has successfully organized and headed many community endeavors that without her foresight would never have achieved their intended goals. Mary will mainly be responsible for initial tele-marketing, data entry, customer service, and disseminating of company information. Mary has 13 years in medical claims filing and three years in secretarial training; both lend themselves well to the departments she will head up. Physicians 1st Billing and Claims and its customers are in good hands with Mary’s leadership.
6.1 Personnel Plan
John and Mary will assume full-time management of and employment at Physicians 1st Billing and Claims.
Two other part-time employees who are equally as valuable for the roles they will play in the operations of Physicians 1st Billing and Claims are Erika and Matthew Biller. Erika will assume some data entry duties and facility maintenance duties. Matthew will assume facility maintenance duties to start and will later participate in data entry. Erika and Matthew will both be responsible for manual clerical duties which are vital to the operations of Physicians 1st Billing and Claims.
| Personnel Plan | |||
| Year 1 | Year 2 | Year 3 | |
| Mary | $21,000 | $26,000 | $30,000 |
| John | $21,000 | $26,000 | $30,000 |
| Matthew and Erika | $6,000 | $10,000 | $10,000 |
| Total People | 4 | 4 | 4 |
| Total Payroll | $48,000 | $62,000 | $70,000 |
Financial Plan investor-ready personnel plan .">
The business will be financed mainly through cash flow. With a service oriented business our main investment is for initial software and computer equipment. During subsequent years, other than normal overhead, we will be looking at:
- Advertising fees of $50.00 monthly to Claim Systems advertising pool.
- Renewal of memberships to local and national organizations.
- Updates of reference manuals and books.
- Office supplies and utilities.
- Payroll and benefits.
7.1 Important Assumptions
This financial plan depends on important assumptions, most of which are shown in the following table.
| General Assumptions | |||
| Year 1 | Year 2 | Year 3 | |
| Plan Month | 1 | 2 | 3 |
| Current Interest Rate | 10.00% | 10.00% | 10.00% |
| Long-term Interest Rate | 10.00% | 10.00% | 10.00% |
| Tax Rate | 19.80% | 20.00% | 20.83% |
| Other | 0 | 0 | 0 |
7.2 Key Financial Indicators
The following shows critical profit variables.

7.3 Projected Profit and Loss
Physicians 1st Billing and Claims will show a loss for the first few months of business operation, but profits will increase with sales volume.

| Pro Forma Profit and Loss | |||
| Year 1 | Year 2 | Year 3 | |
| Sales | $158,700 | $168,000 | $182,000 |
| Direct Cost of Sales | $0 | $0 | $0 |
| Other Costs of Sales | $0 | $0 | $0 |
| Total Cost of Sales | $0 | $0 | $0 |
| Gross Margin | $158,700 | $168,000 | $182,000 |
| Gross Margin % | 100.00% | 100.00% | 100.00% |
| Expenses | |||
| Payroll | $48,000 | $62,000 | $70,000 |
| Marketing/Promotion | $14,730 | $15,672 | $16,614 |
| Depreciation | $0 | $0 | $0 |
| Franchise Fee | $1,596 | $0 | $0 |
| Rent | $1,608 | $700 | $700 |
| Utilities | $876 | $600 | $600 |
| Insurance | $204 | $204 | $204 |
| Payroll Taxes | $0 | $0 | $0 |
| Other | $0 | $0 | $0 |
| Total Operating Expenses | $67,014 | $79,176 | $88,118 |
| Profit Before Interest and Taxes | $91,686 | $88,824 | $93,882 |
| EBITDA | $91,686 | $88,824 | $93,882 |
| Interest Expense | $1,405 | $1,040 | $640 |
| Taxes Incurred | $17,879 | $17,557 | $19,422 |
| Net Profit | $72,402 | $70,227 | $73,820 |
| Net Profit/Sales | 45.62% | 41.80% | 40.56% |
7.4 Break-even Analysis
The break-even analysis shows that Physicians 1st Billing and Claims has a good balance of fixed costs and sufficient sales strength to remain healthy. As with any business, the first few months will show negative financial numbers.

| Break-even Analysis | |
| Monthly Units Break-even | 2,175 |
| Monthly Revenue Break-even | $5,585 |
| Assumptions: | |
| Average Per-Unit Revenue | $2.57 |
| Average Per-Unit Variable Cost | $0.00 |
| Estimated Monthly Fixed Cost | $5,585 |
7.5 Projected Cash Flow
Initially, cash flow will be supported by the personal savings accounts of the head officers of this company, and a four-year loan of $16,000, backed by the owners’ assets.

| Pro Forma Cash Flow | |||
| Year 1 | Year 2 | Year 3 | |
| Cash Received | |||
| Cash from Operations | |||
| Cash Sales | $0 | $0 | $0 |
| Cash from Receivables | $111,467 | $165,232 | $177,833 |
| Subtotal Cash from Operations | $111,467 | $165,232 | $177,833 |
| Additional Cash Received | |||
| Sales Tax, VAT, HST/GST Received | $0 | $0 | $0 |
| New Current Borrowing | $0 | $0 | $0 |
| New Other Liabilities (interest-free) | $0 | $0 | $0 |
| New Long-term Liabilities | $0 | $0 | $0 |
| Sales of Other Current Assets | $0 | $0 | $0 |
| Sales of Long-term Assets | $0 | $0 | $0 |
| New Investment Received | $0 | $0 | $0 |
| Subtotal Cash Received | $111,467 | $165,232 | $177,833 |
| Expenditures | Year 1 | Year 2 | Year 3 |
| Expenditures from Operations | |||
| Cash Spending | $48,000 | $62,000 | $70,000 |
| Bill Payments | $32,289 | $38,842 | $37,982 |
| Subtotal Spent on Operations | $80,289 | $100,842 | $107,982 |
| Additional Cash Spent | |||
| Sales Tax, VAT, HST/GST Paid Out | $0 | $0 | $0 |
| Principal Repayment of Current Borrowing | $3,600 | $4,000 | $4,000 |
| Other Liabilities Principal Repayment | $0 | $0 | $0 |
| Long-term Liabilities Principal Repayment | $0 | $0 | $0 |
| Purchase Other Current Assets | $0 | $0 | $0 |
| Purchase Long-term Assets | $0 | $0 | $0 |
| Dividends | $0 | $0 | $0 |
| Subtotal Cash Spent | $83,889 | $104,842 | $111,982 |
| Net Cash Flow | $27,577 | $60,390 | $65,851 |
| Cash Balance | $43,577 | $103,968 | $169,819 |
7.6 Projected Balance Sheet
The following is the Projected Balance Sheet for the next three years.
| Pro Forma Balance Sheet | |||
| Year 1 | Year 2 | Year 3 | |
| Assets | |||
| Current Assets | |||
| Cash | $43,577 | $103,968 | $169,819 |
| Accounts Receivable | $47,233 | $50,001 | $54,168 |
| Other Current Assets | $0 | $0 | $0 |
| Total Current Assets | $90,811 | $153,969 | $223,987 |
| Long-term Assets | |||
| Long-term Assets | $0 | $0 | $0 |
| Accumulated Depreciation | $0 | $0 | $0 |
| Total Long-term Assets | $0 | $0 | $0 |
| Total Assets | $90,811 | $153,969 | $223,987 |
| Liabilities and Capital | Year 1 | Year 2 | Year 3 |
| Current Liabilities | |||
| Accounts Payable | $6,009 | $2,940 | $3,138 |
| Current Borrowing | $12,400 | $8,400 | $4,400 |
| Other Current Liabilities | $0 | $0 | $0 |
| Subtotal Current Liabilities | $18,409 | $11,340 | $7,538 |
| Long-term Liabilities | $0 | $0 | $0 |
| Total Liabilities | $18,409 | $11,340 | $7,538 |
| Paid-in Capital | $9,604 | $9,604 | $9,604 |
| Retained Earnings | ($9,604) | $62,798 | $133,025 |
| Earnings | $72,402 | $70,227 | $73,820 |
| Total Capital | $72,402 | $142,629 | $216,448 |
| Total Liabilities and Capital | $90,811 | $153,969 | $223,987 |
| Net Worth | $72,402 | $142,629 | $216,448 |
7.7 Business Ratios
Business ratios for the years of this plan are shown below. Industry profile ratios based on the Standard Industrial Classification (SIC) code 6411, Insurance Agents, Brokers, and Service, are shown for comparison.
| Ratio Analysis | ||||
| Year 1 | Year 2 | Year 3 | Industry Profile | |
| Sales Growth | 0.00% | 5.86% | 8.33% | 2.40% |
| Percent of Total Assets | ||||
| Accounts Receivable | 52.01% | 32.47% | 24.18% | 26.30% |
| Other Current Assets | 0.00% | 0.00% | 0.00% | 64.30% |
| Total Current Assets | 100.00% | 100.00% | 100.00% | 90.60% |
| Long-term Assets | 0.00% | 0.00% | 0.00% | 9.40% |
| Total Assets | 100.00% | 100.00% | 100.00% | 100.00% |
| Current Liabilities | 20.27% | 7.37% | 3.37% | 48.20% |
| Long-term Liabilities | 0.00% | 0.00% | 0.00% | 9.50% |
| Total Liabilities | 20.27% | 7.37% | 3.37% | 57.70% |
| Net Worth | 79.73% | 92.63% | 96.63% | 42.30% |
| Percent of Sales | ||||
| Sales | 100.00% | 100.00% | 100.00% | 100.00% |
| Gross Margin | 100.00% | 100.00% | 100.00% | 100.00% |
| Selling, General & Administrative Expenses | 54.38% | 58.20% | 59.44% | 60.10% |
| Advertising Expenses | 0.00% | 0.00% | 0.00% | 1.70% |
| Profit Before Interest and Taxes | 57.77% | 52.87% | 51.58% | 5.20% |
| Main Ratios | ||||
| Current | 4.93 | 13.58 | 29.71 | 1.66 |
| Quick | 4.93 | 13.58 | 29.71 | 1.45 |
| Total Debt to Total Assets | 20.27% | 7.37% | 3.37% | 57.70% |
| Pre-tax Return on Net Worth | 124.69% | 61.55% | 43.08% | 5.80% |
| Pre-tax Return on Assets | 99.42% | 57.01% | 41.63% | 13.70% |
| Additional Ratios | Year 1 | Year 2 | Year 3 | |
| Net Profit Margin | 45.62% | 41.80% | 40.56% | n.a |
| Return on Equity | 100.00% | 49.24% | 34.10% | n.a |
| Activity Ratios | ||||
| Accounts Receivable Turnover | 3.36 | 3.36 | 3.36 | n.a |
| Collection Days | 55 | 106 | 104 | n.a |
| Accounts Payable Turnover | 6.37 | 12.17 | 12.17 | n.a |
| Payment Days | 27 | 46 | 29 | n.a |
| Total Asset Turnover | 1.75 | 1.09 | 0.81 | n.a |
| Debt Ratios | ||||
| Debt to Net Worth | 0.25 | 0.08 | 0.03 | n.a |
| Current Liab. to Liab. | 1.00 | 1.00 | 1.00 | n.a |
| Liquidity Ratios | ||||
| Net Working Capital | $72,402 | $142,629 | $216,448 | n.a |
| Interest Coverage | 65.26 | 85.41 | 146.69 | n.a |
| Additional Ratios | ||||
| Assets to Sales | 0.57 | 0.92 | 1.23 | n.a |
| Current Debt/Total Assets | 20% | 7% | 3% | n.a |
| Acid Test | 2.37 | 9.17 | 22.53 | n.a |
| Sales/Net Worth | 2.19 | 1.18 | 0.84 | n.a |
| Dividend Payout | 0.00 | 0.00 | 0.00 | n.a |
| Sales Forecast | |||||||||||||
| Month 1 | Month 2 | Month 3 | Month 4 | Month 5 | Month 6 | Month 7 | Month 8 | Month 9 | Month 10 | Month 11 | Month 12 | ||
| Unit Sales | |||||||||||||
| Service 1 | 0% | 400 | 800 | 1,200 | 1,800 | 2,200 | 2,600 | 3,000 | 3,400 | 3,800 | 4,200 | 4,600 | 5,000 |
| Service 2 | 0% | 0 | 0 | 0 | 0 | 2,200 | 2,600 | 3,000 | 3,400 | 3,800 | 4,200 | 4,600 | 5,000 |
| Total Unit Sales | 400 | 800 | 1,200 | 1,800 | 4,400 | 5,200 | 6,000 | 6,800 | 7,600 | 8,400 | 9,200 | 10,000 | |
| Unit Prices | Month 1 | Month 2 | Month 3 | Month 4 | Month 5 | Month 6 | Month 7 | Month 8 | Month 9 | Month 10 | Month 11 | Month 12 | |
| Service 1 | $3.50 | $3.50 | $3.50 | $3.50 | $3.50 | $3.50 | $3.50 | $3.50 | $3.50 | $3.50 | $3.50 | $3.50 | |
| Service 2 | $1.50 | $1.50 | $1.50 | $1.50 | $1.50 | $1.50 | $1.50 | $1.50 | $1.50 | $1.50 | $1.50 | $1.50 | |
| Sales | |||||||||||||
| Service 1 | $1,400 | $2,800 | $4,200 | $6,300 | $7,700 | $9,100 | $10,500 | $11,900 | $13,300 | $14,700 | $16,100 | $17,500 | |
| Service 2 | $0 | $0 | $0 | $0 | $3,300 | $3,900 | $4,500 | $5,100 | $5,700 | $6,300 | $6,900 | $7,500 | |
| Total Sales | $1,400 | $2,800 | $4,200 | $6,300 | $11,000 | $13,000 | $15,000 | $17,000 | $19,000 | $21,000 | $23,000 | $25,000 | |
| Direct Unit Costs | Month 1 | Month 2 | Month 3 | Month 4 | Month 5 | Month 6 | Month 7 | Month 8 | Month 9 | Month 10 | Month 11 | Month 12 | |
| Service 1 | 0.00% | $0.00 | $0.00 | $0.00 | $0.00 | $0.00 | $0.00 | $0.00 | $0.00 | $0.00 | $0.00 | $0.00 | $0.00 |
| Service 2 | 0.00% | $0.00 | $0.00 | $0.00 | $0.00 | $0.00 | $0.00 | $0.00 | $0.00 | $0.00 | $0.00 | $0.00 | $0.00 |
| Direct Cost of Sales | |||||||||||||
| Service 1 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | |
| Service 2 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | |
| Subtotal Direct Cost of Sales | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | |
| Personnel Plan | |||||||||||||
| Month 1 | Month 2 | Month 3 | Month 4 | Month 5 | Month 6 | Month 7 | Month 8 | Month 9 | Month 10 | Month 11 | Month 12 | ||
| Mary | 0% | $1,000 | $1,000 | $1,000 | $2,000 | $2,000 | $2,000 | $2,000 | $2,000 | $2,000 | $2,000 | $2,000 | $2,000 |
| John | 0% | $1,000 | $1,000 | $1,000 | $2,000 | $2,000 | $2,000 | $2,000 | $2,000 | $2,000 | $2,000 | $2,000 | $2,000 |
| Matthew and Erika | 0% | $400 | $400 | $400 | $400 | $400 | $400 | $600 | $600 | $600 | $600 | $600 | $600 |
| Total People | 4 | 4 | 4 | 4 | 4 | 4 | 4 | 4 | 4 | 4 | 4 | 4 | |
| Total Payroll | $2,400 | $2,400 | $2,400 | $4,400 | $4,400 | $4,400 | $4,600 | $4,600 | $4,600 | $4,600 | $4,600 | $4,600 | |
| Pro Forma Profit and Loss | |||||||||||||
| Month 1 | Month 2 | Month 3 | Month 4 | Month 5 | Month 6 | Month 7 | Month 8 | Month 9 | Month 10 | Month 11 | Month 12 | ||
| Sales | $1,400 | $2,800 | $4,200 | $6,300 | $11,000 | $13,000 | $15,000 | $17,000 | $19,000 | $21,000 | $23,000 | $25,000 | |
| Direct Cost of Sales | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | |
| Other Costs of Sales | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | |
| Total Cost of Sales | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | |
| Gross Margin | $1,400 | $2,800 | $4,200 | $6,300 | $11,000 | $13,000 | $15,000 | $17,000 | $19,000 | $21,000 | $23,000 | $25,000 | |
| Gross Margin % | 100.00% | 100.00% | 100.00% | 100.00% | 100.00% | 100.00% | 100.00% | 100.00% | 100.00% | 100.00% | 100.00% | 100.00% | |
| Expenses | |||||||||||||
| Payroll | $2,400 | $2,400 | $2,400 | $4,400 | $4,400 | $4,400 | $4,600 | $4,600 | $4,600 | $4,600 | $4,600 | $4,600 | |
| Marketing/Promotion | $280 | $410 | $630 | $770 | $950 | $1,130 | $1,310 | $1,490 | $1,670 | $1,850 | $2,030 | $2,210 | |
| Depreciation | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | |
| Franchise Fee | $133 | $133 | $133 | $133 | $133 | $133 | $133 | $133 | $133 | $133 | $133 | $133 | |
| Rent | $134 | $134 | $134 | $134 | $134 | $134 | $134 | $134 | $134 | $134 | $134 | $134 | |
| Utilities | $73 | $73 | $73 | $73 | $73 | $73 | $73 | $73 | $73 | $73 | $73 | $73 | |
| Insurance | $17 | $17 | $17 | $17 | $17 | $17 | $17 | $17 | $17 | $17 | $17 | $17 | |
| Payroll Taxes | 15% | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 |
| Other | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | |
| Total Operating Expenses | $3,037 | $3,167 | $3,387 | $5,527 | $5,707 | $5,887 | $6,267 | $6,447 | $6,627 | $6,807 | $6,987 | $7,167 | |
| Profit Before Interest and Taxes | ($1,637) | ($367) | $813 | $773 | $5,293 | $7,113 | $8,733 | $10,553 | $12,373 | $14,193 | $16,013 | $17,833 | |
| EBITDA | ($1,637) | ($367) | $813 | $773 | $5,293 | $7,113 | $8,733 | $10,553 | $12,373 | $14,193 | $16,013 | $17,833 | |
| Interest Expense | $131 | $128 | $126 | $123 | $121 | $118 | $116 | $113 | $111 | $108 | $106 | $103 | |
| Taxes Incurred | ($530) | ($99) | $137 | $130 | $1,034 | $1,399 | $1,723 | $2,088 | $2,452 | $2,817 | $3,181 | $3,546 | |
| Net Profit | ($1,237) | ($396) | $550 | $520 | $4,138 | $5,596 | $6,894 | $8,352 | $9,810 | $11,268 | $12,726 | $14,184 | |
| Net Profit/Sales | -88.39% | -14.15% | 13.09% | 8.25% | 37.62% | 43.04% | 45.96% | 49.13% | 51.63% | 53.66% | 55.33% | 56.73% | |
| Pro Forma Cash Flow | |||||||||||||
| Month 1 | Month 2 | Month 3 | Month 4 | Month 5 | Month 6 | Month 7 | Month 8 | Month 9 | Month 10 | Month 11 | Month 12 | ||
| Cash Received | |||||||||||||
| Cash from Operations | |||||||||||||
| Cash Sales | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | |
| Cash from Receivables | $0 | $47 | $1,447 | $2,847 | $4,270 | $6,457 | $11,067 | $13,067 | $15,067 | $17,067 | $19,067 | $21,067 | |
| Subtotal Cash from Operations | $0 | $47 | $1,447 | $2,847 | $4,270 | $6,457 | $11,067 | $13,067 | $15,067 | $17,067 | $19,067 | $21,067 | |
| Additional Cash Received | |||||||||||||
| Sales Tax, VAT, HST/GST Received | 0.00% | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 |
| New Current Borrowing | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | |
| New Other Liabilities (interest-free) | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | |
| New Long-term Liabilities | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | |
| Sales of Other Current Assets | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | |
| Sales of Long-term Assets | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | |
| New Investment Received | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | |
| Subtotal Cash Received | $0 | $47 | $1,447 | $2,847 | $4,270 | $6,457 | $11,067 | $13,067 | $15,067 | $17,067 | $19,067 | $21,067 | |
| Expenditures | Month 1 | Month 2 | Month 3 | Month 4 | Month 5 | Month 6 | Month 7 | Month 8 | Month 9 | Month 10 | Month 11 | Month 12 | |
| Expenditures from Operations | |||||||||||||
| Cash Spending | $2,400 | $2,400 | $2,400 | $4,400 | $4,400 | $4,400 | $4,600 | $4,600 | $4,600 | $4,600 | $4,600 | $4,600 | |
| Bill Payments | $8 | $256 | $811 | $1,255 | $1,416 | $2,480 | $3,021 | $3,524 | $4,066 | $4,608 | $5,150 | $5,692 | |
| Subtotal Spent on Operations | $2,408 | $2,656 | $3,211 | $5,655 | $5,816 | $6,880 | $7,621 | $8,124 | $8,666 | $9,208 | $9,750 | $10,292 | |
| Additional Cash Spent | |||||||||||||
| Sales Tax, VAT, HST/GST Paid Out | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | |
| Principal Repayment of Current Borrowing | $300 | $300 | $300 | $300 | $300 | $300 | $300 | $300 | $300 | $300 | $300 | $300 | |
| Other Liabilities Principal Repayment | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | |
| Long-term Liabilities Principal Repayment | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | |
| Purchase Other Current Assets | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | |
| Purchase Long-term Assets | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | |
| Dividends | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | |
| Subtotal Cash Spent | $2,708 | $2,956 | $3,511 | $5,955 | $6,116 | $7,180 | $7,921 | $8,424 | $8,966 | $9,508 | $10,050 | $10,592 | |
| Net Cash Flow | ($2,708) | ($2,909) | ($2,065) | ($3,108) | ($1,846) | ($724) | $3,146 | $4,642 | $6,100 | $7,558 | $9,016 | $10,474 | |
| Cash Balance | $13,292 | $10,383 | $8,318 | $5,210 | $3,364 | $2,640 | $5,786 | $10,428 | $16,528 | $24,087 | $33,103 | $43,577 | |
| Pro Forma Balance Sheet | |||||||||||||
| Month 1 | Month 2 | Month 3 | Month 4 | Month 5 | Month 6 | Month 7 | Month 8 | Month 9 | Month 10 | Month 11 | Month 12 | ||
| Assets | Starting Balances | ||||||||||||
| Current Assets | |||||||||||||
| Cash | $16,000 | $13,292 | $10,383 | $8,318 | $5,210 | $3,364 | $2,640 | $5,786 | $10,428 | $16,528 | $24,087 | $33,103 | $43,577 |
| Accounts Receivable | $0 | $1,400 | $4,153 | $6,907 | $10,360 | $17,090 | $23,633 | $27,567 | $31,500 | $35,433 | $39,367 | $43,300 | $47,233 |
| Other Current Assets | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 |
| Total Current Assets | $16,000 | $14,692 | $14,536 | $15,225 | $15,570 | $20,454 | $26,273 | $33,352 | $41,928 | $51,962 | $63,453 | $76,403 | $90,811 |
| Long-term Assets | |||||||||||||
| Long-term Assets | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 |
| Accumulated Depreciation | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 |
| Total Long-term Assets | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 |
| Total Assets | $16,000 | $14,692 | $14,536 | $15,225 | $15,570 | $20,454 | $26,273 | $33,352 | $41,928 | $51,962 | $63,453 | $76,403 | $90,811 |
| Liabilities and Capital | Month 1 | Month 2 | Month 3 | Month 4 | Month 5 | Month 6 | Month 7 | Month 8 | Month 9 | Month 10 | Month 11 | Month 12 | |
| Current Liabilities | |||||||||||||
| Accounts Payable | $0 | $230 | $770 | $1,209 | $1,334 | $2,380 | $2,904 | $3,389 | $3,913 | $4,437 | $4,961 | $5,485 | $6,009 |
| Current Borrowing | $16,000 | $15,700 | $15,400 | $15,100 | $14,800 | $14,500 | $14,200 | $13,900 | $13,600 | $13,300 | $13,000 | $12,700 | $12,400 |
| Other Current Liabilities | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 |
| Subtotal Current Liabilities | $16,000 | $15,930 | $16,170 | $16,309 | $16,134 | $16,880 | $17,104 | $17,289 | $17,513 | $17,737 | $17,961 | $18,185 | $18,409 |
| Long-term Liabilities | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 | $0 |
| Total Liabilities | $16,000 | $15,930 | $16,170 | $16,309 | $16,134 | $16,880 | $17,104 | $17,289 | $17,513 | $17,737 | $17,961 | $18,185 | $18,409 |
| Paid-in Capital | $9,604 | $9,604 | $9,604 | $9,604 | $9,604 | $9,604 | $9,604 | $9,604 | $9,604 | $9,604 | $9,604 | $9,604 | $9,604 |
| Retained Earnings | ($9,604) | ($9,604) | ($9,604) | ($9,604) | ($9,604) | ($9,604) | ($9,604) | ($9,604) | ($9,604) | ($9,604) | ($9,604) | ($9,604) | ($9,604) |
| Earnings | $0 | ($1,237) | ($1,634) | ($1,084) | ($564) | $3,573 | $9,169 | $16,063 | $24,415 | $34,224 | $45,492 | $58,218 | $72,402 |
| Total Capital | $0 | ($1,237) | ($1,634) | ($1,084) | ($564) | $3,573 | $9,169 | $16,063 | $24,415 | $34,224 | $45,492 | $58,218 | $72,402 |
| Total Liabilities and Capital | $16,000 | $14,692 | $14,536 | $15,225 | $15,570 | $20,454 | $26,273 | $33,352 | $41,928 | $51,962 | $63,453 | $76,403 | $90,811 |
| Net Worth | $0 | ($1,237) | ($1,634) | ($1,084) | ($564) | $3,573 | $9,169 | $16,063 | $24,415 | $34,224 | $45,492 | $58,218 | $72,402 |
The quickest way to turn a business idea into a business plan
Fill-in-the-blanks and automatic financials make it easy.
No thanks, I prefer writing 40-page documents.

Discover the world’s #1 plan building software

- Our approach
Scott Young, MD
Co-Executive Director and Senior Medical Director of CMI
Scott Young, MD, serves as associate executive director for Clinical Care and Innovation at The Permanente Federation. He also serves as the Executive Director and Senior Medical Director of Kaiser Permanente’s Care Management Institute. He leads a nationwide team that is integral to Kaiser Permanente’s commitment to improve the care and wellness of its 9.3 million members. His work includes commissioning the discovery, development and spread of programs and best practices focused on care delivery, education and member experience.
Dr. Young is former director for Health IT at the Agency for Healthcare Research and Quality. Prior to joining that agency, he served as a senior clinical advisor at the Centers for Medicare and Medicaid Services. Dr. Young’s policy experience also includes service as a Robert Wood Johnson health policy fellow in the office of U.S. Sen. Jeff Bingaman of New Mexico.
He is former executive vice president of the Utah HealthCare Institute, a not-for-profit organization providing clinical care, outreach programs, medical education, research, informatics and health policy services. Dr. Young is a founding member of Intermountain Health Care’s Utah Valley Family Practice Residency.
Dr. Young received his medical degree from the University of Oklahoma in 1987 and completed his training at the Fairfax Family Practice Residency. He is board certified in family medicine and a fellow of the American Academy of Family Physicians.
Joan Gelrud, RN, MSN, CPHQ, FACHE
Senior Vice President of National Health Plan and Hospital Quality and the Co-executive Director of CMI
Joan Gelrud leads work to advance Kaiser Permanente’s nation-leading excellence in quality, safety and experience. She oversees Care Experience, Risk and Patient Safety, the Design Consultancy, Quality Governance, Accreditation, Licensing and Regulation, and the Performance Institute. As the Co-Executive Director of the Care Management Institute, Joan, with her partner Scott Young, MD oversee the award-winning work of the interdisciplinary CMI team for Kaiser Permanente.
Joan joined Kaiser Permanente in September of 2015. In her position as Vice President of Quality, Regulatory and Risk Management for Mid-Atlantic States, Joan provided strategic leadership for Kaiser Permanente to compete as a quality leader in health care. She had responsibility for the quality and safety of care, treatment and services provided to members, including outcomes and accreditation, licensing, clinical risk management, peer review and credentialing. Joan was responsible for leveraging best practices across the region and served as the Chief Nurse Executive. Joan was also responsible for Infection Prevention, Employee Health, Regional Patient Care Services, Clinical Staff Education, Outreach to members and communities via mobile van services. Under the safety umbrella, Joan was responsible for patient and workforce safety across the region. She completed Kaiser Permanente’s Executive Leadership Program at Harvard University while in Mid-Atlantic States.
Prior to joining Kaiser Permanente, Joan was Vice President at MedStar St. Mary’s Hospital in Leonardtown, Maryland where responsibilities included Quality, Safety, Data and Analytics, Clinical Resource Management, Stroke Center, Organizational Learning and Research, Community Health Outreach, Human Resources, Imaging, Risk Management, Cardiology, Neurology, Respiratory Therapy, Rehabilitation Services, Patient Advocates, Pharmacy and Laboratory. Some of Joan’s operational accomplishments included opening practices to improve access to pediatric neurology, cardiology and pulmonary outpatient services, working with Children’s National Medical Center and MedStar Georgetown University Hospital. She expanded local interventional radiology and tele-neurology services with the MedStar Washington Hospital Center and MedStar Georgetown University Hospital. Her team achieved a Health Enterprise Zone designation in St. Mary’s County and a competitive state grant to improve access to healthcare, reduce readmissions and address social barriers to health.
Jim Bellows, PhD
Managing Director
Jim Bellows leads CMI’s research and development work, which includes supporting care delivery innovation projects, identifying specific population care practices that contribute to superior performance, and supporting and studying the spread of the most promising practices.
He is also responsible for CMI’s efforts in demonstrating the value of population care and consults with a variety of Program Office leaders and departments on areas related to program evaluation and performance measurement.
Dr. Bellows has been a lecturer at the University of California Berkeley School of Public Health, where he taught Health Care Quality – Measurement and Improvement from 2004 to 2007. He earned his PhD in health services research and health economics from the University of California Berkeley and joined CMI in July 2001 after several earlier careers. He received a master’s degree in public health from University of California Berkeley and a bachelor’s degree from the University of California Santa Cruz.
Maria A. Butler
Director of Business Operations
Maria Butler is the Director of Business Operations at Kaiser Permanente’s Care Management Institute. Maria joined CMI in 2006 and oversees the business function of the department; managing finance activities, human resources and administrative operations that support the department’s ability to achieve its business objectives. This management function works closely with the CMI Executive Directors, leadership, managers, and staff to ensure the smooth running of the organization by carrying out the department’s plan, anticipating risk, and solving problems creatively and effectively. Maria has a BA degree from San Francisco State University and over twenty years of experience in finance and administration having worked at APL Global Logistics, Crowley Maritime Corporation, Peet’s Coffee & Tea, and Saatchi & Saatchi Corporate Communications.
Tracy Cameron
Senior Director
Tracy Cameron leads the Care Management Institute’s work in Care Experience. In this role, she partners with regional and national leaders to improve access to care and provide our members with an excellent care experience across settings. She previously served as Director of Performance Assessment for The Permanente Federation and Director of Medical Economics in Kaiser Permanente’s Northern California region.
Prior to joining Kaiser Permanente in 1987, Tracy was a research scientist at Pacific Presbyterian Medical Center and the University of California at Berkeley, where she worked in public health research.
Tracy holds a bachelor’s degree in Sociology from Purdue University, as well as a master’s degree in Sociology and an MBA from the University of California, Berkeley.
Carol Cain, PhD
Senior Director, Clinical Information Services
Carol Cain, PhD, directs the Care Management Institute’s Clinical Information Services, including Kaiser Permanente’s Clinical Library, guideline and evidence services, and care delivery informatics. She co-leads the Permanente Federation’s Clinical Education portfolio, including national Continuing Medical Education activities and conferences, and quality improvement for Maintenance of Certification. She also coordinates the Care Management Institute’s partner relations with organizations outside Kaiser Permanente.
Carol has worked on care delivery improvement in several clinical pathways, including the transition from hospital to home, reducing hospital infections, managing chronic pain, and others, with the goal of expanding physician capacity in guiding clinical improvement projects, sharing pathways across Kaiser Permanente, and looking at ongoing reliability and quality in those pathways. She has also worked on design of the transition from hospital to home from a patient and caregiver perspective; spread of successful innovations; and care delivery implications of technology. She has a background in clinical informatics from Stanford and is currently teaching a biomedical informatics graduate course on designing IT innovations. She previously managed the health IT portfolio at AHRQ, the Agency for Healthcare Research and Quality.
Jeff Convissar, MD
Medical Director
Jeff Convissar, MD is the Medical Director at Kaiser Permanente’s Care Management Institute. He has been with Kaiser Permanente since 1992. Jeff was previously the Executive Director of National Risk Management. Prior to that, for 12 years he was an attending physician in the Emergency Department at the Kaiser Permanente Santa Clara Medical Center in Northern California. At Santa Clara, Jeff also served as the Assistant Chief of Quality. Jeff has a BA in Biology from Brown University, his MD is from the UCLA School of Medicine and ED residency training was completed at Harbor-UCLA Medical Center. Jeff is responsible for a variety of improvement initiatives at Kaiser Permanente.
Rivka Gordon, PA, MHS
Chief of Staff
Rivka Gordon is Chief of Staff to the Associate Executive Director of the Care Management Institute and is a member of the leadership team. Rivka is a Primary Care Physician Assistant with a Masters degree in Health Sciences from Duke University. In addition to her work at Kaiser Permanente, Rivka serves on Planned Parenthood Federation of America’s National Medical Committee and on the San Francisco Women’s Community Clinic and Tara Health Foundation boards of directors.
Craig W Robbins, MD, MPH
Medical Director, Clinical Information Services
Dr. Craig Robbins serves as Medical Director of the Center for Clinical Information Services in the KP Care Management Institute. He also serves as Medical Director for the KP Maintenance of Certification Portfolio at The Permanente Federation. He has been a family physician with the Colorado Permanente Medical Group since July 1998. In his CMI role, Dr. Robbins is the lead physician for the KP National Guidelines Program which has been an organizational member of the Guidelines International Network (G-I-N) since 2010. He is a current member of the G-I-N Board of Trustees, the Executive Advisory Board for the Kaiser Permanente Research Associates Evidence-based Practice Center (KPRA-EPC), and the Editorial Board for the National Guideline and Quality Metric Clearinghouses (NGC/NQMC). Dr. Robbins received his BS (1990) and MD (1993) from the University of Michigan and his MPH (1998) from the University of Pittsburgh. He completed his Family Medicine Residency (1993-6) at the University of Virginia and a Faculty Development Fellowship (1996-8) at the University of Pittsburgh Medical Center-St Margaret Hospital in Pittsburgh, PA.
Lisa Schilling, RN, MPH
Vice President
Lisa Schilling, RN, MPH, is national Vice President, Healthcare Performance Improvement and Director of Kaiser Permanente’s Center for Health System Performance. She leads the strategy to develop and implement a performance improvement system and planning to adopt its total health strategy in care delivery.
A leader with more than 20 years’ experience, Lisa serves on the editorial board of the Joint Commission Journal for Quality and Safety and has authored several publications on related topics.
Prior to Kaiser Permanente, she was the national director of critical care services at VHA Inc., focusing on improving delivery system performance.
Matthew C. Stiefel
Matt Stiefel directs Population Health in Kaiser Permanente’s Care Management Institute. He was a 2008-09 fellow with the Institute for Healthcare Improvement, and continues as a faculty member for the IHI Triple Aim. Matt joined Kaiser Permanente in 1981 as a medical economist, and later held management positions in Kaiser Permanente Northwest, directing planning, marketing, and medical economics. He joined the Care Management Institute in 1998. Prior to Kaiser Permanente, he served as a policy analyst on the Carter Administration Domestic Policy Staff and in the US Department of Health, Education and Welfare, and as a local health planner in the San Francisco bay area. He completed an MS in epidemiology from the Harvard School of Public Health in 2013, holds an MPA from the Wharton School, and a BA in psychology from Stanford.
Winston Wong, MD
Dr. Wong serves as Medical Director, Community Benefit, National Program Office, and is responsible for developing partnerships with communities and organizations in advancing population management and evidence based medicine, with a particular focus on health disparities and vulnerable populations. Previous to Kaiser Permanente, Dr. Wong served as a Captain in the U.S. Public Health Service and was awarded an Outstanding Service Medal. In addition to playing various advisory roles with CMMS, NIH and the National Academy of Medicine, and most recently to DHHS as an advisor on minority health, Wong currently serves on Boards representing public hospitals and school based health centers addressing issues of access and quality for diverse populations. He is also a Board member of the California Endowment, one of the nation’s largest health philanthropies. Bilingual in Cantonese and Toisan dialects, Dr. Wong continues a small practice in Family Medicine at Asian Health Services in Oakland, a federally qualified health center, where he previously served as Medical Director. Dr. Wong was featured as a “Face of Public Health” in the American Journal of Public Health. Dr. Wong received his undergraduate and Master’s degrees at UC Berkeley, his medical degree from UC San Francisco, and an Honorary Doctorate in Humane Letters from the A.T. Still School of Osteopathy.
- Terms & Conditions
- Privacy Practices
- Site policies
- Quick Facts
- Evaluation/Analytics
- Evidence Services
- Patient-Centered Improvement
- Breastfeeding Support
- Cardiovascular Health
- Spreading Effective Practices
- Publications

IMAGES
VIDEO
COMMENTS
10 Steps to Starting a Healthcare Consulting Business. 1. Conduct Market Research To Determine Demand. An important step to starting a healthcare consulting business is conducting market research. To begin, you must learn what services your clients want and how much they are willing to pay for them.
Starting your healthcare consulting business. Starting a healthcare consulting business requires careful planning and preparation. Here are the key steps to get your healthcare consulting business off the ground. Creating a business plan. A business plan outlines your business goals, target audience, marketing strategies, and financial projections.
Biotechnology Reagents. Prepared the business plan and financial model for a division of a billion-dollar public biotechnology company. The business makes instruments, consumables, and software for scientists engaged in medical research, drug discovery, agricultural research, biosecurity, and quality and safety testing.
The McKinsey Health Institute (MHI) is an enduring, non-profit-generating entity within the firm. It was founded on the conviction that, over the next decade, humanity could add as much as 45 billion extra years of higher-quality life (roughly 6 years per person on average—and substantially more in some countries and populations). Learn more.
You need a relevant bachelor's degree to begin working as a healthcare consultant. 1. Earn a bachelor's degree. To ensure your bachelor's degree is relevant to your desired position in healthcare consulting, choose a field of study related to the industry, such as public health, business, or even nursing.
With your expertise and experience in the field, you can start building a thriving online medical consultation business. Now, let's look into the steps to building a successful healthcare consulting business. 1. Crafting a Healthcare consulting business plan. Preparing a healthcare consulting business plan involves creating a document that ...
18 Steps to Starting a Healthcare Consulting Business 1. Understand the Industry. Players in the healthcare consulting services industry provide specialist advice to businesses involved in healthcare fields such as hospitals, physicians, pharmaceutical companies, healthcare related organizations, health management organizations and healthcare insurance providers et al.
The global healthcare market is one of the largest and highest-valued industries in the world. According to Global Newswire, the global healthcare services market is currently valued at $7548.52 billion and is expected to reach $10414.36 billion in 2026. This growth is expected to continue for the foreseeable future.
Below you will find an extensive array of business plan examples for a variety of medical and healthcare businesses, including private clinics, medical device startups, telemedicine services, and healthcare consulting firms. Each plan is meticulously crafted to address crucial aspects such as market research, compliance with healthcare ...
Top leader Healthcare Provider digital services Everest. Accenture scored higher than all competitors in both Market Impact and Vision & Capability for its ability to drive digital transformation across the healthcare provider value chain, including patient engagement, care management, financials and network management. Learn more.
Medical Practice Business Plan. Over the past 20+ years, we have helped over 500 entrepreneurs and business owners create business plans to start a new practice and grow their medical private practices. On this page, we will first give you some background information with regards to the importance of business planning.
Veterinary Practice Business Plans. Looking for a free sample business plan for a medical billing, chiropractic, dental, hospital, or another health care businesses? You've come to the right place! Explore our library of Medical & Health Business Plan Templates and find inspiration for your own business.
Create your online presence. 5. Deliver quality work. 6. Keep learning and improving. Be the first to add your personal experience. 7. Here's what else to consider. Be the first to add your ...
Traditionally, a marketing plan includes the four P's: Product, Price, Place, and Promotion. For a medical device business plan, your marketing strategy should include the following: Product: In the product section, you should reiterate the type of medical device company that you documented in your company overview.
Here are the key steps to consider when writing a business plan: 1. Executive Summary. An executive summary is the first section planned to offer an overview of the entire business plan. However, it is written after the entire business plan is ready and summarizes each section of your plan.
Discover Upmetrics' library of 400+ business plan examples to help you write your business plan. Upmetrics is a modern and intuitive business plan app that streamlines business planning with its free templates and AI-powered features. So what are you waiting for? Download your example and draft a perfect business plan.
Explore a real-world medical services management business plan example and download a free template with this information to start writing your own business plan. ... Consultants: $14,000 : Insurance: $1,000 : Rent: $2,000 : Research and development: $40,000 : Expensed equipment: $20,000 : Other: $4,000 : Total Start-up Expenses:
University, Beijing, ESADE Business School, Barcelona, IE Business School, Madrid, Pas-teur Institute, Paris, as well as in Argentina, Chile, Mexico, Vietnam and Morocco. "Our company just won a regional business plan competition. A big thanks to our advisors, including Stephanie Marrus and the UCSF Startup 101 team, for helping us prepare."
Position your practice's business opportunity. Now that you're familiar with what's included in your executive summary, tuck that information away, and get to work on the rest of your plan. Think of the next few sections of your plan as the overarching description of your practice's business opportunity.
A business plan consultant works closely with you and understands your business thoroughly. They help you achieve your goals like expanded market share, cost reduction, enhanced customer experience, and more. Consultants have experience in various industries and expertise in fields like marketing, strategic planning, and more. So, having a ...
Founded in 2002, Zinnov is a global management and strategy consulting firm, with presence in Silicon Valley, Houston, Bangalore, and Gurgaon. Over the past 16 years, Zinnov has successfully consulted [... view the full profile of Zinnov] Santa Clara, California. 250 - 499 $100/hr Inquire.
The price of this package includes: state of the art medical billing and accounting software, unlimited training for the first six months, two years of 24-hour technical support, emergency support service, and a full-featured marketing package. The price of the package is $5,000.00 plus $45.00 for shipping and handling.
Joan Gelrud leads work to advance Kaiser Permanente's nation-leading excellence in quality, safety and experience. She oversees Care Experience, Risk and Patient Safety, the Design Consultancy, Quality Governance, Accreditation, Licensing and Regulation, and the Performance Institute. As the Co-Executive Director of the Care Management ...
Provider Gender. Go public. Find a Santa Clara Valley Medical Center (SCVMC) provider near you in San Jose, Bascom, East Valley, Gilroy, Milpitas, Moorpark, Sunnyvale and Tully. Search for care teams across a range of specialties, including family medicine, internal medicine, radiology, surgery, and more.