Nursing Management: Guide to Organizing, Staffing, Scheduling, Directing & Delegation

This is a guide for nurses who wants to learn the concepts behind Nursing Management. This will guide you to Organizing, Staffing, Scheduling, Directing & Delegation for nursing.

Table of Contents
Organizing process includes, three forms of authority, organizational chart, organizational structure, managerial levels, patterns of organizational structure, types of organizational structure, staffing process.
- Two Ways of Developing a Staffing Pattern
Considerations in Staffing Pattern
Patient classification system, patient care is classified according to:, elements of directing, barriers in communication, good reasons for delegation, managers who do not delegate, common errors in delegation, steps in effective delegating, conflict management, two main types, conflict resolution strategies.
- Determine what task are to be done, who is to do these, how the tasks are to be grouped, who reports to whom and what decisions are to be made.
- It is a form of identifying roles and relationships of each staff on order to delineate specific tasks or functions that will carry out organizational plan s and objectives.
- Process of identifying and grouping the work to be performed, defining and delegating responsibility and authority and establishing relationships for the purpose of enabling the people to work more effectively together in accomplishing objectives.
- As a process, it refers to the building of a structure that will provide for the separation of activities to be performed and for the arrangement of these activities in a framework which indicates their hierarchal importance and functional association.
- Identifying and defining basic tasks.
- Delegation of authority and assigning responsibility
- Establishing relationships
- Chain of Command – unbroken line of reporting relationships that extends through the entire organization. The line defines the chain of command and the formal decision making structure.
- Unity of Command – within the chin states that, each person in the organization should take orders and reports only to one person.
- Span of Control – refers to the number of employees that should be placed under the direction of one leader-manager.
- Staff Authority – authority that is based on the expertise and which usually involves advising the line managers.
- Team Authority – is granted to committees or work teams involved in an organization’s daily operations. Work teams are group of operating employees who shared a common vision , goals and objectives.
- Drawing that shows how the parts of the organizations are link.
- It depicts the formal organizational relationship, areas of responsibility and accountability and channel of communication.
- Depicts an organization’s structure.
- Depicts and identifies role and expectations, arrangement of positions and working relationships.
- Dotted or Unbroken line – represents staff positions/staff authority (advisor to the line managers).
- Centrality – refers to the location of a position on an organizational chart where frequent and various types of communication occur. Determined by organizational distance; those with small organizational distance receive more information than those who are more peripherally located.
- Solid Horizontal Line – represent same positions but different functions.
- Solid Vertical Line – chain of command form authority to subordinates (line authority)
1. Tall/Centralized Structure
- Responsible for only few subordinates so there is narrow span of control
- Because of the vertical in nature, there are many levels of communication
- Communication is difficult and messages do not get to the top.
- Workers are boss-oriented because of close contact with their supervisor.
2. Flat/Decentralized Structure
- Characterized by few levels and a broad span of control
- Communication is easy and direct
Advantages:
- Shortens the administrative distance from the top to the lower
- Solutions to problems are easily carried out/fast response
- Workers developed their abilities and autonomy
Disadvantage:
- Impractical in large organization.
1. Line Organization/Bureaucratic/Pyramidal
- There is clearly defined superior-subordinate relationship
- AR ►and power are concentrated at the top
2. Flat/Horizontal Organization
- Decentralized type
- Applicable in small organization
- Nurses become productive and directly involved in the decision making skills
- Workers become satisfied
3. Functional Organization
- Permits a specialist to aid line position within a limited and clearly defined scope of authority
4. Ad Hoc Organization
- Modification of bureaucratic structure
5. Matrix structure
- Focus on both product and functions
- Most complex
- Has both vertical and horizontal chain of command and line of communication
- Process of assigning competent people to fulfill the roles designated for the organizational structure through recruitment, selection and development, induction and orientation of the new staff of the goals, vision, mission, philosophy etc.
- Preparing to Recruit – types and number of personnel
- Attracting a Staff – formal advertisement
- Recruiting and Selecting a Staff – interview ►induction ►orientation ►job order ►pre-employment testing ►signing of contract
Staffing Pattern – plan that articulates how many and what kind of staff are needed/shift or per day in ►unit or in ►department.
Two Ways of Developing a Staffing Pattern
- Generating the full time equivalents of an employee
- Determine the nurse-patient ratio in providing nursing care
- 1.0 FTE = works 5 days/week, 8 hours/day
- 0.5 FTE = part time employee who works 5 days/2 weeks
1. Benchmarking
- Management tool for seeking out the best practice in one’s industry so as to improve one’s performance.
- Process of measuring products, practices and services against best performing organization as atool for identifying desired standards of organizational performance.
2. Regulatory Requirements – mandated by RA 3. Skill Mix – percent or ratio of professionals to non professional Ex: 40 FTE (20 RN + 20 non RN) = 50% RN mix 4. Staff Support – staff support in place for the operations of the units or department. 5. Historical Information – review of any data on quality or staff perception regarding the effectiveness of the previous staffing pattern
- Measuring tool used to articulate the nursing workload for specific patient or group of patients over a specific time.
- Patient Acuity – measure of nursing workload that is generated for each patient.
- Self care or minimal care patients are capable of carrying ADL, e.g., hygiene, meals etc.
- Intermediate or moderate care requires some help from the nursing staff with special treatments or certain aspects of personal care, e.g., patients with IV fluids , catheter, respirator, etc.
- Total care patients are those who are bedridden and who lack strength and mobility to do average daily living. Ex: patients on CBR, immediate post-op, with contraptions.
- Intensive care patients are those who are critically ill and in constant danger of death or serious injury . Ex: comatose, bedridden etc.
- Timetable showing planned work days and shifts for nursing personnel.
Issues to consider in scheduling staff:
- Patient type and acuity
- Number of patients
- Experience of Staff
- Support available to the staff
Shifting Variations
- 3 shift (8 hr shift)
- 12 hr shift
- 10 hr shift
- Weekend option
- Rotating work shift
- Self-scheduling – staff makes their own schedule
- Permanent work shift
- Floaters – “on-call”
Forty Hour Week Law – based on RA5901
- No work, no pay
- Entitled to 2-week sick leave and off duty for 2 days
- Special Holidays – with pay
- Act of issuing of orders, assignments, instructions, to accomplish organizational goals and objectives.
- Delegation – entails responsibility
- Assignments – no responsibility
- Communication
- Coordination
Communication – exchange of ideas, thoughts or information through verbal speech, writing and signals
1. Physical Barriers
- Environmental factors that prevent or reduce the opportunities for communication. Ex: Distance and Noise
2. Social and Psychological Barriers
- Blocks or inhibitors of communication that rise from the judgment, emotions, social values of people.Ex: stress, trust, fear , defensiveness
- Internal climate (values, feelings, temperament and stress levels) and external climate (weather, timing, temperature, lack of validation to the message).
3. Semantics
- Words, figures, symbols,penmanship and interpretation of the message through signs and symbols.
4. Interpretations
- Defects in communication skills by verbalizing, listening, writing, reading and telephony
- Act of assigning to someone else a portion of the work to be done with corresponding authority, responsibility and accountability (ARA).
- According to ANA, it is the trabsfer of responsibilities for the performance of the task from one person to another
- Much of the work of manager is accomplished by transferring the responsibilities to subordinates
- Manager delegate routine task so that they are free to handle problems that are more complex or require higher level of expertise
- Delegate routine task if someone else is better prepared or has greater expertise or knowledge in solving the problems
- Does not trust
- Fear of mistake
- Fear of criticism
- Fear of own ability to delegate
- Managers believe that they can do the work faster and better
- Managers believe that the responsibility may be rejected if delegated
- Managers who are lazy
- Manager who are overburdened and exhausted
- Improper Delegation – delegating at the wrong person, time, tasks and beyond the capability of the subordinates.
- Identify necessary skills and levels
- Select most capable personnel
- Communicate goal clearly
- Empower the delegate
- Set deadlines and monitor progress
- Model the role and provide guidance
- Evaluate performance
- Motivation – whatever influences our choices and creates direction, intensity, and persistence in our behavior.
- Supervision – guiding and directing the work to be done. It entails motivating and encouraging the staff to participate in the activities to meet the goals and objectives for personal development in making the work better.
- Coordination – arranging in proper order. It creates harmony in all activities to facilitate success of work
- Conflict – internal and external discord that results in from differences in ideas, values or feelings between 2 or more people. It arises because of differences in economic and professional values.
- Management: Set Goals
- Disruptive Conflict – takes place in environment filled with anger, fear and stress. There is no mutually acceptable set of rules and the goal of each party is the elimination of each opponent.
- Win lose strategy
- Loses feels angry
- Restri ction – autocratic coercive style that uses indirect and obstructive expression of conflict.
- Smoothing Behavior – persuades the opponent in a diplomatic way
- Avoidance Behavior – 2 parties are aware of the conflict but choose not to acknowledge or attempt to resolve it.
- Majority rule – unanimous decision
- Compromising – consensus strategy where each side agrees solutions
- Interactive Problem Solving – constructive process in which the parties involve recognized that conflict, assist and openly try to solve the problems
- Win-Win Strategy – focuses on goals and attempts to meet the needs of both parties.
- Lose-Lose Strategy – neither side wins
- Confrontation – most effective means of resolving the conflict. Resolves through knowledge and reason brought out in an open.
- Negotiation – “give and take”
9 thoughts on “Nursing Management: Guide to Organizing, Staffing, Scheduling, Directing & Delegation”
nice article :)
Nice staff….so helpful.
Very informative… love it, thanks! ❤
Very helpful in my leadership and management course 🙏
VERY INFORMATIVE.THANKS
Awesome and knowledgeful ,thanks 💕🌹🤗🧑⚕️
I have learnt a lot and it has help my long essay
Well discussed piece of work 👏
Very informative and helpful ; )
Leave a Comment Cancel reply

- school Campus Bookshelves
- menu_book Bookshelves
- perm_media Learning Objects
- login Login
- how_to_reg Request Instructor Account
- hub Instructor Commons
- Download Page (PDF)
- Download Full Book (PDF)
- Periodic Table
- Physics Constants
- Scientific Calculator
- Reference & Cite
- Tools expand_more
- Readability
selected template will load here
This action is not available.

4.1: Leadership and Management Introduction
- Last updated
- Save as PDF
- Page ID 63153

- Ernstmeyer & Christman (Eds.)
- Chippewa Valley Technical College via OpenRN
Learning Objectives
- Compare and contrast the role of a leader and a manager
- Examine the roles of team members
- Identify the activities managers perform
- Describe the role of the RN as a leader and change agent
- Evaluate the effects of power, empowerment, and motivation in leading and managing a nursing team
- Recognize limitations of self and others and utilize resources
As a nursing student preparing to graduate, you have spent countless hours on developing clinical skills, analyzing disease processes, creating care plans, and cultivating clinical judgment. In comparison, you have likely spent much less time on developing management and leadership skills. Yet, soon after beginning your first job as a registered nurse, you will become involved in numerous situations requiring nursing leadership and management skills. Some of these situations include the following:
- Prioritizing care for a group of assigned clients
- Collaborating with interprofessional team members regarding client care
- Participating in an interdisciplinary team conference
- Acting as a liaison when establishing community resources for a patient being discharged home
- Serving on a unit committee
- Investigating and implementing a new evidence-based best practice
- Mentoring nursing students
Delivering safe, quality client care often requires registered nurses (RN) to manage care provided by the nursing team. Making assignments, delegating tasks, and supervising nursing team members are essential managerial components of an entry-level staff RN role. As previously discussed, nursing team members include RNs, licensed practical/vocational nurses (LPN/VN), and assistive personnel (AP). [1]
Read more about assigning, delegating, and supervising in the “ Delegation and Supervision ” chapter.
An RN is expected to demonstrate leadership and management skills in many facets of the role. Nurses manage care for high-acuity patients as they are admitted, transferred, and discharged; coordinate care among a variety of diverse health professionals; advocate for clients’ needs; and manage limited resources with shrinking budgets. [2]
Read more about collaborating and communicating with the interprofessional team; advocating for clients; and admitting, transferring, and discharging clients in the “ Collaboration Within the Interprofessional Team ” chapter.
An article published in the Online Journal of Issues in Nursing states, “With the growing complexity of healthcare practice environments and pending nurse leader retirements, the development of future nurse leaders is increasingly important.” [3] This chapter will explore leadership and management responsibilities of an RN. Leadership styles are introduced, and change theories are discussed as a means for implementing change in the health care system.
- American Nurses Association & NCSBN. (2019). National guidelines for nursing delegation. https://www.ncsbn.org/NGND-PosPaper_06.pdf ↵
- Cherry, B., & Jacob, S. R. (2017). Nursing leadership and management. In Cherry, B. & Jacob, S. (Eds.), Contemporary nursing: Issues, trends, and management (8th ed.). Elsevier, pp. 294-314. ↵
- Dyess, S. M., Sherman, R. O., Pratt, B. A., & Chiang-Hanisko, L. (2016). Growing nurse leaders: Their perspectives on nursing leadership and today’s practice environment. OJIN: The Online Journal of Issues in Nursing, 21 (1). https://ojin.nursingworld.org/MainMenuCategories/ANAMarketplace/ANAPeriodicals/OJIN/TableofContents/Vol-21-2016/No1-Jan-2016/Articles-Previous-Topics/Growing-Nurse-Leaders.html ↵
An official website of the United States government
The .gov means it's official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you're on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
- Browse Titles
NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health.
Open Resources for Nursing (Open RN); Ernstmeyer K, Christman E, editors. Nursing Management and Professional Concepts [Internet]. Eau Claire (WI): Chippewa Valley Technical College; 2022.

Nursing Management and Professional Concepts [Internet].
- About Open RN
Chapter 2 - Prioritization
2.1. prioritization introduction, learning objectives.
• Prioritize nursing care based on patient acuity
• Use principles of time management to organize work
• Analyze effectiveness of time management strategies
• Use critical thinking to prioritize nursing care for patients
• Apply a framework for prioritization (e.g., Maslow, ABCs)
“So much to do, so little time.” This is a common mantra of today’s practicing nurse in various health care settings. Whether practicing in acute inpatient care, long-term care, clinics, home care, or other agencies, nurses may feel there is “not enough of them to go around.”
The health care system faces a significant challenge in balancing the ever-expanding task of meeting patient care needs with scarce nursing resources that has even worsened as a result of the COVID-19 pandemic. With a limited supply of registered nurses, nurse managers are often challenged to implement creative staffing practices such as sending staff to units where they do not normally work (i.e., floating), implementing mandatory staffing and/or overtime, utilizing travel nurses, or using other practices to meet patient care demands.[ 1 ] Staffing strategies can result in nurses experiencing increased patient assignments and workloads, extended shifts, or temporary suspension of paid time off. Nurses may receive a barrage of calls and text messages offering “extra shifts” and bonus pay, and although the extra pay may be welcomed, they often eventually feel burnt out trying to meet the ever-expanding demands of the patient-care environment.
A novice nurse who is still learning how to navigate the complex health care environment and provide optimal patient care may feel overwhelmed by these conditions. Novice nurses frequently report increased levels of stress and disillusionment as they transition to the reality of the nursing role.[ 2 ] How can we address this professional dilemma and enhance the novice nurse’s successful role transition to practice? The novice nurse must enter the profession with purposeful tools and strategies to help prioritize tasks and manage time so they can confidently address patient care needs, balance role demands, and manage day-to-day nursing activities.
Let’s take a closer look at the foundational concepts related to prioritization and time management in the nursing profession.
2.2. TENETS OF PRIORITIZATION
Prioritization.
As new nurses begin their career, they look forward to caring for others, promoting health, and saving lives. However, when entering the health care environment, they often discover there are numerous and competing demands for their time and attention. Patient care is often interrupted by call lights, rounding physicians, and phone calls from the laboratory department or other interprofessional team members. Even individuals who are strategic and energized in their planning can feel frustrated as their task lists and planned patient-care activities build into a long collection of “to dos.”
Without utilization of appropriate prioritization strategies, nurses can experience time scarcity , a feeling of racing against a clock that is continually working against them. Functioning under the burden of time scarcity can cause feelings of frustration, inadequacy, and eventually burnout. Time scarcity can also impact patient safety, resulting in adverse events and increased mortality.[ 1 ] Additionally, missed or rushed nursing activities can negatively impact patient satisfaction scores that ultimately affect an institution’s reimbursement levels.
It is vital for nurses to plan patient care and implement their task lists while ensuring that critical interventions are safely implemented first. Identifying priority patient problems and implementing priority interventions are skills that require ongoing cultivation as one gains experience in the practice environment.[ 2 ] To develop these skills, students must develop an understanding of organizing frameworks and prioritization processes for delineating care needs. These frameworks provide structure and guidance for meeting the multiple and ever-changing demands in the complex health care environment.
Let’s consider a clinical scenario in the following box to better understand the implications of prioritization and outcomes.
Imagine you are beginning your shift on a busy medical-surgical unit. You receive a handoff report on four medical-surgical patients from the night shift nurse:
• Patient A is a 34-year-old total knee replacement patient, post-op Day 1, who had an uneventful night. It is anticipated that she will be discharged today and needs patient education for self-care at home.
• Patient B is a 67-year-old male admitted with weakness, confusion, and a suspected urinary tract infection. He has been restless and attempting to get out of bed throughout the night. He has a bed alarm in place.
• Patient C is a 49-year-old male, post-op Day 1 for a total hip replacement. He has been frequently using his patient-controlled analgesia (PCA) pump and last rated his pain as a “6.”
• Patient D is a 73-year-old male admitted for pneumonia. He has been hospitalized for three days and receiving intravenous (IV) antibiotics. His next dose is due in an hour. His oxygen requirements have decreased from 4 L/minute of oxygen by nasal cannula to 2 L/minute by nasal cannula.
Based on the handoff report you received, you ask the nursing assistant to check on Patient B while you do an initial assessment on Patient D. As you are assessing Patient D’s oxygenation status, you receive a phone call from the laboratory department relating a critical lab value on Patient C, indicating his hemoglobin is low. The provider calls and orders a STAT blood transfusion for Patient C. Patient A rings the call light and states she and her husband have questions about her discharge and are ready to go home. The nursing assistant finds you and reports that Patient B got out of bed and experienced a fall during the handoff reports.
It is common for nurses to manage multiple and ever-changing tasks and activities like this scenario, illustrating the importance of self-organization and priority setting. This chapter will further discuss the tools nurses can use for prioritization.
2.3. TOOLS FOR PRIORITIZING
Prioritization of care for multiple patients while also performing daily nursing tasks can feel overwhelming in today’s fast-paced health care system. Because of the rapid and ever-changing conditions of patients and the structure of one’s workday, nurses must use organizational frameworks to prioritize actions and interventions. These frameworks can help ease anxiety, enhance personal organization and confidence, and ensure patient safety.
Acuity and intensity are foundational concepts for prioritizing nursing care and interventions. Acuity refers to the level of patient care that is required based on the severity of a patient’s illness or condition. For example, acuity may include characteristics such as unstable vital signs, oxygenation therapy, high-risk IV medications, multiple drainage devices, or uncontrolled pain. A “high-acuity” patient requires several nursing interventions and frequent nursing assessments.
Intensity addresses the time needed to complete nursing care and interventions such as providing assistance with activities of daily living (ADLs), performing wound care, or administering several medication passes. For example, a “high-intensity” patient generally requires frequent or long periods of psychosocial, educational, or hygiene care from nursing staff members. High-intensity patients may also have increased needs for safety monitoring, familial support, or other needs.[ 1 ]
Many health care organizations structure their staffing assignments based on acuity and intensity ratings to help provide equity in staff assignments. Acuity helps to ensure that nursing care is strategically divided among nursing staff. An equitable assignment of patients benefits both the nurse and patient by helping to ensure that patient care needs do not overwhelm individual staff and safe care is provided.
Organizations use a variety of systems when determining patient acuity with rating scales based on nursing care delivery, patient stability, and care needs. See an example of a patient acuity tool published in the American Nurse in Table 2.3 .[ 2 ] In this example, ratings range from 1 to 4, with a rating of 1 indicating a relatively stable patient requiring minimal individualized nursing care and intervention. A rating of 2 reflects a patient with a moderate risk who may require more frequent intervention or assessment. A rating of 3 is attributed to a complex patient who requires frequent intervention and assessment. This patient might also be a new admission or someone who is confused and requires more direct observation. A rating of 4 reflects a high-risk patient. For example, this individual may be experiencing frequent changes in vital signs, may require complex interventions such as the administration of blood transfusions, or may be experiencing significant uncontrolled pain. An individual with a rating of 4 requires more direct nursing care and intervention than a patient with a rating of 1 or 2. [3]
Example of a Patient Acuity Tool [ 4 ]
View in own window
Read more about using a patient acuity tool on a medical-surgical unit.
Rating scales may vary among institutions, but the principles of the rating system remain the same. Organizations include various patient care elements when constructing their staffing plans for each unit. Read more information about staffing models and acuity in the following box.
Staffing Models and Acuity
Organizations that base staffing on acuity systems attempt to evenly staff patient assignments according to their acuity ratings. This means that when comparing patient assignments across nurses on a unit, similar acuity team scores should be seen with the goal of achieving equitable and safe division of workload across the nursing team. For example, one nurse should not have a total acuity score of 6 for their patient assignments while another nurse has a score of 15. If this situation occurred, the variation in scoring reflects a discrepancy in workload balance and would likely be perceived by nursing peers as unfair. Using acuity-rating staffing models is helpful to reflect the individualized nursing care required by different patients.
Alternatively, nurse staffing models may be determined by staffing ratio. Ratio-based staffing models are more straightforward in nature, where each nurse is assigned care for a set number of patients during their shift. Ratio-based staffing models may be useful for administrators creating budget requests based on the number of staff required for patient care, but can lead to an inequitable division of work across the nursing team when patient acuity is not considered. Increasingly complex patients require more time and interventions than others, so a blend of both ratio and acuity-based staffing is helpful when determining staffing assignments.[ 5 ]
As a practicing nurse, you will be oriented to the elements of acuity ratings within your health care organization, but it is also important to understand how you can use these acuity ratings for your own prioritization and task delineation. Let’s consider the Scenario B in the following box to better understand how acuity ratings can be useful for prioritizing nursing care.
You report to work at 6 a.m. for your nursing shift on a busy medical-surgical unit. Prior to receiving the handoff report from your night shift nursing colleagues, you review the unit staffing grid and see that you have been assigned to four patients to start your day. The patients have the following acuity ratings:
Patient A: 45-year-old patient with paraplegia admitted for an infected sacral wound, with an acuity rating of 4.
Patient B: 87-year-old patient with pneumonia with a low grade fever of 99.7 F and receiving oxygen at 2 L/minute via nasal cannula, with an acuity rating of 2.
Patient C: 63-year-old patient who is postoperative Day 1 from a right total hip replacement and is receiving pain management via a PCA pump, with an acuity rating of 2.
Patient D: 83-year-old patient admitted with a UTI who is finishing an IV antibiotic cycle and will be discharged home today, with an acuity rating of 1.
Based on the acuity rating system, your patient assignment load receives an overall acuity score of 9. Consider how you might use their acuity ratings to help you prioritize your care. Based on what is known about the patients related to their acuity rating, whom might you identify as your care priority? Although this can feel like a challenging question to answer because of the many unknown elements in the situation using acuity numbers alone, Patient A with an acuity rating of 4 would be identified as the care priority requiring assessment early in your shift.
Although acuity can a useful tool for determining care priorities, it is important to recognize the limitations of this tool and consider how other patient needs impact prioritization.
Maslow’s Hierarchy of Needs
When thinking back to your first nursing or psychology course, you may recall a historical theory of human motivation based on various levels of human needs called Maslow’s Hierarchy of Needs. Maslow’s Hierarchy of Needs reflects foundational human needs with progressive steps moving towards higher levels of achievement. This hierarchy of needs is traditionally represented as a pyramid with the base of the pyramid serving as essential needs that must be addressed before one can progress to another area of need.[ 6 ] See Figure 2.1 [ 7 ] for an illustration of Maslow’s Hierarchy of Needs.
Maslow’s Hierarchy of Needs places physiological needs as the foundational base of the pyramid.[ 8 ] Physiological needs include oxygen, food, water, sex, sleep, homeostasis, and excretion. The second level of Maslow’s hierarchy reflects safety needs. Safety needs include elements that keep individuals safe from harm. Examples of safety needs in health care include fall precautions. The third level of Maslow’s hierarchy reflects emotional needs such as love and a sense of belonging. These needs are often reflected in an individual’s relationships with family members and friends. The top two levels of Maslow’s hierarchy include esteem and self-actualization. An example of addressing these needs in a health care setting is helping an individual build self-confidence in performing blood glucose checks that leads to improved self-management of their diabetes.
So how does Maslow’s theory impact prioritization? To better understand the application of Maslow’s theory to prioritization, consider Scenario C in the following box.
You are an emergency response nurse working at a local shelter in a community that has suffered a devastating hurricane. Many individuals have relocated to the shelter for safety in the aftermath of the hurricane. Much of the community is still without electricity and clean water, and many homes have been destroyed. You approach a young woman who has a laceration on her scalp that is bleeding through her gauze dressing. The woman is weeping as she describes the loss of her home stating, “I have lost everything! I just don’t know what I am going to do now. It has been a day since I have had water or anything to drink. I don’t know where my sister is, and I can’t reach any of my family to find out if they are okay!”
Despite this relatively brief interaction, this woman has shared with you a variety of needs. She has demonstrated a need for food, water, shelter, homeostasis, and family. As the nurse caring for her, it might be challenging to think about where to begin her care. These thoughts could be racing through your mind:
Should I begin to make phone calls to try and find her family? Maybe then she would be able to calm down.
Should I get her on the list for the homeless shelter so she wouldn’t have to worry about where she will sleep tonight?
She hasn’t eaten in awhile; I should probably find her something to eat.
All of these needs are important and should be addressed at some point, but Maslow’s hierarchy provides guidance on what needs must be addressed first. Use the foundational level of Maslow’s pyramid of physiological needs as the top priority for care. The woman is bleeding heavily from a head wound and has had limited fluid intake. As the nurse caring for this patient, it is important to immediately intervene to stop the bleeding and restore fluid volume. Stabilizing the patient by addressing her physiological needs is required before undertaking additional measures such as contacting her family. Imagine if instead you made phone calls to find the patient’s family and didn’t address the bleeding or dehydration – you might return to a severely hypovolemic patient who has deteriorated and may be near death. In this example, prioritizing emotional needs above physiological needs can lead to significant harm to the patient.
Although this is a relatively straightforward example, the principles behind the application of Maslow’s hierarchy are essential. Addressing physiological needs before progressing toward additional need categories concentrates efforts on the most vital elements to enhance patient well-being. Maslow’s hierarchy provides the nurse with a helpful framework for identifying and prioritizing critical patient care needs.
Airway, breathing, and circulation, otherwise known by the mnemonic “ABCs,” are another foundational element to assist the nurse in prioritization. Like Maslow’s hierarchy, using the ABCs to guide decision-making concentrates on the most critical needs for preserving human life. If a patient does not have a patent airway, is unable to breathe, or has inadequate circulation, very little of what else we do matters. The patient’s ABCs are reflected in Maslow’s foundational level of physiological needs and direct critical nursing actions and timely interventions. Let’s consider Scenario D in the following box regarding prioritization using the ABCs and the physiological base of Maslow’s hierarchy.
You are a nurse on a busy cardiac floor charting your morning assessments on a computer at the nurses’ station. Down the hall from where you are charting, two of your assigned patients are resting comfortably in Room 504 and Room 506. Suddenly, both call lights ring from the rooms, and you answer them via the intercom at the nurses’ station.
Room 504 has an 87-year-old male who has been admitted with heart failure, weakness, and confusion. He has a bed alarm for safety and has been ringing his call bell for assistance appropriately throughout the shift. He requires assistance to get out of bed to use the bathroom. He received his morning medications, which included a diuretic about 30 minutes previously, and now reports significant urge to void and needs assistance to the bathroom.
Room 506 has a 47-year-old woman who was hospitalized with new onset atrial fibrillation with rapid ventricular response. The patient underwent a cardioversion procedure yesterday that resulted in successful conversion of her heart back into normal sinus rhythm. She is reporting via the intercom that her “heart feels like it is doing that fluttering thing again” and she is having chest pain with breathlessness.
Based upon these two patient scenarios, it might be difficult to determine whom you should see first. Both patients are demonstrating needs in the foundational physiological level of Maslow’s hierarchy and require assistance. To prioritize between these patients’ physiological needs, the nurse can apply the principles of the ABCs to determine intervention. The patient in Room 506 reports both breathing and circulation issues, warning indicators that action is needed immediately. Although the patient in Room 504 also has an urgent physiological elimination need, it does not overtake the critical one experienced by the patient in Room 506. The nurse should immediately assess the patient in Room 506 while also calling for assistance from a team member to assist the patient in Room 504.
Prioritizing what should be done and when it can be done can be a challenging task when several patients all have physiological needs. Recently, there has been professional acknowledgement of the cognitive challenge for novice nurses in differentiating physiological needs. To expand on the principles of prioritizing using the ABCs, the CURE hierarchy has been introduced to help novice nurses better understand how to manage competing patient needs. The CURE hierarchy uses the acronym “CURE” to guide prioritization based on identifying the differences among Critical needs, Urgent needs, Routine needs, and Extras.[ 9 ]
“Critical” patient needs require immediate action. Examples of critical needs align with the ABCs and Maslow’s physiological needs, such as symptoms of respiratory distress, chest pain, and airway compromise. No matter the complexity of their shift, nurses can be assured that addressing patients’ critical needs is the correct prioritization of their time and energies.
After critical patient care needs have been addressed, nurses can then address “urgent” needs. Urgent needs are characterized as needs that cause patient discomfort or place the patient at a significant safety risk.[ 10 ]
The third part of the CURE hierarchy reflects “routine” patient needs. Routine patient needs can also be characterized as “typical daily nursing care” because the majority of a standard nursing shift is spent addressing routine patient needs. Examples of routine daily nursing care include actions such as administering medication and performing physical assessments.[ 11 ] Although a nurse’s typical shift in a hospital setting includes these routine patient needs, they do not supersede critical or urgent patient needs.
The final component of the CURE hierarchy is known as “extras.” Extras refer to activities performed in the care setting to facilitate patient comfort but are not essential.[ 12 ] Examples of extra activities include providing a massage for comfort or washing a patient’s hair. If a nurse has sufficient time to perform extra activities, they contribute to a patient’s feeling of satisfaction regarding their care, but these activities are not essential to achieve patient outcomes.
Let’s apply the CURE mnemonic to patient care in the following box.
If we return to Scenario D regarding patients in Room 504 and 506, we can see the patient in Room 504 is having urgent needs. He is experiencing a physiological need to urgently use the restroom and may also have safety concerns if he does not receive assistance and attempts to get up on his own because of weakness. He is on a bed alarm, which reflects safety considerations related to his potential to get out of bed without assistance. Despite these urgent indicators, the patient in Room 506 is experiencing a critical need and takes priority. Recall that critical needs require immediate nursing action to prevent patient deterioration. The patient in Room 506 with a rapid, fluttering heartbeat and shortness of breath has a critical need because without prompt assessment and intervention, their condition could rapidly decline and become fatal.
In addition to using the identified frameworks and tools to assist with priority setting, nurses must also look at their patients’ data cues to help them identify care priorities. Data cues are pieces of significant clinical information that direct the nurse toward a potential clinical concern or a change in condition. For example, have the patient’s vital signs worsened over the last few hours? Is there a new laboratory result that is concerning? Data cues are used in conjunction with prioritization frameworks to help the nurse holistically understand the patient’s current status and where nursing interventions should be directed. Common categories of data clues include acute versus chronic conditions, actual versus potential problems, unexpected versus expected conditions, information obtained from the review of a patient’s chart, and diagnostic information.
Acute Versus Chronic Conditions
A common data cue that nurses use to prioritize care is considering if a condition or symptom is acute or chronic. Acute conditions have a sudden and severe onset. These conditions occur due to a sudden illness or injury, and the body often has a significant response as it attempts to adapt. Chronic conditions have a slow onset and may gradually worsen over time. The difference between an acute versus a chronic condition relates to the body’s adaptation response. Individuals with chronic conditions often experience less symptom exacerbation because their body has had time to adjust to the illness or injury. Let’s consider an example of two patients admitted to the medical-surgical unit complaining of pain in Scenario E in the following box.
As part of your patient assignment on a medical-surgical unit, you are caring for two patients who both ring the call light and report pain at the start of the shift. Patient A was recently admitted with acute appendicitis, and Patient B was admitted for observation due to weakness. Not knowing any additional details about the patients’ conditions or current symptoms, which patient would receive priority in your assessment? Based on using the data cue of acute versus chronic conditions, Patient A with a diagnosis of acute appendicitis would receive top priority for assessment over a patient with chronic pain due to osteoarthritis. Patients experiencing acute pain require immediate nursing assessment and intervention because it can indicate a change in condition. Acute pain also elicits physiological effects related to the stress response, such as elevated heart rate, blood pressure, and respiratory rate, and should be addressed quickly.
Actual Versus Potential Problems
Nursing diagnoses and the nursing care plan have significant roles in directing prioritization when interpreting assessment data cues. Actual problems refer to a clinical problem that is actively occurring with the patient. A risk problem indicates the patient may potentially experience a problem but they do not have current signs or symptoms of the problem actively occurring.
Consider an example of prioritizing actual and potential problems in Scenario F in the following box.
A 74-year-old woman with a previous history of chronic obstructive pulmonary disease (COPD) is admitted to the hospital for pneumonia. She has generalized weakness, a weak cough, and crackles in the bases of her lungs. She is receiving IV antibiotics, fluids, and oxygen therapy. The patient can sit at the side of the bed and ambulate with the assistance of staff, although she requires significant encouragement to ambulate.
Nursing diagnoses are established for this patient as part of the care planning process. One nursing diagnosis for this patient is Ineffective Airway Clearance . This nursing diagnosis is an actual problem because the patient is currently exhibiting signs of poor airway clearance with an ineffective cough and crackles in the lungs. Nursing interventions related to this diagnosis include coughing and deep breathing, administering nebulizer treatment, and evaluating the effectiveness of oxygen therapy. The patient also has the nursing diagnosis Risk for Skin Breakdown based on her weakness and lack of motivation to ambulate. Nursing interventions related to this diagnosis include repositioning every two hours and assisting with ambulation twice daily.
The established nursing diagnoses provide cues for prioritizing care. For example, if the nurse enters the patient’s room and discovers the patient is experiencing increased shortness of breath, nursing interventions to improve the patient’s respiratory status receive top priority before attempting to get the patient to ambulate.
Although there may be times when risk problems may supersede actual problems, looking to the “actual” nursing problems can provide clues to assist with prioritization.
Unexpected Versus Expected Conditions
In a similar manner to using acute versus chronic conditions as a cue for prioritization, it is also important to consider if a client’s signs and symptoms are “expected” or “unexpected” based on their overall condition. Unexpected conditions are findings that are not likely to occur in the normal progression of an illness, disease, or injury. Expected conditions are findings that are likely to occur or are anticipated in the course of an illness, disease, or injury. Unexpected findings often require immediate action by the nurse.
Let’s apply this tool to the two patients previously discussed in Scenario E. As you recall, both Patient A (with acute appendicitis) and Patient B (with weakness and diagnosed with osteoarthritis) are reporting pain. Acute pain typically receives priority over chronic pain. But what if both patients are also reporting nausea and have an elevated temperature? Although these symptoms must be addressed in both patients, they are “expected” symptoms with acute appendicitis (and typically addressed in the treatment plan) but are “unexpected” for the patient with osteoarthritis. Critical thinking alerts you to the unexpected nature of these symptoms in Patient B, so they receive priority for assessment and nursing interventions.
Handoff Report/Chart Review
Additional data cues that are helpful in guiding prioritization come from information obtained during a handoff nursing report and review of the patient chart. These data cues can be used to establish a patient’s baseline status and prioritize new clinical concerns based on abnormal assessment findings. Let’s consider Scenario G in the following box based on cues from a handoff report and how it might be used to help prioritize nursing care.
Imagine you are receiving the following handoff report from the night shift nurse for a patient admitted to the medical-surgical unit with pneumonia:
At the beginning of my shift, the patient was on room air with an oxygen saturation of 93%. She had slight crackles in both bases of her posterior lungs. At 0530, the patient rang the call light to go to the bathroom. As I escorted her to the bathroom, she appeared slightly short of breath. Upon returning the patient to bed, I rechecked her vital signs and found her oxygen saturation at 88% on room air and respiratory rate of 20. I listened to her lung sounds and noticed more persistent crackles and coarseness than at bedtime. I placed the patient on 2 L/minute of oxygen via nasal cannula. Within 5 minutes, her oxygen saturation increased to 92%, and she reported increased ease in respiration.
Based on the handoff report, the night shift nurse provided substantial clinical evidence that the patient may be experiencing a change in condition. Although these changes could be attributed to lack of lung expansion that occurred while the patient was sleeping, there is enough information to indicate to the oncoming nurse that follow-up assessment and interventions should be prioritized for this patient because of potentially worsening respiratory status. In this manner, identifying data cues from a handoff report can assist with prioritization.
Now imagine the night shift nurse had not reported this information during the handoff report. Is there another method for identifying potential changes in patient condition? Many nurses develop a habit of reviewing their patients’ charts at the start of every shift to identify trends and “baselines” in patient condition. For example, a chart review reveals a patient’s heart rate on admission was 105 beats per minute. If the patient continues to have a heart rate in the low 100s, the nurse is not likely to be concerned if today’s vital signs reveal a heart rate in the low 100s. Conversely, if a patient’s heart rate on admission was in the 60s and has remained in the 60s throughout their hospitalization, but it is now in the 100s, this finding is an important cue requiring prioritized assessment and intervention.
Diagnostic Information
Diagnostic results are also important when prioritizing care. In fact, the National Patient Safety Goals from The Joint Commission include prompt reporting of important test results. New abnormal laboratory results are typically flagged in a patient’s chart or are reported directly by phone to the nurse by the laboratory as they become available. Newly reported abnormal results, such as elevated blood levels or changes on a chest X-ray, may indicate a patient’s change in condition and require additional interventions. For example, consider Scenario H in which you are the nurse providing care for five medical-surgical patients.
You completed morning assessments on your assigned five patients. Patient A previously underwent a total right knee replacement and will be discharged home today. You are about to enter Patient A’s room to begin discharge teaching when you receive a phone call from the laboratory department, reporting a critical hemoglobin of 6.9 gm/dL on Patient B. Rather than enter Patient A’s room to perform discharge teaching, you immediately reprioritize your care. You call the primary provider to report Patient B’s critical hemoglobin level and determine if additional intervention, such as a blood transfusion, is required.
2.4. CRITICAL THINKING AND CLINICAL REASONING
Prioritization of patient care should be grounded in critical thinking rather than just a checklist of items to be done. Critical thinking is a broad term used in nursing that includes “reasoning about clinical issues such as teamwork, collaboration, and streamlining workflow.”[ 1 ] Certainly, there are many actions that nurses must complete during their shift, but nursing requires adaptation and flexibility to meet emerging patient needs. It can be challenging for a novice nurse to change their mindset regarding their established “plan” for the day, but the sooner a nurse recognizes prioritization is dictated by their patients’ needs, the less frustration the nurse might experience. Prioritization strategies include collection of information and utilization of clinical reasoning to determine the best course of action. Clinical reasoning is defined as, “A complex cognitive process that uses formal and informal thinking strategies to gather and analyze patient information, evaluate the significance of this information, and weigh alternative actions.” [2]
When nurses use critical thinking and clinical reasoning skills, they set forth on a purposeful course of intervention to best meet patient-care needs. Rather than focusing on one’s own priorities, nurses utilizing critical thinking and reasoning skills recognize their actions must be responsive to their patients. For example, a nurse using critical thinking skills understands that scheduled morning medications for their patients may be late if one of the patients on their care team suddenly develops chest pain. Many actions may be added or removed from planned activities throughout the shift based on what is occurring holistically on the patient-care team.
Additionally, in today’s complex health care environment, it is important for the novice nurse to recognize the realities of the current health care environment. Patients have become increasingly complex in their health care needs, and organizations are often challenged to meet these care needs with limited staffing resources. It can become easy to slip into the mindset of disenchantment with the nursing profession when first assuming the reality of patient-care assignments as a novice nurse. The workload of a nurse in practice often looks and feels quite different than that experienced as a nursing student. As a nursing student, there may have been time for lengthy conversations with patients and their family members, ample time to chart, and opportunities to offer personal cares, such as a massage or hair wash. Unfortunately, in the time-constrained realities of today’s health care environment, novice nurses should recognize that even though these “extra” tasks are not always possible, they can still provide quality, safe patient care using the “CURE” prioritization framework. Rather than feeling frustrated about “extras” that cannot be accomplished in time-constrained environments, it is vital to use prioritization strategies to ensure appropriate actions are taken to complete what must be done. With increased clinical experience, a novice nurse typically becomes more comfortable with prioritizing and reprioritizing care.
Prioritization of patient care should be grounded in critical thinking rather than just a checklist of items to be done. Critical thinking is a broad term used in nursing that includes “reasoning about clinical issues such as teamwork, collaboration, and streamlining workflow.”[ 1 ] Certainly, there are many actions that nurses must complete during their shift, but nursing requires adaptation and flexibility to meet emerging patient needs. It can be challenging for a novice nurse to change their mindset regarding their established “plan” for the day, but the sooner a nurse recognizes prioritization is dictated by their patients’ needs, the less frustration the nurse might experience. Prioritization strategies include collection of information and utilization of clinical reasoning to determine the best course of action. Clinical reasoning is defined as, “A complex cognitive process that uses formal and informal thinking strategies to gather and analyze patient information, evaluate the significance of this information, and weigh alternative actions.”[ 2 ]
2.7. LEARNING ACTIVITIES
Learning activities.
(Answers to “Learning Activities” can be found in the “Answer Key” at the end of the book. Answers to interactive activities are provided as immediate feedback.)
The CURE hierarchy has been introduced to help novice nurses better understand how to manage competing patient needs. The CURE hierarchy uses the acronym “CURE” to help guide prioritization based on identifying the differences among C ritical needs, U rgent needs, R outine needs, and E xtras.
You are the nurse caring for the patients in the following table. For each patient, indicate if this is a “critical,” “urgent,” “routine,” or “extra” need.
II. GLOSSARY
Airway, breathing, and circulation.
Nursing problems currently occurring with the patient.
The level of patient care that is required based on the severity of a patient’s illness or condition.
A staffing model used to make patient assignments that reflects the individualized nursing care required for different types of patients.
Conditions having a sudden onset.
Conditions that have a slow onset and may gradually worsen over time.
A complex cognitive process that uses formal and informal thinking strategies to gather and analyze patient information, evaluate the significance of this information, and weigh alternative actions.”[ 1 ]
A broad term used in nursing that includes “reasoning about clinical issues such as teamwork, collaboration, and streamlining workflow.”[ 2 ]
A strategy for prioritization based on identifying “critical” needs, “urgent” needs, “routine” needs, and “extras.”
Pieces of significant clinical information that direct the nurse toward a potential clinical concern or a change in condition.
Conditions that are likely to occur or anticipated in the course of an illness, disease, or injury.
Prioritization strategies often reflect the foundational elements of physiological needs and safety and progr ess toward higher levels.
A staffing model used to make patient assignments in terms of one nurse caring for a set number of patients.
A nursing problem that reflects that a patient may experience a problem but does not currently have signs reflecting the problem is actively occurring.
A prioritization strategy including the review of planned tasks and allocation of time believed to be required to complete each task.
A feeling of racing against a clock that is continually working against you.
Conditions that are not likely to occur in the normal progression of an illness, disease, or injury.
Licensed under a Creative Commons Attribution 4.0 International License. To view a copy of this license, visit https://creativecommons.org/licenses/by/4.0/ .
- Cite this Page Open Resources for Nursing (Open RN); Ernstmeyer K, Christman E, editors. Nursing Management and Professional Concepts [Internet]. Eau Claire (WI): Chippewa Valley Technical College; 2022. Chapter 2 - Prioritization.
- PDF version of this title (18M)
In this Page
- PRIORITIZATION INTRODUCTION
- TENETS OF PRIORITIZATION
- TOOLS FOR PRIORITIZING
- CRITICAL THINKING AND CLINICAL REASONING
- LEARNING ACTIVITIES
Other titles in this collection
- Open RN OER Textbooks

Related Items in Bookshelf
- All Textbooks
Related information
- PMC PubMed Central citations
- PubMed Links to PubMed
Recent Activity
- Chapter 2 - Prioritization - Nursing Management and Professional Concepts Chapter 2 - Prioritization - Nursing Management and Professional Concepts
Your browsing activity is empty.
Activity recording is turned off.
Turn recording back on
Connect with NLM
National Library of Medicine 8600 Rockville Pike Bethesda, MD 20894
Web Policies FOIA HHS Vulnerability Disclosure
Help Accessibility Careers

Want to create or adapt books like this? Learn more about how Pressbooks supports open publishing practices.
3.3 Assignment
Nursing team members receive assignments at the start of their shift. Assignment refers to routine care, activities, and procedures that are within the authorized scope of practice of the RN or LPN/VN or routine functions of the assistive personnel. [1] Assistive personnel (AP) are defined as certified nursing assistants (CNA), client care technicians (PCT), certified medical assistants (CMA), certified medication aides, and home health aides. [2] See Table 3.3a for a description of the typical scope of practice and common tasks performed by members of the nursing team. These tasks are within the traditional role that the team member has acquired through a basic educational program and are the expectation of the hiring agency during a shift of work. Keep in mind that scope of practice is defined by each state’s Nurse Practice Act. Agency policy can be more restrictive than the Nurse Practice Act but cannot be less restrictive.
Assignments are typically made by the charge nurse or nurse supervisor from the previous shift. A charge nurse is an RN who provides leadership on a hospital unit within a health care facility during their shift. Charge nurses perform many of the tasks that general nurses do, but also have some supervisory duties such as making assignments, delegating tasks, preparing schedules, monitoring admissions and discharges, and serving as a staff member resource. [3]
Table 3.3a Nursing Team Members’ Scope of Practice and Common Tasks [4]
An example of a patient assignment is when an RN assigns an LPN to care for a client with stable heart failure. The LPN collects assessment data, monitors intake/output throughout the shift, and administers routine oral medication. The LPN documents this information and reports information back to the RN. This is considered the LPN’s “assignment” because the skills are taught within an LPN educational program and are consistent with the state’s Nursing Practice Act for LPN scope of practice. They are also included in the unit’s job description for an LPN. The RN may also assign this client to a CNA to help provide assistance with tasks that are allowed within the CNA scope. These tasks may include assistance with personal hygiene, toileting, and ambulation. The CNA documents these tasks as they are completed and reports information back to the RN. These tasks are considered the CNA’s assignment because they are taught within a nursing assistant educational program, are consistent with the nursing assistant scope of practice, and are included in the job description for this unit’s nursing assistant role.
Special consideration is required for advanced assistive personnel roles. With increased staffing needs, skills such as administering medications, inserting Foley catheters, or performing injections are included in specialized training programs for assistant personnel. Due to the impact these skills can have on the outcome and safety of the client, the National Council of State Board of Nursing (NCSBN) recommends these activities be considered delegated tasks by the RN or nurse leader. By delegating these advanced skills when appropriate, the nurse validates competency, provides supervision, and maintains accountability for client outcomes. Read more about delegation in the “ Delegation ” subsection of this chapter.
When making assignments to other nursing team members, it is essential for the RN to keep in mind specific tasks that cannot be delegated to other nursing team members. These tasks include, but are not limited to, those tasks described in Table 3.3b.
Table 3.3b Examples of Tasks Outside the Scope of Practice of Nursing Assistive Personnel
As always, refer to the state’s Nurse Practice Act for specific details about nursing team members’ scope of practice. See the following box for an example of the scope of practice for RNs and LPNs according to Wisconsin’s Nurse Practice Act.
Read more information about scope and standards of practice for RNs and LPNs in Wisconsin’s Nurse Practice Act, Chapter N6 PDF.
- American Nurses Association and NCSBN. (2019). National guidelines for nursing delegation . https://www.ncsbn.org/NGND-PosPaper_06.pdf ↵
- RegisteredNursing.org. (2021, April 13). What is a charge nurse? https://www.registerednursing.org/specialty/charge-nurse/ ↵
- RegisteredNursing.org. (2021, January 27). Assignment, delegation and supervision: NCLEX-RN. https://www.registerednursing.org/nclex/assignment-delegation-supervision/ ↵
- State of Wisconsin Department of Health Services. (2018). Medication administration by unlicensed assistive personnel (UAP): Guidelines for registered nurses delegating medication administration to unlicensed assistive personnel. https://www.dhs.wisconsin.gov/publications/p01908.pdf ↵
Routine care, activities, and procedures that are within the authorized scope of practice of the RN, LPN/VN, or routine functions of the assistive personnel.
Leadership and Management of Nursing Care Copyright © 2022 by Kim Belcik and Open Resources for Nursing is licensed under a Creative Commons Attribution 4.0 International License , except where otherwise noted.
Share This Book

Want to create or adapt books like this? Learn more about how Pressbooks supports open publishing practices.
3.2 Communication
Effective communication is a vital component of proper assignment, delegation, and supervision. It is also one of the Standards of Professional Performance established by the American Nurses Association (ANA). [1]
Consider the fundamentals of good communication practices. Effective communication requires each interaction to include a sender of the message, a clear and concise message, and a receiver who can decode and interpret that message. The receiver also provides a feedback message back to the sender in response to the received message. See Figure 3.1 [2] for an image of effective communication between a sender and receiver. This feedback message is referred to as closed-loop communication in health care settings. Closed-loop communication enables the person giving the instructions to hear what they said reflected back and to confirm that their message was received correctly. It also allows the person receiving the instructions to verify and confirm the actions to be taken. If closed-loop communication is not used, the receiver may nod or say “OK,” and the sender may assume the message has been effectively transmitted, but this may not be the case and can lead to errors and client harm.
An example of closed-loop communication can be found in the following exchange:
- RN: “Jane, can you get a set of vitals on Mr. Smith and let me know if the results are outside of normal range?”
- Jane, CNA: “OK, I’ll get a set of vitals on Mr. Smith and let you know if they are out of range.”
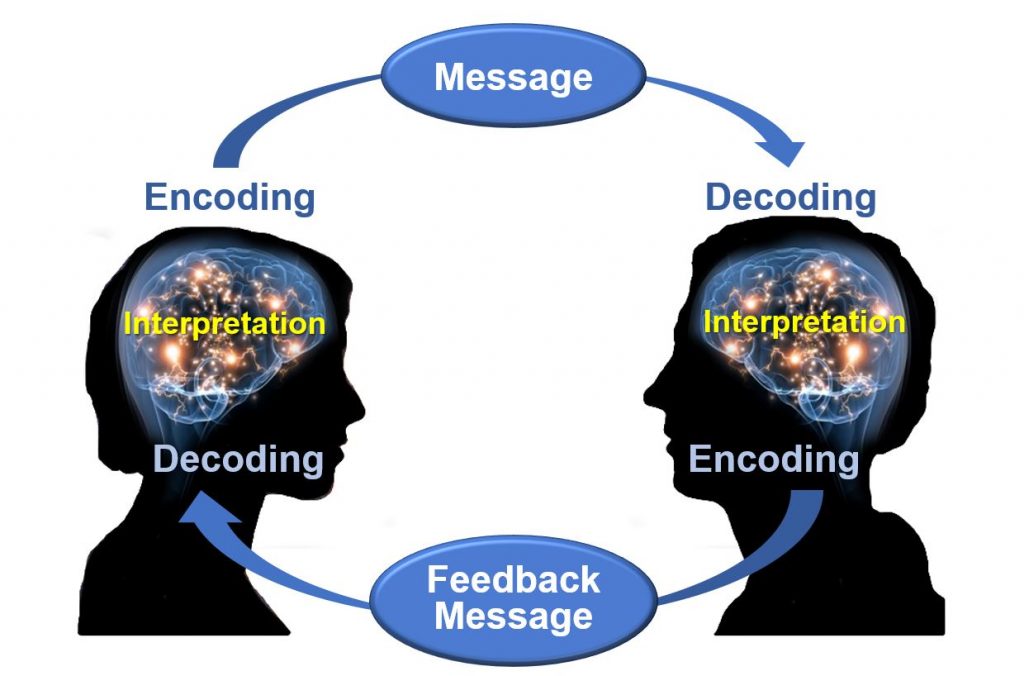
Closed-loop communication is vital for communication among health care team members to avoid misunderstandings that can cause unsafe client care. According to the HIPAA Journal , poor communication leads to a “reduction in the quality of care, poor client outcomes, wastage of resources, and high health care costs.” [3] Parameters for reporting results and the results that should be expected are often left unsaid rather than spelled out in sufficient detail. It is imperative for the RN to provide clear, complete, concise instructions when delegating. A lack of clarity can lead to misunderstanding, unfinished tasks, incomplete care, and/or medical errors. [4]
Effective communication is at the core of proper assignment, delegation, and supervision. With effective communication at the beginning of every shift, each nursing team member should have a clear plan for their shift, what to do and why, and what and when to report to the RN or team leader. Communication should continue throughout the shift as tasks are accomplished and patients’ needs change. Effective communication improves client outcomes and satisfaction scores, as well as improving team morale by enhancing the collaborative relationships of the health care team.
The RN is accountable for clear, concise, correct, and complete communication when making assignments and delegating, both initially and throughout the shift. These communication characteristics can be remembered by using the mnemonic the “4 Cs”:
- Clear: Information is understood by the listener. Asking the listener to restate the instructions and the plan can be helpful to determine whether the communication is clear.
- Concise: Sufficient information should be provided to accurately perform the task, but excessive or irrelevant information should be avoided because it can confuse the listener and waste precious time.
- Correct: Correct communication is not vague or confusing. Accurate information is also aligned with agency policy and the team member’s scope of practice as defined by their state’s Nurse Practice Act and other state regulations.
- Complete: Complete instructions leave no room for doubt. Always ask if further information or clarification is needed, especially regarding tasks that are infrequently performed or include unique instructions. [5]
The use of closed-loop communication is the best method to achieve clear, concise, correct, and complete information exchanged among team members. Closed-loop communication allows team members the opportunity to verify and validate the exchange of information. By repeating back information, members confirm the exchange has occurred, understanding is clear, and expectations are heard.
Closed-loop communication should also be used when the RN is receiving a verbal order from a provider. For example, when the resuscitation team leader gives a verbal order of “Epinephrine 1 mg/mL IV push now,” the RN confirms correct understanding of the order by repeating back, “I will prepare Epinephrine 1 mg/mL to be given IV push now.” After the provider confirms the verbal order and the task is completed, the nurse confirms completion of the task by stating, ““Epinephrine 1 mg/mL IV push was administered.”
In addition to using closed-loop communication, a common format used by health care team members to exchange client information is ISBARR, a mnemonic for the components of I ntroduction, S ituation, B ackground, A ssessment, R equest/Recommendations, and R epeat Back. ISBARR and other communication strategies are discussed in more detail in the “ Interprofessional Communication ” section of the “Collaboration Within the Interprofessional Team” chapter.
- American Nurses Association. (2021). Nursing: Scope and standards of practice (4th ed.). American Nurses Association. ↵
- “Osgood-Schramm-model-of-communication.jpg“ by Jordan Smith at eCampus Ontario is licensed under CC BY 4.0 . Access for free at https://ecampusontario.pressbooks.pub/communicationatwork/chapter/1-3-the-communication-process/ ↵
- HIPAA Journal. (n.d.). Effects of poor communication in healthcare. https://www.hipaajournal.com/effects-of-poor-communication-in-healthcare/ ↵
- LaCharity, L. A., Kumagai, C. K., & Bartz, B. (2019). Prioritization, delegation and assignment (4th ed.). Mosby, p. 6. ↵
A process that enables the person giving the instructions to hear what they said reflected back and to confirm that their message was, in fact, received correctly.
Nursing Management and Professional Concepts Copyright © by Chippewa Valley Technical College is licensed under a Creative Commons Attribution 4.0 International License , except where otherwise noted.
Share This Book

Home / NCLEX-RN Exam / Assignment, Delegation and Supervision: NCLEX-RN
Assignment, Delegation and Supervision: NCLEX-RN
Identifying tasks for delegation based on client needs, the "right task" and the "right person": identifying tasks for delegation based on client needs, ensuring the appropriate education, skills, and experience of personnel performing delegated tasks, assigning and supervising the care provided by others, communicating tasks to be completed and report client concerns immediately, organizing the workload to manage time effectively, utilizing the five rights of delegation, evaluating delegated tasks to ensure the correct completion of the activity or activities, evaluating the ability of staff members to perform the assigned tasks for the position, evaluating the effectiveness of staff members' time management skills.
In this section of the NCLEX-RN examination, you will be expected to demonstrate your knowledge and skills of assignment, delegation, and supervision in order to:
- Identify tasks for delegation based on client needs
- Ensure appropriate education, skills, and experience of personnel performing delegated tasks
- Assign and supervise care provided by others (e.g., LPN/VN, assistive personnel, other RNs)
- Communicate tasks to be completed and report client concerns immediately
- Organize the workload to manage time effectively
- Utilize the five rights of delegation (e.g., right task, right circumstances, right person, right direction or communication, right supervision or feedback)
- Evaluate delegated tasks to ensure correct completion of activity
- Evaluate the ability of staff members to perform assigned tasks for the position (e.g., job description, scope of practice, training, experience)
- Evaluate the effectiveness of staff members' time management skills
The assignment of care to others, including nursing assistants, licensed practical nurses, and other registered nurses, is perhaps one of the most important daily decisions that nurses make.
Proper and appropriate assignments facilitate quality care. Improper and inappropriate assignments can lead to poor quality of care, disappointing outcomes of care, the jeopardization of client safety, and even legal consequences.
For example, when a registered nurse delegates aspects of patient care to a licensed practical nurse that are outside of the scope of practice of the licensed practical nurse, the client is in potential physical and/or psychological jeopardy because this delegated task, which is outside of the scope of practice for this licensed practical nurse, is something that this nurse was not prepared and educated to perform. This practice is also illegal and it is considered practicing outside of one's scope of practice when, and if, this licensed practical nurse accepts this assignment. All levels of nursing staff should refused to accept any assignment that is outside of their scope of practice.
- How is the Scope of Practice Determined for a Nurse?
- Scope of Practice vs Scope of Employment
- RN Scope of Practice
Delegation, simply defined, is the transfer of the nurse's responsibility for the performance of a task to another nursing staff member while retaining accountability for the outcome. Responsibility can be delegated. Accountability cannot be delegated. The delegating registered nurse remains accountable for all client care despite the fact that some of these aspects of care can, and are, delegated to others.
Appropriate decisions relating to the successful assignment of care are accurately based on the needs of the patient, the skills of the staff, the staffs' position description or job descriptions, the employing facility's policies and procedures, and legal aspects of care such as the states' legal scopes of practice for nurses, nursing assistants and other members of the nursing team.
The " Five Rights of Delegation " that must be used when assigning care to others are:
- The "right" person
- The "right" task
- The "right" circumstances
- The "right" directions and communication and
- The "right" supervision and evaluation
In other words, the right person must be assigned to the right tasks and jobs under the right circumstances. The nurse who assigns the tasks and jobs must then communicate with and direct the person doing the task or job. The nurse supervises the person and determines whether or not the job was done in the correct, appropriate, safe and competent manner.
The client is the center of care. The needs of the client must be competently met with the knowledge, skills and abilities of the staff to meet these needs. In other words, the nurse who delegates aspects of care to other members of the nursing team must balance the needs of the client with the abilities of those to which the nurse is delegating tasks and aspects of care, among other things such as the scopes of practice and the policies and procedures within the particular healthcare facility.
Some client needs are relatively predictable; and other patient needs are unpredictable as based on the changing status of the client. Some needs require high levels of professional judgment and skill; and other patient needs are somewhat routinized and without the need for high levels of professional judgment and skill. Some client needs are acute, ever changing and/or rarely encountered; and other patient needs are chronic, relatively stable, more predictable, and more frequently encountered.
Based on these characteristics and the total client needs for the group of clients that the registered nurse is responsible and accountable for, the registered nurse determines and analyzes all of the health care needs for a group of clients; the registered nurse delegates care that matches the skills of the person that the nurse is delegating to.
For example, a new admission who is highly unstable should be assigned to a registered nurse; the care of a stable chronically ill patient who is relatively stable and more predictable than a serious ill and unstable acute client can be delegated to the licensed practical nurse; and assistance with the activities of daily living and basic hygiene and comfort care can be assigned and delegated to an unlicensed assistive staff member like a nursing assistant or a patient care technician. Lastly, the care of a client with chest tubes and chest drainage can be delegated to either another registered nurse or a licensed practical nurse, therefore, the registered nurse who is delegating must insure that the nurse is competent to perform this complex task, to monitor the client's response to this treatment, and to insure that the equipment is functioning properly.
The staff members' levels of education, knowledge, past experiences, skills, abilities, and competencies are also evaluated and matched with the needs of all of the patients in the group of patients that will be cared for. Some staff members may possess greater expertise than others. Some, such as new graduates, may not possess the same levels of knowledge, past experiences, skills, abilities, and competencies that more experienced staff members possess. Some may even be more competent in some aspects of client care than other aspects of client care. For example, a licensed practical nurse on the medical surgical floor may have more knowledge, skills, abilities, and competencies than a registered nurse in terms of chest tube maintenance and care because they may have, perhaps, had years of prior experience in an intensive care area of another healthcare facility before coming to your nursing care facility.
Delegation should be done according to the differentiated practice for each of the staff members. A patient care technician, a certified nursing assistant, a licensed practical nurse, an associate degree registered nurse and a bachelor's degree registered nurse should not be delegated to the same aspects of nursing care. Based on the basic entry educational preparation differences among these members of the nursing team, care should be assigned according to the level of education of the particular team member.
Also, staff members differ in terms of their knowledge, skills, abilities and competencies. A staff member who has just graduated as a certified nursing assistant and a newly graduated registered nurse cannot be expected to perform patient care tasks at the same level of proficiency, skill and competency as an experienced nursing assistant or registered nurse. It takes time for new graduates to refine the skills that they learned in school.
Validated and documented competencies must also be considered prior to assignment of patient care. No aspect of care can be assigned or delegated to another nursing staff member unless this staff member has documented evidence that they are deemed competent by a registered nurse to do so. For example, a newly hired certified nursing assistant cannot perform bed baths until a supervising registered nurse has observed this certified nursing assistant provide a bed bath and has decided that they are now competent to do this task without direct supervision.
All healthcare facilities and agencies must assess and validate competency before total care or any aspect of care is performed by an individual without the direct supervision of another, regardless of their years of experience. Competency checklists are used to document the competency of the staff; they must be referred to as assignments are made. Care can be delegated to another only when that person is deemed competent to perform the role or task and this competency is documented.
Scopes of practice are also considered prior to the assignment of care. All states have scopes of practice for advanced nurse practitioners, registered nurses, licensed practical nurses and unlicensed assistive personnel like nursing assistants and patient care technicians.
The job of the registered nurse is far from done after client care has been delegated to members of the nursing team. The delegated care must be followed up on and the staff members have to be supervised as they deliver care. The registered nurse remains responsible for and accountable for the quality, appropriateness, completeness, and timeliness of all of the care that is delivered.
The supervision of the care provided by others includes the monitoring the care, coaching and supporting the staff member who is providing the care, assisting the staff member with priority setting and time management skills, as indicated, educating the staff member about the proper provision of care, as indicated by a knowledge or skills deficit, and also praising and positively reinforcing the staff for a job well done.
Remember, the delegating registered nurse is still responsible and accountable for all of the client care that is delegated to others.
Registered nurses who assign, delegate and/or provide nursing care to clients and groups of clients must report all significant changes that occur in terms of the client and their condition. For example, a significant change in a client's laboratory values requires that the registered nurse report this to the nurse's supervisor and doctor.
They must also communicate and document all tasks that were completed and the client's responses to this treatment. As the old adage says, "If it wasn't documented, it wasn't done."
Time is finite and often the needs of the client are virtually infinite. Time management, organization, and priority setting skills, therefore, are essential to the complete and effective provision of care to an individual client and to a group of clients.
Priorities of care, as previously discussed, are established using a number of methods and frameworks including the ABCs, Maslow's Hierarchy of Needs and the ABCs/MAAUAR method of priority setting.
Some time management techniques, in addition to priority setting, that you may want to consider using to insure that you manage your workload and time effectively include:
- Clarifying your assignment as necessary
- Planning your work in an orderly and systematic manner knowing that priorities and clients' status change frequently
- Avoiding all unnecessary interruptions
- Learning how to say no to others when they ask you for help and you have priority patient needs that would not be addressed if you helped another
As previously discussed, all delegation may be based on the "Five Rights of Delegation" which are:
- The "right" directions and communication
In addition to the supervision of delegated tasks in terms of quality, appropriateness, and timeliness, the registered nurse who has delegated tasks must insure that the assigned activities have been correctly completed.
When assignments are made, the registered nurse must insure that the staff member will have ample time during the shift to complete the assignment and, then, the registered nurse must monitor and measure the staff members' progress toward the completion of assigned tasks throughout the duration of the shift.
This monitoring must be done in an ongoing and continuous manner and not at the end of the shift when it is too late to make corrections.
As previously discussed, staff members should have documented competency for all tasks that are assigned to them. All nursing team members have the responsibility, however, to refuse an assignment if they believe that they cannot do it properly. When this occurs, the registered nurse should either teach the staff member how to perform the task and then document their competency in terms of this assigned task or assign the task to another nursing team member who has documented competency and is sure that they can perform the task in a correct manner.
Part of supervision entails the ongoing evaluation of staff's ability by the registered nurse to perform assigned tasks using direct observations and with indirect observations of patient safety, the quality of the care provided, the appropriateness of care provided, and the timeliness of care provided. For example, the registered nurse can directly observe the performance of the nursing assistant while the client is being transferred from the bed to the chair; and the registered nurse can review the medication administration record to determine if the licensed practical nurse has administered medications in a timely manner which is an example of indirect observation.
The ability of a staff member to perform a specific task is not only based on their competency but it is also based on their:
- Legal scope of practice,
- Documented competency,
- Education and training,
- Past experiences,
- Position description which is also referred to as the job description and
- Healthcare facility specific policies and procedures.
All states throughout our nation have legally legislated scopes of practice for registered professional nurses, licensed practical or vocational nurses, and advanced nursing practice nurses; and they also have legal guidelines related to what an unlicensed, assistive staff member, such as a student nurse technician, patient care aide, patient care technician or nursing assistant, can and cannot legally perform regardless of whether or not the healthcare provider or the delegating nurse believes that they are competent to do.
Although these legal, legislated scopes of practice may vary a little from state to state, they share a lot of commonalities and similarities. For example:
- The scope of practice for the registered nurse will most likely include the legal ability of the registered professional nurse to perform all phases of the nursing process including assessment, nursing diagnosis, planning, implementation and evaluation.
- The scope of practice for the licensed practical or vocational nurse will most likely include the legal ability of this nurse to perform data collection, plan, implement and evaluate care under the direct supervision and guidance of the registered nurse.
- The scope of practice for an advanced practice nurse, such as a nurse practitioner, will most likely include the legal ability of the advanced practice registered professional nurse to perform all phases of the nursing process including assessment, nursing diagnosis, planning, implementation and evaluation in addition to prescribing some medications.
Nurses violate scope of practice statutes, or laws, when they function in roles and aspects of care that are above, beyond and/or not included in their scope of practice. Permanent license revocation may occur when a nurse practices outside of the legally mandated scope of practice. Additionally, licensed nurses who have failed to either reapply for their license or have had it revoked as part of a state disciplinary action cannot and continue to practice nursing are guilty of practicing nursing without a license.
Among the tasks that CANNOT be legally and appropriately delegated to nonprofessional, unlicensed assistive nursing personnel, such as nursing assistants, patient care technicians, and personal care aides, include assessments, nursing diagnosis, establishing expected outcomes, evaluating care and any and all other tasks and aspects of care including but not limited to those that entail sterile technique, critical thinking, professional judgment and professional knowledge.
Some examples of tasks and aspects of care that can be delegated legally to nonprofessional, unlicensed assistive nursing personnel, provided they are competent in these areas, under the direct supervision of the nurse include:
- Assisting the client with their activities of daily living such as ambulation, dressing, grooming, bathing and hygiene
- Measuring and recording fluid intake and output
- Measuring and recording vital signs, height and weight
- The provision of nonpharmacological comfort and pain relief interventions such as establishing and maintaining an environment conducive to comfort and providing the client with a soothing and therapeutic back rub
- Observation and reporting changes in and the current status of the patient’s condition and reactions to care
- The transport of clients and specimens and other errands and tasks such as stocking supplies
- Assistance with transfers, range of motion, feeding, ambulation, and other tasks such as making beds and assisting with bowel and bladder functions
In addition to the legally mandated state scopes of practice, the registered nurse must also insure that the delegated tasks are permissible according to the nursing team members' position description which is also referred to as the job description, and the particular facility's specific policies and procedures relating to client care and who can and who cannot perform certain tasks.
For example, intravenous bolus and push medications may be permissible for only licensed registered nurses in certain areas of the healthcare facility such as the intensive care units; the administration of blood and blood components may be restricted to only registered nurses; and the care of a client who is receiving conscious sedation may be restricted to only a few registered nurses in the particular healthcare facility, according to these job descriptions, policies and procedures.
As previously mentioned, the registered nurse must allot a reasonable amount of time for staff members to complete their assignments when care and tasks are delegated. The staff should be able to complete their assignments within the allocated period of time. When an assignment is not done as expected, the delegating nurse should determine why this has occurred and they must take corrective actions to insure task completion.
One of the things that the delegating nurse will want to consider when an assignment is not completed within the allotted time frame is determining whether or not the staff member is organizing their work and using effective time management skills. If the staff member is not using effective time management skills, the nurse must teach and assist the staff member about better time management and priority setting skills.
RELATED NCLEX-RN MANAGEMENT OF CARE CONTENT:
- Advance Directives
- Assignment, Delegation and Supervision (Currently here)
- Case Management
- Client Rights
- Collaboration with Interdisciplinary Team
- Concepts of Management
- Confidentiality/Information Security
- Continuity of Care
- Establishing Priorities
- Ethical Practice
- Informed Consent
- Information Technology
- Legal Rights and Responsibilities
- Performance Improvement & Risk Management (Quality Improvement)
SEE – Management of Care Practice Test Questions
- Recent Posts

The Ultimate Guide to Nursing Assignments: 7 Tips and Strategies
Nursing assignments are a critical component of every nursing student’s academic journey. They serve as opportunities to test your knowledge, apply theoretical concepts to real-world scenarios, and develop essential skills necessary for your future nursing career. However, tackling nursing assignments can often be overwhelming, particularly when you’re juggling multiple responsibilities. In this comprehensive guide, we provide valuable tips, strategies, and expert assignment help services to help you excel in your nursing assignments. Whether you’re struggling with research, structuring your assignment, or proofreading, we’re here to support you every step of the way.
Understanding the Nursing Assignments
To excel in nursing assignments , it’s crucial to start by thoroughly understanding the requirements. Take the time to carefully read the assignment prompt, paying close attention to the topic, word count, formatting guidelines, and any specific instructions provided by your instructor. Understanding these key components will ensure that you meet all the necessary criteria.

Conducting Thorough Research
Once you have a clear understanding of the assignment, it’s time to conduct thorough research. Solid research forms the foundation of any successful nursing assignment. Begin by gathering relevant and credible sources, such as nursing textbooks, scholarly articles, reputable websites , and academic databases specific to nursing. These resources will provide you with evidence-based information to support your arguments and demonstrate your understanding of the topic.
Creating a Well-Structured Outline
A well-structured outline is essential for organizing your thoughts and ensuring a logical flow in your nursing assignment. An effective outline acts as a roadmap, guiding you through the writing process and ensuring that you cover all the necessary points.
At [Your Service Name], our expert writers can assist you in creating a comprehensive outline tailored to your specific assignment. By collaborating with us, you can receive personalized guidance in organizing your ideas effectively and structuring your assignment in a logical manner. Our writers understand the nuances of nursing assignments and can help you identify the most important concepts and supporting evidence to include.
Using a Professional Tone
Maintaining a professional tone throughout your nursing assignment is crucial. As aspiring healthcare professionals, it’s essential to communicate your ideas with clarity, conciseness, and professionalism. Use clear and concise language, avoiding jargon or slang that may hinder the reader’s understanding. Present your arguments and supporting evidence in a logical and coherent manner, demonstrating your ability to think critically and apply nursing principles.
Our expert writers have extensive experience in academic writing within the field of nursing. They possess a deep understanding of the professional tone required for nursing assignments and can ensure that your assignment is written to the highest standards. By collaborating with us, you can receive guidance in maintaining a professional tone and effectively conveying your ideas.

Incorporating Practical Examples
In addition to a professional tone, incorporating practical examples into your nursing assignment can greatly enhance its quality. Practical examples bring theoretical concepts to life, illustrating their application in real-life scenarios. They demonstrate your understanding of nursing principles and showcase your ability to bridge the gap between theory and practice.
Our team consists of experienced nursing professionals who can assist you in incorporating relevant practical examples into your assignment. Drawing from their extensive knowledge and expertise, they can provide you with real-life scenarios or case studies that strengthen the impact and credibility of your work. By collaborating with us, you can elevate the quality of your assignment by demonstrating your ability to apply nursing concepts in practical settings.
Proofreading and Editing
Proofreading and editing are essential steps in the assignment writing process. They ensure that your nursing assignment is polished, error-free, and effectively communicates your ideas. After completing the initial draft, it’s crucial to take a break and return to your work with fresh eyes. During the proofreading stage, carefully review your assignment for grammar, spelling, punctuation, and sentence structure. Correct any errors and inconsistencies that may affect the clarity and professionalism of your writing.
At nursingresearchhelp.com , we have a dedicated team of proofreaders and editors who specialize in nursing assignments. They meticulously review your work, ensuring that it adheres to formatting guidelines and meets the highest standards of academic writing. Our proofreaders and editors will help you refine your assignment, ensuring that it is polished and error-free. By collaborating with us, you can rest assured that your assignment will be thoroughly reviewed and refined before submission.
Seeking Help When Needed
In addition to proofreading and editing, it’s important to seek help when needed. Nursing assignments can be challenging, and it’s perfectly normal to require assistance. Whether you’re facing difficulties in understanding the assignment prompt, need guidance in specific areas, or simply want a fresh perspective on your work, don’t hesitate to reach out for support.
Our friendly and knowledgeable support team is always available to address any questions or concerns you may have. We understand the unique challenges faced by nursing students and can provide you with the guidance and clarification you need. By seeking help when needed, you can overcome obstacles and ensure the successful completion of your nursing assignments.

Mastering nursing assignments is within your reach with the right tips, strategies, and expert assignment help services. At nursingresearchhelp.com we are committed to supporting nursing students in excelling in their academic pursuits. Our experienced writers, proofreaders, and editors can provide personalized assistance throughout the assignment writing process, ensuring that your assignments meet the highest standards of quality and professionalism.
With our help, you can confidently tackle your nursing assignments and overcome any challenges you may face. Visit our website nursingresearchhelp.com to learn more about our services and how we can support you in achieving academic excellence. Whether you need guidance in understanding the assignment, conducting thorough research, creating a well-structured outline, using a professional tone, incorporating practical examples, or ensuring a polished final product, we are here to assist you. Trust us for reliable and professional assignment help tailored to your needs.
Don’t let the challenges of nursing assignments hold you back—reach out to us for reliable and professional assignment help tailored to your needs.
You might also like

Nursingresearchhelp.com is the fastest, easiest and most reliable way to have content written for your website. You’ll be able to post a project and 1000s of freelance writers from across the globe will have instant access to write your content quickly, professionally, and affordably.
QUICK LINKS
- HOW IT WORKS
- OUR SERVICES
- TERMS OF USE

Call/Text: +1 608 912 3884


- Walden University
- Faculty Portal
Common Assignments: Writing in Nursing
Although there may be some differences in writing expectations between disciplines, all writers of scholarly work are required to follow basic writing standards such as writing clear, concise, and grammatically correct sentences; using proper punctuation; demonstrating critical thought; and, in all Walden programs, using APA style. When writing in nursing, however, students must also be familiar with the goals of the discipline and discipline-specific writing expectations.
Nurses are primarily concerned about providing quality care to patients and their families, and this demands both technical knowledge and the appropriate expression of ideas (“Writing in nursing,” n.d). As a result, nursing students are expected to learn how to present information succinctly, and even though they may often use technical medical terminology (“Writing in nursing,” n.d.), their work should be accessible to anyone who may read it. Among many goals, writers within this discipline are required to:
- Document knowledge/research
- Demonstrate critical thinking
- Express creative ideas
- Explore nursing literature
- Demonstrate understanding of learning activities. (Wagner, n.d., para. 2)
Given this broad set of objectives, nursing students would benefit from learning how to write diverse literature, including scholarly reports, reviews, articles, and so on. They should aim to write work that can be used in both the research and clinical aspects of the discipline. Walden instructors often ask nursing students to write position and reflective papers, critique articles, gather and analyze data, respond to case studies, and work collaboratively on a project. Although there may be differences between the writing expectations within the classroom and those in the workplace, the standards noted below, though more common in scholarly writing, require skills that are transferrable to the work setting.
Because one cannot say everything there is to say about a particular subject, writers present their work from a particular perspective. For instance, one might choose to examine the shortage of nurses from a public policy perspective. One’s particular contribution, position, argument, or viewpoint is commonly referred to as the thesis and, according to Gerring et al. (2004), a good thesis is one that is “new, true, and significant” (p. 2). To strengthen a thesis, one might consider presenting an argument that goes against what is currently accepted within the field while carefully addressing counterarguments and adequately explaining why the issue under consideration matters (Gerring et al., 2004). The thesis is particularly important because readers want to know whether the writer has something new or worthwhile to say about the topic. Thus, as you review the literature, before writing, it is important to find gaps and creative linkages between viewpoints with the goal of contributing innovative ideas to an ongoing discussion. For a contribution to be worthwhile you must read the literature carefully and without bias; doing this will enable you to identify some of the subtle differences in the viewpoints presented by different authors and help you to better identify the gaps in the literature. Because the thesis is essentially the heart of your discussion, it is important that it is argued objectively and persuasively.
With the goal of providing high quality care, the healthcare industry places a premium on rigorous research as the foundation for evidence-based practices. Thus, students are expected to keep up with the most current research in their field and support the assertions they make in their work with evidence from the literature. Nursing students also must learn how to evaluate evidence in nursing literature and identify the studies that answer specific clinical questions (Oermann & Hays, 2011). Writers are also expected to critically analyze and evaluate studies and assess whether findings can be used in clinical practice (Beyea & Slattery, 2006). (Some useful and credible sources include journal articles, other peer-reviewed sources, and authoritative sources that might be found on the web. If you need help finding credible sources contact a librarian.)
Like other APA style papers, research papers in nursing should follow the following format: title, abstract, introduction, literature review, method, results, discussion, references, and appendices (see APA 7, Sections 2.16-2.25). Note that the presentation follows a certain logic: In the introduction one presents the issue under consideration; in the literature review, one presents what is already known about the topic (thus providing a context for the discussion), identifies gaps, and presents one’s approach; in the methods section, one would then identify the method used to gather data; and in the results and discussion sections, one then presents and explains the results in an objective manner, noting the limitations of the study (Dartmouth Writing Program, 2005). Note that not all papers need to be written in this manner; for guidance on the formatting of a basic course paper, see the appropriate template on our website.
In their research, nursing researchers use quantitative, qualitative, or mixed methods. In quantitative studies, researchers rely primarily on quantifiable data; in qualitative studies, they use data from interviews or other types of narrative analyses; and in mixed methods studies, they use both qualitative and quantitative approaches. A researcher should be able to pose a researchable question and identify an appropriate research method. Whatever method the researcher chooses, the research must be carried out in an objective and scientific manner, free from bias. Keep in mind that your method will have an impact on the credibility of your work, so it is important that your methods are rigorous. Walden offers a series of research methods courses to help students become familiar with the various research methods.
Instructors expect students to master the content of the discipline and use discipline- appropriate language in their writing. In practice, nurses may be required to become familiar with standardized nursing language as it has been found to lead to the following:
- better communication among nurses and other health care providers,
- increased visibility of nursing interventions,
- improved patient care,
- enhanced data collection to evaluate nursing care outcomes,
- greater adherence to standards of care, and
- facilitated assessment of nursing competency. (Rutherford, 2008)
Like successful writers in other disciplines and in preparation for diverse roles within their fields, in their writing nursing students should demonstrate that they (a) have cultivated the thinking skills that are useful in their discipline, (b) are able to communicate professionally, and (c) can incorporate the language of the field in their work appropriately (Colorado State University, 2011).
If you have content-specific questions, be sure to ask your instructor. The Writing Center is available to help you present your ideas as effectively as possible.
Beyea, S. C., & Slattery, M. J. (2006). Evidence-based practice in nursing: A guide to successful implementation . http://www.hcmarketplace.com/supplemental/3737_browse.pdf
Colorado State University. (2011). Why assign WID tasks? http://wac.colostate.edu/intro/com6a1.cfm
Dartmouth Writing Program. (2005). Writing in the social sciences . http://www.dartmouth.edu/~writing/materials/student/soc_sciences/write.shtml
Rutherford, M. (2008). Standardized nursing language: What does it mean for nursing practice? [Abstract]. Online Journal of Issues in Nursing , 13 (1). http://ojin.nursingworld.org/MainMenuCategories/ThePracticeofProfessionalNursing/Health-IT/StandardizedNursingLanguage.html
Wagner, D. (n.d.). Why writing matters in nursing . https://www.svsu.edu/nursing/programs/bsn/programrequirements/whywritingmatters/
Writing in nursing: Examples. (n.d.). http://www.technorhetoric.net/7.2/sectionone/inman/examples.html
Didn't find what you need? Search our website or email us .
Read our website accessibility and accommodation statement .
- Previous Page: Collaborative Writing in Business & Management
- Next Page: Learning Agreements (LAs)
- Office of Student Disability Services
Walden Resources
Departments.
- Academic Residencies
- Academic Skills
- Career Planning and Development
- Customer Care Team
- Field Experience
- Military Services
- Student Success Advising
- Writing Skills
Centers and Offices
- Center for Social Change
- Office of Academic Support and Instructional Services
- Office of Degree Acceleration
- Office of Research and Doctoral Services
- Office of Student Affairs
Student Resources
- Doctoral Writing Assessment
- Form & Style Review
- Quick Answers
- ScholarWorks
- SKIL Courses and Workshops
- Walden Bookstore
- Walden Catalog & Student Handbook
- Student Safety/Title IX
- Legal & Consumer Information
- Website Terms and Conditions
- Cookie Policy
- Accessibility
- Accreditation
- State Authorization
- Net Price Calculator
- Contact Walden
Walden University is a member of Adtalem Global Education, Inc. www.adtalem.com Walden University is certified to operate by SCHEV © 2024 Walden University LLC. All rights reserved.

IMAGES
VIDEO
COMMENTS
Determine the # of nursing care hours needed/patient. Generating the full time equivalents of an employee. Determine the nurse-patient ratio in providing nursing care. FTE - measure of work committed of full time employee. 1.0 FTE = works 5 days/week, 8 hours/day. 0.5 FTE = part time employee who works 5 days/2 weeks.
Delivering safe, quality client care often requires registered nurses (RN) to manage care provided by the nursing team. Making assignments, delegating tasks, and supervising nursing team members are essential managerial components of an entry-level staff RN role. As previously discussed, nursing team members include RNs, licensed practical/vocational nurses (LPN/VN), and assistive personnel ...
Compare and contrast the role of a leader and a manager. Examine the roles of team members. Identify the activities managers perform. Describe the role of the RN as a leader and change agent. Evaluate the effects of power, empowerment, and motivation in leading and managing a nursing team. Recognize limitations of self and others and utilize ...
Module 4 Assignment Org Analysis The Nurse Leader. Assignments None. 5. M1 - 4455- M1 - 5 questions. Assignments 100% (5) 7. N4455 Module 3 Assignment Financial Management Su23 (1) On Campus-1. Assignments 0% (1) 3.
Learning Objectives. Compare and contrast the role of a leader and a manager. Examine the roles of team members. Identify the activities managers perform. Describe the role of the RN as a leader and change agent. Evaluate the effects of power, empowerment, and motivation in leading and managing a nursing team.
3.3 Assignment. Nursing team members working in inpatient or long-term care settings receive patient assignments at the start of their shift. Assignment refers to routine care, activities, and procedures that are within the legal scope of practice of registered nurses (RN), licensed practical/vocational nurses (LPN/VN), or assistive personnel ...
The health care system faces a significant challenge in balancing the ever-expanding task of meeting patient care needs with scarce nursing resources that has even worsened as a result of the COVID-19 pandemic. With a limited supply of registered nurses, nurse managers are often challenged to implement creative staffing practices such as sending staff to units where they do not normally work ...
Rosanne Raso is the editor-in-chief of Nursing Management and the vice president and CNO at NewYork-Presbyterian/Weill Cornell in New York, N.Y. Joyce Fitzpatrick is the director of the Marian K. Shaughnessy Nurse Leadership Academy and Elizabeth Brooks Ford professor of nursing at Case Western Reserve University Frances Payne Bolton School of Nursing in Cleveland, Ohio.
Manage priorities. A good nurse manager has plenty of tasks but often needs more time. Strong organizational and time management skills — and the ability to streamline processes and delegate appropriate tasks — help to improve efficiency and empower your staff. Embrace change. Health care is constantly changing.
Nursing Management (Springhouse) 51(6):p 17-20, June 2020. | DOI: 10.1097/01.NUMA.0000662704.97080.df. Free; Metrics Abstract. ... Nurses are facing patient assignments that were unfathomable weeks ago as new blueprints to organize patient care are now created in real time, often with unfamiliar coworkers. ...
3.3 Assignment Nursing team members receive assignments at the start of their shift. Assignment refers to routine care, activities, and procedures that are within the authorized scope of practice of the RN or LPN/VN or routine functions of the assistive personnel. [1] Assistive personnel (AP) are defined as certified nursing assistants (CNA), client care technicians (PCT), certified medical ...
3.2 Communication. Effective communication is a vital component of proper assignment, delegation, and supervision. It is also one of the Standards of Professional Performance established by the American Nurses Association (ANA). [1]
Evaluate the effectiveness of staff members' time management skills; The assignment of care to others, including nursing assistants, licensed practical nurses, and other registered nurses, is perhaps one of the most important daily decisions that nurses make. Proper and appropriate assignments facilitate quality care.
It has clues to the information you need. It provides the framework for the assignment-making process, including staff constraints, additional duties that must be covered, and patient factors most impor-tant on your unit. Use the electronic health record (EHR) to generate various useful pieces of patient in-formation.
Nursing Management has been awarded a 2021 Association for Women in Communications' Clarion Award for Best Overall External Magazine - Circulation of 100,000 or less (November 2020 and December 2020 issues).. Nursing Management has been awarded a 2022 APEX Award of Excellence for Magazines, Journals & Tabloids—Writing (Entire Issue) for the November 2021 Safety Solutions issue.
6. NRS 451VN Week 2 Benchmark, Effective Approaches in Leadership and Management - Nurse Staffing Ratios. Assignments 50% (2) 8. Benchmark - Effective Approaches in Leadership and Management. Assignments None. 7. Healthcare organizations evaluation. Coursework None.
The Ultimate Guide to Nursing Assignments: 7 Tips and Strategies. Nursing assignments are a critical component of every nursing student's academic journey. They serve as opportunities to test your knowledge, apply theoretical concepts to real-world scenarios, and develop essential skills necessary for your future nursing career.
In the dynamic and demanding field of nursing, students often find themselves grappling with complex assignments that require a deep understanding of healthcare management principles. This blog ...
Step 1: Make a List of Everything You Need to Keep Track Of. Lists can help you figure out what tools you might need. For example, you might need a more detailed and customized planner if you want to keep track of things like classes, assignments, exams, clinicals, and extracurricular activities.
Delegate tasks to unlicensed assistive personnel (UAP). Identify tasks needed for assignment and delegation. Assign clients to staff nurses according to acuity. Inspect the code cart equipment and supplies. As the charge nurse considers the unit assignments and tasks for the day, they thinks about the evidence-based guidelines for delegation.
UMB NU371 NURS371 NU 371 Evidence-Based Nursing Practice (UMB UMass Boston, Fall 2021) HESI Delegation of Nursing Management ... · Making client assignments is a charge nurse action that must be performed before or during the first hour of the shift to make the best use of unit personnel resources. o Inspect the code cart equipment and supplies.
1. PATIENT ASSIGNMENTPATIENT ASSIGNMENT. 2. 3. Specific objectives: At the end of this topic the student will be able to: Clarify purposes of nursing assignment. Identify principles of nursing assignment. Determine factors to be considered in distributing duties. Differentiate between different methods of nursing assignment. 4. 5.
Walden instructors often ask nursing students to write position and reflective papers, critique articles, gather and analyze data, respond to case studies, and work collaboratively on a project. Although there may be differences between the writing expectations within the classroom and those in the workplace, the standards noted below, though ...